
This blog post is part of a series featuring new articles published in the LCNTDR Collection: Advances in scientific research for NTD control, led by the London Centre for Neglected Tropical Disease Research (LCNTDR). Stay tuned for updates on Twitter @bugbittentweets and @NTDResearch. You can find other posts in the series here.
Soil-transmitted helminths and Schistosomiasis
Soil-transmitted helminths (STH) and schistosomiasis (SCH) are the most widespread neglected tropical diseases (NTDs) globally, with 1.5 billion and 240 million individuals estimated to be infected worldwide. In Ethiopia, 36 million and 5 million individuals are currently infected with STH and SCH. STH collectively refers to roundworm (Ascaris lumbricoides; AL), whipworm (Trichuris trichiura; TT), hookworm (Necator americanus, Ancylostoma duodenale and Ancylostoma ceylanicum; HW), and threadworm (Strongyloides stercoralis; SS). The Schistosoma blood flukes cause either urogenital (Schistosoma haematobium; SH) or intestinal (Schistosoma mansoni; SM) SCH. In general, STH and SCH eggs are excreted in infected individuals’ faeces and contaminate soil and water sources. Their presence can therefore be considered a proxy marker for poor sanitation and hygiene.
Ethiopia set ambitious national targets of eliminating STH and SCH as public health problems by 2020 and breaking their transmission by 2025. To support national efforts towards these targets, a recent review presented epidemiological data on STH and SCH prevalence, stratified by region, species, age and diagnostics.
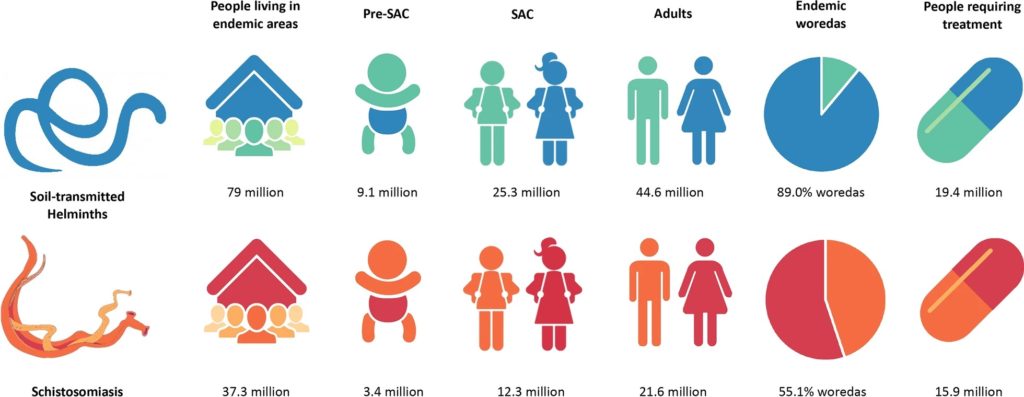
Bringing down the worms: STH & SCH trends in different regions of Ethiopia
The systematic review of published studies between 2000-2020 identified 267 datasets suitable for data extraction. All nine Ethiopian regions reported STH and SCH prevalence, the majority of which were reported in Amhara (38%). Interestingly, sample population focus has shifted over time, moving from community-wide perspectives, to school-aged children (SAC) and pre-SAC.
A total of 402,189 stool samples extracted from the 267 datasets informed the resultant parasite prevalence and intensity measures used for the analysis. Parasite prevalence decreased over time for most species, as shown in the following graph.
