On June 4, 2017, a 2-year old little girl died of Rocky Mountain Spotted Fever in Indianapolis. Five days before getting sick, she went on a camping trip with her family where she was likely bitten by a tick. She quickly developed a fever and a rash, and tested positive for strep, and so her physicians initially treated her for that. Unfortunately, her condition continued to deteriorate. After two more visits to physicians, she was diagnosed with Rocky Mountain Spotted Fever. While this disease is easily treatable with doxycycline at the earlier stage of infection, at this point her body was overwhelmed and could not recover. This tragedy, as many others, could have been preventable if the medical professionals recognized the possible connection between her illness and the camping trip she took before taking ill. The taking of simple travel history could have enabled one of her physicians to connect the dots and include Rocky Mountain Spotted Fever on the list of differential diagnosis. According to the CDC, whenever physicians suspect this condition, it is recommended that they start immediate treatment with doxycycline, while waiting for confirmatory laboratory tests. Unfortunately, primary physicians rarely take adequate travel history, and very few of them had any training on the ecology of infectious diseases that would allow them to connect the dots. The curriculum of medical schools primarily focus on the diagnosis and treatment of the most common ailments, focusing on the alleviation of the symptoms in isolation. Therefore, I argue that the medical professionals of the future need to be exposed to the ecology of infectious diseases during their undergraduate education.
At Eastern Washington University, where I teach, every Biology undergraduate needs to take a Senior Capstone class before they graduate. In these classes, while learning about a specific topic, they also need to develop and complete a research project, building on everything they learned during their education at EWU. Each spring, I teach a Senior Capstone class in Disease Ecology. Most of the students who enroll in my class are applying to medical, dental and other health professional schools. Students at the beginning of class had little experience in disease ecology, which was apparent from their reactions when I took them to collect ticks for their first lab period. During the Spring quarter of 2017, they studied the concepts of disease ecology from a textbook edited by Rick Ostfeld and others. In addition, they developed a number of projects that studied the ecology of various diseases relevant to our area. Their projects were either related to ongoing projects in my lab on ticks, mosquitoes and the diseases they transmit in our area, or were developed in collaboration with relevant state and federal agencies. Please see below short summaries of their projects, providing examples of the kinds of exposures they received to disease ecology.
Ivermectin: an Anomaly in the Decline of Anthelmintic Efficacy
(by Samantha Ayotte and Molly Sherwood)
 Over the past decade, scientists, equine veterinarians and horse owners alike have been searching for answers when it comes to the apparent rapid emergence of anthelmintic resistance of parasitic infections within horses. Many equine gastrointestinal parasitic infections are highly virulent, including those members of the family Strongylidae, or more commonly known as strongyles. These parasitic nematodes can cause a multitude of problems including colic, lack of appetite, lethargy, significant weight loss, aneurysm and may even result in death. Ivermectin and fenbendazole are two commonly used anthelmintics known to treat these infections. Our research centered around the question of whether or not resistance was developing to either of these drugs in the strongyles of eastern Washington. Twenty-four horses on a ranch in the area were pre-determined to have strongyle infections, and fecal egg count reduction tests were performed using both ivermectin and fenbendazole. Ivermectin showed to have maintained a 100% efficacy in the treatment of strongyles in eastern Washington, while fenbendazole appeared to comply with the trend of emerging resistance that has been observed around the globe. Our results suggest that while some anthelmintics do indeed appear to be rapidly declining in their ability to treat infections, the future may not be quite as grim for some of the drugs. This begs the question: is ivermectin the super drug of anthelmintics everywhere, or has resistance just not caught up with it quite yet in this part of the world?
