
Rabies virus
Rabies virus, genus Lyssavirus, is a vaccine-preventable, zoonotic, viral disease present on all continents except Antarctica. Rabies infects all mammals and has the highest case fatality rate of any infectious disease, with over 95% of human deaths occurring in the Asia and Africa regions. In humans, rabies is a neglected tropical disease that predominantly affects poor and vulnerable populations living in remote rural locations.
Rabies infections are typically transmitted through the bite of a rabid animal. The incubation period is typically 2–3 months, but may vary from 1 week to 1 year, dependent upon factors such as location of virus entry and viral load. Initial symptoms of rabies include fever with pain and an unusual tingling, pricking or burning sensation (paraesthesia) at the wound site. As the virus spreads to the central nervous system (CNS), progressive and fatal inflammation of the brain and spinal cord develops. Infections that reach the CNS are almost invariably lethal in both natural reservoirs, such as bats and carnivores, and accidental hosts, such as livestock and humans.
Rabies virus neutralizing antibodies
Interestingly, some exposures to rabies lead to the production of rabies virus neutralizing antibodies (RVNAs). RVNAs clear the infection before the virus invades the CNS and causes neurological symptoms. These “abortive infections” occur predominately in bats but could be widespread in both reservoir and non-reservoir hosts.
Widespread abortive RABV infections open the possibility of using serological studies in non-reservoir species to complement existing surveillance systems. Non-reservoir host surveillance could be more practical than surveillance of reservoirs, involving costly capture and sampling, and more reliable than passive reports of human and animal mortality.
In Latin America, common vampire bats (Desmodus rotundus) are the primary source of rabies. However, livestock and human death reporting efforts vary geographically. In a recent study conducted in southern Peru, Benavides and colleagues aimed to identify animals among five livestock species with abortive infections and determine whether seropositivity correlates with rabies mortality in livestock recorded through passive surveillance.

Abortive rabies infections in Peruvian livestock
Between May and June 2016, livestock sampling was conducted in Apurimac, Ayacucho and Cusco, Peru, which together account for almost 70% of rabies cases in Peruvian livestock. Rabies vaccination of cattle varies considerably while sheep and goats are rarely vaccinated.
Serology was performed on serum samples from 305 animals in 13 districts (92% of samples). All animals were healthy during sampling and questionnaires confirmed the lack of recent illness. None of the animals were vaccinated prior to samples. Of the 305 animals sampled, 23 were seropositive with titers >0.10 UL/mL:
- Overall seroprevalence (n/N = 23/305): 7.5% (95% CI: 5–11)
- Cattle seroprevalence (n/N = 19/173): 11% (95% CI: 7–17)
- Goat seroprevalence (n/N = 3/60): 5% (95% CI: 1–15)
- Sheep seroprevalence (n/N = 1/28): 4% (95% CI: 0–20)
- Equines (n/N = 0/39): 0%
- Pigs (n/N = 0/5): 0%
Titers from positive animals ranged from 0.12 to 70 IU/mL. Five farms had more than one seropositive animal. Approximately one-third (12/35) of the communities sampled had at least one seropositive animal. Follow up activities two years after initial samples confirmed that none of the seropositive animals died from rabies.
Overall, 92% of sampled animals presented evidence of a vampire bat bite. Fresh bites were observed in 56% of all animals, while 77% of animals had evidence of older bites. The frequency of fresh bites was similar in females (55%) and males (58%), as well as in animals older (56%) and younger (58%) than one year. Neither age or sex of the animals was correlated with serological status.
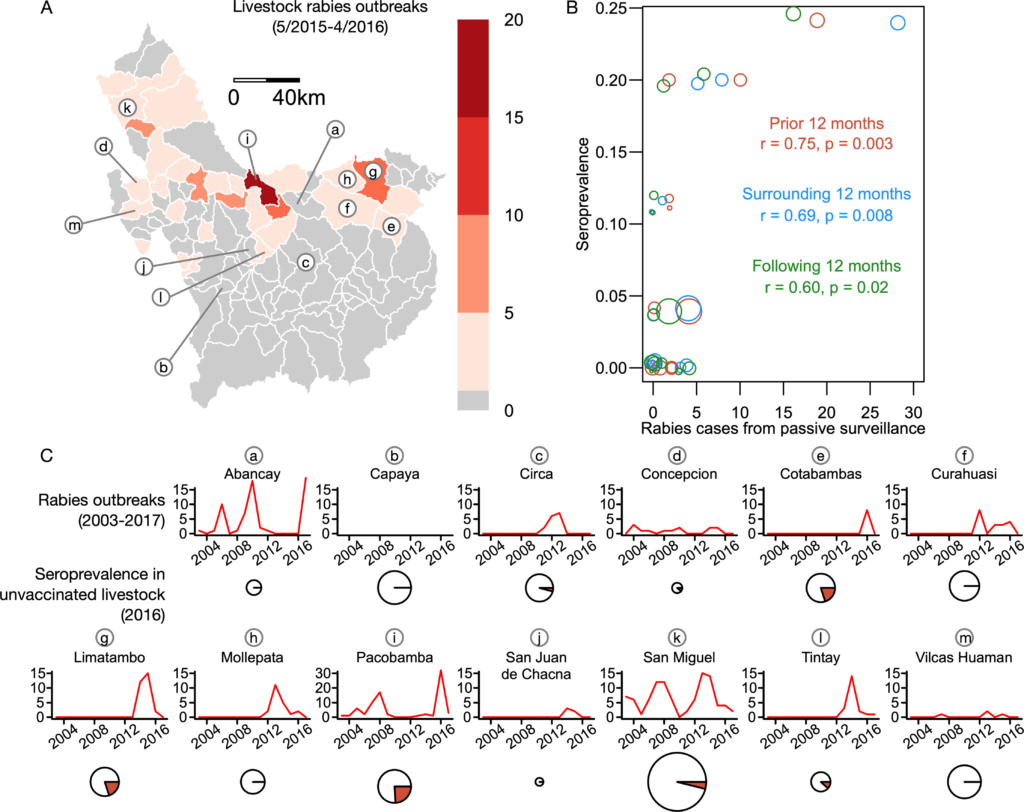
Only one community with seropositive animals was in a district (Circa) without confirmed rabies reported in the 12 months prior to sample collection, although outbreaks had occurred in earlier years. No seropositive animals were found in the Cayapa districts where rabies had never been reported. The researchers also found that the number of cases reported one year prior to sampling significantly increased the likelihood of being seropositive. The number of cases reported 6 months prior or after sampling and the number of cases reported one year following sampling also significantly increased the likelihood of being seropositive.
Conclusion
In the recent study, Benavides and colleagues found that unvaccinated cattle, goats and sheep that are regularly bitten by vampire bats produce detectable levels of RVNAs and remained healthy for at least two years after sampling. The correlation of abortive infections with reported cases of livestock mortality highlights the possibility of using livestock serology to approximate levels of rabies circulation in bats. It also demonstrates for the first time that rabies mortality reports alone do not fully characterize rates of viral exposures from bats to livestock. More research to better understand the basis of abortive infections will help address this gap in knowledge within rabies biology.

Comments