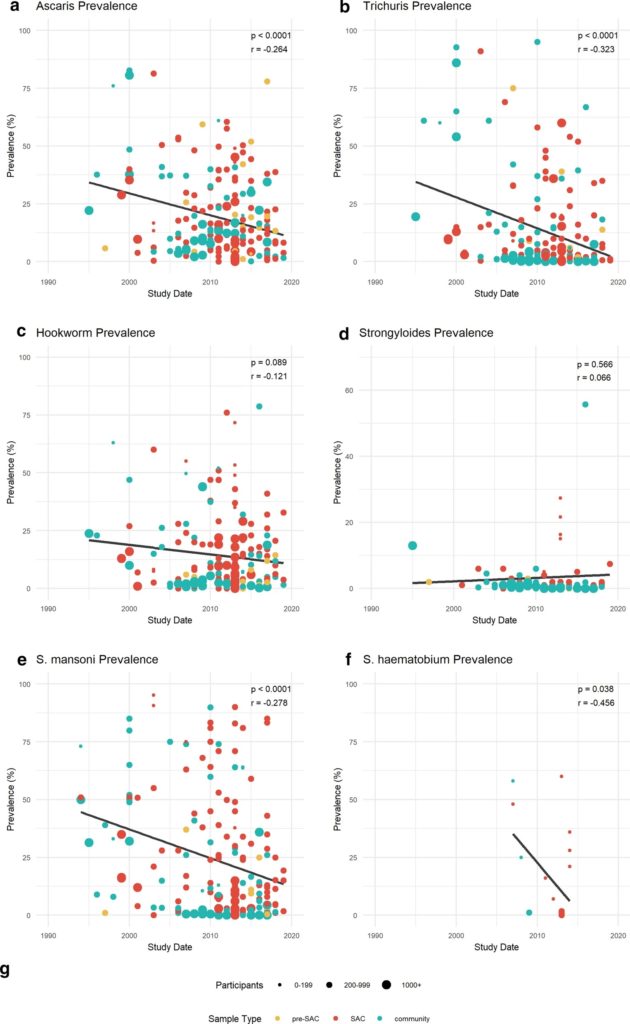
The most statistically significant decrease was demonstrated by TT (34–2%), whilst a significant reduction was also seen in SM (45–14%), AL (34–11%) and SH (35–6%).
The second graph below shows prevalence over time stratified geographically, highlighting regional successes and those requiring further attention. The greatest parasite reduction is seen in Amhara, where TT, SM and AL reduced by 99%, 83%, and 80% respectively, and SNNPR where HW, TT, SM, and AL reduced by 98%, 94%, 86%, and 80% respectively. A significant prevalence increase was only seen in Tigray for HW.
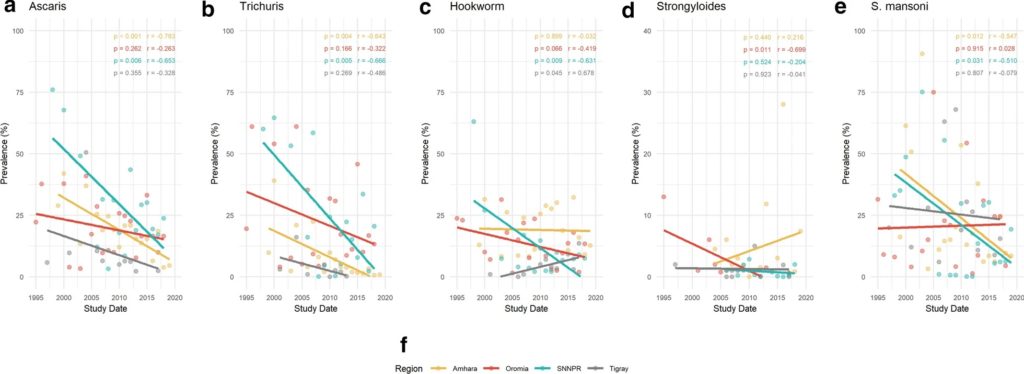
Bringing down the worms: STH & SCH trends in different age groups in Ethiopia.
Most notably, the historical SAC-focused mass drug administration (MDA) is reflected in the age-prevalence distribution of parasite burden. AL and TT showed the most pronounced deviation from the typical distribution of infection, as higher parasite burdens were seen in adults compared to pre-SAC, SAC and adolescents. HW showed higher than expected infection levels in SAC, yet remained typically high in adults. This chiefly demonstrates the interaction of natural age-prevalence distributions on MDA efficacy. AL and TT are normally found in higher burdens in pre-SAC and SAC age groups, which decreases in adulthood. Therefore, SAC-focused MDA has successfully reduced the SAC parasite burden whilst simultaneously creating an infection reservoir in adults.