Over the past decade, scientists, equine veterinarians and horse owners alike have been searching for answers when it comes to the apparent rapid emergence of anthelmintic resistance of parasitic infections within horses. Many equine gastrointestinal parasitic infections are highly virulent, including those members of the family Strongylidae, or more commonly known as strongyles. These parasitic nematodes can cause a multitude of problems including colic, lack of appetite, lethargy, significant weight loss, aneurysm and may even result in death. Ivermectin and fenbendazole are two commonly used anthelmintics known to treat these infections. Our research centered around the question of whether or not resistance was developing to either of these drugs in the strongyles of eastern Washington. Twenty-four horses on a ranch in the area were pre-determined to have strongyle infections, and fecal egg count reduction tests were performed using both ivermectin and fenbendazole. Ivermectin showed to have maintained a 100% efficacy in the treatment of strongyles in eastern Washington, while fenbendazole appeared to comply with the trend of emerging resistance that has been observed around the globe. Our results suggest that while some anthelmintics do indeed appear to be rapidly declining in their ability to treat infections, the future may not be quite as grim for some of the drugs. This begs the question: is ivermectin the super drug of anthelmintics everywhere, or has resistance just not caught up with it quite yet in this part of the world?
Ticks and the Pathogens they bring to the Community
(by Katarina Behla, Haley Heitzman, Grant Jenkins and Mark Weigand)
 Ticks are a great host for carrying disease and the number of cases reported for tick-borne diseases increase each year for most. We wanted to investigate Rickettsia rickettsii that causes the disease commonly known as Rocky mountain spotted fever (RMSF). In 2010 there were roughly 2300 cases reported for RMSF in humans over the US but we wanted to investigate mammals that were directly in the environment of ticks. In our study, we investigated small mammals such as chipmunks and deer mice at the Turnbull National Wildlife Refuge (TNWR) in Cheney WA for antibodies against Rickettsia. Our procedure was to collect blood samples from these small mammals and use their serum, which would contain the antibodies, in a Spotted Fever Group Rickettsia EIA IgG Antibody Kit. This kit had small wells that contained the antigen of Rickettsia so if there was an antibody for this disease in the serum, the antibody would stick to the antigen and we would have a positive test resulting in a color change when running the kit. If positive, that could mean these animals were introduced to Rickettsia bacteria and this pathogen is prevalent in our area. In our study we set out Sherman Traps and a mix of peanut butter and oats along with cotton bedding to attract the small mammals. After three different trapping days with 50 traps set out, we obtained two different blood samples from small rodents and after running the kit, the test results were inconclusive so we couldn’t say whether they contained the antibody or not. However, this antibody kit worked properly because our positive controls had an obvious color change indicating that the antibodies were present in the positive control serum. With further research and more samples, this kit would be very useful if there is indeed a risk of Rocky Mountain Spotted Fever in Cheney, Washington.
Ticks are a great host for carrying disease and the number of cases reported for tick-borne diseases increase each year for most. We wanted to investigate Rickettsia rickettsii that causes the disease commonly known as Rocky mountain spotted fever (RMSF). In 2010 there were roughly 2300 cases reported for RMSF in humans over the US but we wanted to investigate mammals that were directly in the environment of ticks. In our study, we investigated small mammals such as chipmunks and deer mice at the Turnbull National Wildlife Refuge (TNWR) in Cheney WA for antibodies against Rickettsia. Our procedure was to collect blood samples from these small mammals and use their serum, which would contain the antibodies, in a Spotted Fever Group Rickettsia EIA IgG Antibody Kit. This kit had small wells that contained the antigen of Rickettsia so if there was an antibody for this disease in the serum, the antibody would stick to the antigen and we would have a positive test resulting in a color change when running the kit. If positive, that could mean these animals were introduced to Rickettsia bacteria and this pathogen is prevalent in our area. In our study we set out Sherman Traps and a mix of peanut butter and oats along with cotton bedding to attract the small mammals. After three different trapping days with 50 traps set out, we obtained two different blood samples from small rodents and after running the kit, the test results were inconclusive so we couldn’t say whether they contained the antibody or not. However, this antibody kit worked properly because our positive controls had an obvious color change indicating that the antibodies were present in the positive control serum. With further research and more samples, this kit would be very useful if there is indeed a risk of Rocky Mountain Spotted Fever in Cheney, Washington.
