Recent estimates indicate that around 250 million people currently have schistosomiasis, a waterborne disease caused by parasitic flatworms. This corresponds to an average of 3 million disability-adjusted life years – considerably higher than 20 years ago.
Against this background, it is difficult to avoid asking why control efforts for such a widespread disease are so inadequate that the World Health Organization (WHO) has listed it among the ‘neglected tropical diseases’.
How did schistosomiasis become such a scourge?
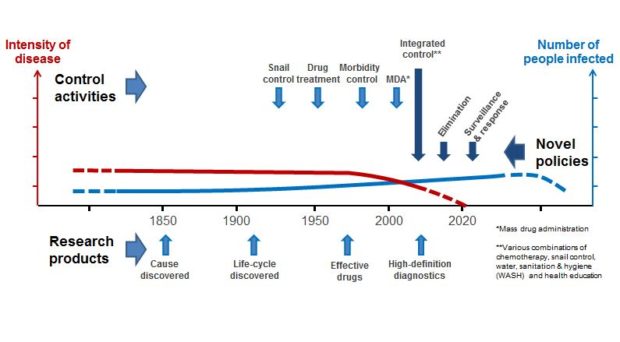
One reason is that effective, counteractive measures against schistosomiasis were not available until the discovery of the parasite by Theodor Bilharz in 1851 and the clarification of its life-cycle by Leiper in 1916. These findings opened up the possibility for organized disease prevention but the recommendation to avoid water contact (and thus the snail intermediate host) was as unrealistic then as it is today.
From the early 1980s, mass drug administration with the then new drug praziquantel started to make a real difference in the endemic areas, and although reinfection remained a problem, morbidity could now be managed through repeated drug treatment. Control programmes that previously relied on anti-snail chemicals released into water bodies used by people in the endemic areas, could now include drug treatment. Indeed, chemotherapy proved so efficient that it soon became the only approach, strongly contributing to the 1984 recommendation by the WHO that morbidity control be the main goal, a strategy that still remains in place. However, there is still a large discrepancy between the number of people requiring preventive treatment and those actually receiving it.
Success in China
Mao Zedong wrote his famous poem ‘Farewell to the God of Plague’ on 1 July 1958 upon learning that schistosomiasis had been wiped out in Yukiang Province only a few years after the establishment of the Chinese National Control Programme. Part of the explanation for the ongoing success of this programme is the fact that snail control was never abandoned. In contrast to other endemic areas, the snail intermediate host species in Southeast Asia (Oncomelania) are amphibious and cannot survive long when covered by mud, a factor utilized to perfection in China.
Important developments
Renewed awareness of the crucial importance of transmission has led to a strengthened emphasis on snail control together with health education and the water, sanitation, hygiene (WASH) approach, now promoted in all WHO member states.
Another important development is the recent advent of new, far more sensitive diagnostics based on the detection of circulating schistosome antigens. These tools are a necessity when dealing with low infection intensities which are now common thanks to preventive chemotherapy. Indeed, preliminary trials with high definition diagnostics indicate that schistosomiasis prevalence may have been considerably underrated.
Vaccination potential?
In the case of vaccine development, there is a continuing lack of funding for research; not that vaccination in itself is a cure-all solution, but even a partially effective vaccine would be a long-term complement to effective chemotherapy.
In recent years, a few candidate molecules for human use have reached the clinical-trial level, but we don’t know how long it will take for their full validation. On the other hand, the usefulness of a veterinary, transmission-blocking vaccine has already been evaluated in China, where the sole parasite species, Schistosoma japonicum, has a range of definitive hosts other than humans. More than 50% protection has been achieved in livestock through vaccination, which should significantly curb the risk for human infection.
Different countries need different approaches
However, the large epidemiological differences between endemic countries makes it impossible to apply the same approach everywhere. Although the scope for elimination of schistosomiasis is promising in some countries, China, Brazil, Egypt, Morocco and Oman among them, the situation is altogether different in sub-Saharan Africa, which harbours 90% of all schistosomiasis in the world. Transmission control here is notoriously difficult and may never be achievable without a human vaccine.
In conclusion, it is highly unsatisfactory to depend upon a single drug for the control of a major disease, even if there is no evidence of widespread resistance. Equally disconcerting is the realization that the number of people with schistosomiasis will continue to rise as a reflection of the ongoing population growth. In spite of spectacular progress towards the goal of disease elimination, there are still research gaps and outstanding issues that need to be resolved. Elimination will be difficult to achieve without a broad approach, including transmission control and the establishment of a regular survey system activating a rapid response whenever needed must be part of the long-term plan.
Comments