Bringing down the worms: the diagnostic need to progress to elimination
The overall decrease in prevalence is testament to the intensive efforts the Ethiopian Public Health Institute has made to eliminate STH and SCH. However, as parasite prevalence levels lower, the sensitivity of diagnostics and epidemiological measurements employed will need to increase in order to accurately report national progress. Due to the non-linear relationship between prevalence and average intensity of infection, whereby prevalence changes negligibly at high intensities and dramatically at lower intensities, the use of prevalence as the predominant epidemiological parameter should be re-examined. Despite this, throughout the reviewed literature, intensity was reported in 20-35% studies alongside prevalence. In order to improve Ethiopia’s control program monitoring, the Ethiopian Public Health Institute could consider updating their key statistic definitions to include intensity measures as recommended by the WHO, and foster an environment where intensity is routinely measured alongside prevalence.
Overall, 19 different diagnostic methods were noted throughout this review. Kato–Katz (35%) and formal ether concentration technique (FECT) (5%) were predominantly used either standalone or in combination (6%). Kato–Katz sensitivity is dependent upon STH intensity. Single slides accuracy drops from 74–95% to 53–80% between high and low-intensity settings. This sensitivity can increase by doubling the slides read per sample, from 50-80% in low intensity settings. A third of reviewed studies used single Kato–Katz slides, demonstrating the need to update Ethiopia’s diagnostic protocol to accurately report the low prevalence desired for elimination.
What are the next steps to bring down the worms?
The epidemiological data provided by this review suggests the current SAC-based treatment and control strategy should expand to community-wide intervetions. In doing so, the reservoir of infection in adult populations will be targeted, reducing the re-infection of treated SAC. This will also enable the predominantly adult-centric HW infection to mirror the prevalence decrease seen for AL and TT. As STH and SCH prevalence decreases, current monitoring would benefit from the use of intensity measurements, and improved diagnostic sensitivity to accurately capture success of Ethiopia’s control efforts. Stratifying this further by age and gender will be crucial for evaluation by enabling identification of pockets of infection within communities. This will in-turn generate specific guidelines targeted at age/gender groups to reduce interaction with infectious material through parasite control, WaSH behaviour change activities, and targeted communication materials. Implementing these changes has the potential to help Ethiopia reach their elimination targets in the near future.
 The study featured in this blog post was published in the LCNTDR Collection: Advances in scientific research for NTD control, led by the London Centre for Neglected Tropical Disease Research (LCNTDR). The collection has been publishing in Parasites & Vectors since 2016, and releasing new articles periodically. This series features recent advances in scientific research for NTDs executed by LCNTDR member institutions and their collaborators. It aims to highlight the wide range of work being undertaken by the LCNTDR towards achieving the United Nations Sustainable Development Goals as well as supporting the objectives of the World Health Organization road map for neglected tropical disease 2021-2030.
The study featured in this blog post was published in the LCNTDR Collection: Advances in scientific research for NTD control, led by the London Centre for Neglected Tropical Disease Research (LCNTDR). The collection has been publishing in Parasites & Vectors since 2016, and releasing new articles periodically. This series features recent advances in scientific research for NTDs executed by LCNTDR member institutions and their collaborators. It aims to highlight the wide range of work being undertaken by the LCNTDR towards achieving the United Nations Sustainable Development Goals as well as supporting the objectives of the World Health Organization road map for neglected tropical disease 2021-2030.
The LCNTDR was launched in 2013 with the aim of providing focused operational and research support for NTDs. LCNTDR, a joint initiative of the Natural History Museum, the London School of Hygiene & Tropical Medicine, the Royal Veterinary College, the Partnership for Child Development, the SCI Foundation (formerly known as the Schistosomiasis Control Initiative) and Imperial College London, undertakes interdisciplinary research to build the evidence base around the design, implementation, monitoring and evaluation of NTD programmes.
You can find other blog posts in the series here.

Comments