West Nile Virus carrying Mosquitoes: Where are you in Spokane County?
(by Amanda Bryson, Steven Strange, and Emily Marsura)
West Nile (WNV) was found in Spokane County in 2016. WNV is a disease carried by mosquitoes resulting in illness and possible death, leading to a dangerous situation for public health. The two different genus/species that are known to carry WNV in Spokane County are Culex pipiens and Culex tarsalis. In our project, our objective was to determine the distribution of these two mosquito species in Spokane county. We used CDC light traps to catch mosquitoes at 3 different locations, and we identified the mosquitoes to genus. CDC light traps use batteries to run a light and a motorized fan, and also utilize carbon dioxide vapor from dry ice as bait to attract the mosquitoes into the trap. We found Culex sp. in Colbert as well as Central Spokane. Our results provide valuable information on the distribution of vector mosquitoes, which could be used if an outbreak of WNV were to occur. More research would need to be performed, in a collaborative effort with the Spokane Regional Health District, to identify the habitats of the WNV vector mosquitoes of Spokane County.
Importance of protective equipment, concerning local ponds
(by Matthew Cornelius and Tucker Gossett)
Many people are unaware of the dangers of recreating in standing bodies of water. This could be mostly due to local interest being low in safety and high in fun. In our project, we studied the diversity of parasites and bacteria in two ponds commonly used for classes on Turnbull National Wildlife Refuge. We found that bacteria such as E. coli and Legionella, and parasites that cause swimmer’s itch are commonly found in these ponds. Swimmer’s itch (also called cercarial dermatitis) is a skin rash caused by an allergic reaction to infection with flatworm parasites of birds, which are released from infected snails. E. coli can cause intestinal distress, and Legionella affects the respiratory system and could cause shortness of breath, coughing, among other illnesses. If you have swam in or drank the pond water, and have symptoms, seek medical attention immediately. Use protective equipment when in the water such as waders, if you find yourself fishing or waterfowl hunting. While we sought to uncover what was in the local waters, there are still things we didn’t discover. An example of dangers we could have found would be viruses, but due to the limitations we had conducting the study, that discovery will have to wait for further findings.
Diversity of fungal needle endophytes of Pinus ponderosa
(by Jaimie Kenney, Rachael Hamby, Larissa Severance)
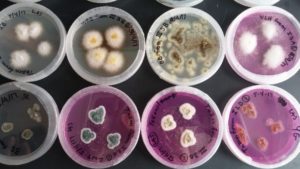 Animals aren’t the only organisms with diverse microbiomes! Plant tissues are also teaming with microbial life. Fungal endophytes are loosely defined as fungi that live at least part of their life cycle within plant tissues without causing obvious negative effects on their hosts. They may inhabit leaf, stem, or root tissue, but unlike mycorrhizae, do not possess hyphae that extend outside of the host plant. Endophytic fungi appear to be in all modern plants, spanning the spectrum from latent pathogens to obligate mutualists. Ponderosa pine (Pinus ponderosa) is the most widespread pine species in North America and is a dominant member of native plant communities across the inland Northwest. However, little is known about the composition of the endophyte community it hosts within its needles or how these endophytes might contribute to its fitness or alter its relationships with other members of the ecosystem. This study aimed to increase our knowledge of fungal needle endophyte diversity in ponderosa pine and elucidate roles these fungal endophytes might play in protecting ponderosa pine from foliar pathogens. Three ponderosa pines of similar age and within close proximity of each other were chosen for sampling from a 200-acre ponderosa pine woodland located near Airway Heights, Washington. From each of the three selected trees, healthy needles were collected from five different branches. On each branch, needles were taken from a younger section and from an older section. Needles were surface sterilized and plated on both rose Bengal and potato dextrose agar plates, then left to grown in the dark for a week. A total of 20 different fungal morphotypes were produced. We then tested whether there was a significant difference between numbers of fungal morphotypes isolated from younger needles versus older needles on the same branch, between needles on different branches on the same tree, and between needles on different trees at the same site. Statistical analysis showed a difference in fungal endophyte communities between different trees, but no statistical difference between branches on the same tree and needles of different ages. A better understanding of the diversity and role fungal needle endophytes of ponderosa pine play in its ecology will help inform future efforts to protect this integral native species.
Animals aren’t the only organisms with diverse microbiomes! Plant tissues are also teaming with microbial life. Fungal endophytes are loosely defined as fungi that live at least part of their life cycle within plant tissues without causing obvious negative effects on their hosts. They may inhabit leaf, stem, or root tissue, but unlike mycorrhizae, do not possess hyphae that extend outside of the host plant. Endophytic fungi appear to be in all modern plants, spanning the spectrum from latent pathogens to obligate mutualists. Ponderosa pine (Pinus ponderosa) is the most widespread pine species in North America and is a dominant member of native plant communities across the inland Northwest. However, little is known about the composition of the endophyte community it hosts within its needles or how these endophytes might contribute to its fitness or alter its relationships with other members of the ecosystem. This study aimed to increase our knowledge of fungal needle endophyte diversity in ponderosa pine and elucidate roles these fungal endophytes might play in protecting ponderosa pine from foliar pathogens. Three ponderosa pines of similar age and within close proximity of each other were chosen for sampling from a 200-acre ponderosa pine woodland located near Airway Heights, Washington. From each of the three selected trees, healthy needles were collected from five different branches. On each branch, needles were taken from a younger section and from an older section. Needles were surface sterilized and plated on both rose Bengal and potato dextrose agar plates, then left to grown in the dark for a week. A total of 20 different fungal morphotypes were produced. We then tested whether there was a significant difference between numbers of fungal morphotypes isolated from younger needles versus older needles on the same branch, between needles on different branches on the same tree, and between needles on different trees at the same site. Statistical analysis showed a difference in fungal endophyte communities between different trees, but no statistical difference between branches on the same tree and needles of different ages. A better understanding of the diversity and role fungal needle endophytes of ponderosa pine play in its ecology will help inform future efforts to protect this integral native species.
Ticks aren’t so dangerous… if you know how to avoid them
(by Vogan Wohlers, Kaitlyn Johnson, Ariel Schneider, Kambria Hyatt, and Tanner Schrumpf)
 Tick populations begin increasing as winter comes to a close and temperatures begin to rise. Hikers should be aware of ticks because they do carry dangerous diseases. There’s no reason to avoid spending time outdoors because of a wariness of tick bites, because simply knowing that ticks are in your presence gives you an advantage. Our study in Cheney, WA showed that ticks prefer warmer temperatures. As the temperature increased throughout the trail on each individual collection day, tick density also increased. However, number of ticks collected reduced week after week. This may have been due to ticks finding hosts and no longer being on the trail for our data collection. These two factors provide evidence that ticks will be most prevalent immediately after winter when the temperature increases, but before they have had an opportunity to find other animal hosts. Tick awareness should thus be heightened during the spring season. Although our observation was hoping to result in a significant favorable vegetation type for ticks, our data did not provide this. There was a relationship between higher numbers of ticks collected in shrubs, but our findings were not statistically significant. While ticks appear to prefer shrubs, they may also be in grass and other areas of vegetation, so those who spend time outdoors should always be prepared for a tick encounter. Focusing on Cheney, WA, tick bites may cause diseases such as tick paralysis, tularemia, and Rocky Mountain Spotted Fever. Any individual who enjoys recreational activities should remind themselves that they don’t want to acquire one of these tick-borne diseases, therefore keeping an eye out for ticks and taking precautions while outside is essential for their health and wellbeing.
Tick populations begin increasing as winter comes to a close and temperatures begin to rise. Hikers should be aware of ticks because they do carry dangerous diseases. There’s no reason to avoid spending time outdoors because of a wariness of tick bites, because simply knowing that ticks are in your presence gives you an advantage. Our study in Cheney, WA showed that ticks prefer warmer temperatures. As the temperature increased throughout the trail on each individual collection day, tick density also increased. However, number of ticks collected reduced week after week. This may have been due to ticks finding hosts and no longer being on the trail for our data collection. These two factors provide evidence that ticks will be most prevalent immediately after winter when the temperature increases, but before they have had an opportunity to find other animal hosts. Tick awareness should thus be heightened during the spring season. Although our observation was hoping to result in a significant favorable vegetation type for ticks, our data did not provide this. There was a relationship between higher numbers of ticks collected in shrubs, but our findings were not statistically significant. While ticks appear to prefer shrubs, they may also be in grass and other areas of vegetation, so those who spend time outdoors should always be prepared for a tick encounter. Focusing on Cheney, WA, tick bites may cause diseases such as tick paralysis, tularemia, and Rocky Mountain Spotted Fever. Any individual who enjoys recreational activities should remind themselves that they don’t want to acquire one of these tick-borne diseases, therefore keeping an eye out for ticks and taking precautions while outside is essential for their health and wellbeing.
Bat Lives Matter
(by Samual Altman, Samanta Castaneda, Victor Hurtado, Liam Johnston, and Jennifer Wilcox)
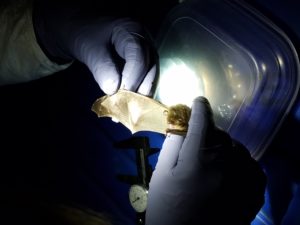 As we speak, a deadly fungal disease is sweeping across the United States killing bats with no end in sight. Starting in New York in 2006 and spreading west White-nose syndrome (WNS) has become an emerging disease of hibernating bats in North America, killing off millions of bats throughout the northeastern and central United States. WNS is caused by Pseudogymnoascus destructans (PD), a fungus that infects the ears, wings and nose of the bats during their winter hibernation period giving it a fuzzy white appearance. Infected bats rouse more often during their hibernation period, which causes them to burn off more of their fat deposits, which in turn causes starvation and then death. PD is spread primarily from bat-to-bat contact or from the environment where the fungus is present. By 2016 WNS made the jump to Washington State with its first confirmed case in King County infecting a Little Brown Bat (Myotis lucifugus). In our project, we had the opportunity to assist Abigail Tobin, the bat biologist at the Washington Department of Fish and Wildlife, as she conducted active surveillance of WNS at a bat roost site on BLM lands in Lincoln County. After an exciting evening, luckily none of the 25 bats processed showed any signs of White Nose Syndrome. Even though WNS doesn’t pose a threat to humans or other animals, fungal spores can be transmitted on shoes, clothing, and recreational equipment. It is imperative that hikers and recreators are aware of the danger PD poses to native bats so they avoid transmitting the disease. The future of Washington bats rests with all of us, and we all need to work to halt the spread of this devastating disease.
As we speak, a deadly fungal disease is sweeping across the United States killing bats with no end in sight. Starting in New York in 2006 and spreading west White-nose syndrome (WNS) has become an emerging disease of hibernating bats in North America, killing off millions of bats throughout the northeastern and central United States. WNS is caused by Pseudogymnoascus destructans (PD), a fungus that infects the ears, wings and nose of the bats during their winter hibernation period giving it a fuzzy white appearance. Infected bats rouse more often during their hibernation period, which causes them to burn off more of their fat deposits, which in turn causes starvation and then death. PD is spread primarily from bat-to-bat contact or from the environment where the fungus is present. By 2016 WNS made the jump to Washington State with its first confirmed case in King County infecting a Little Brown Bat (Myotis lucifugus). In our project, we had the opportunity to assist Abigail Tobin, the bat biologist at the Washington Department of Fish and Wildlife, as she conducted active surveillance of WNS at a bat roost site on BLM lands in Lincoln County. After an exciting evening, luckily none of the 25 bats processed showed any signs of White Nose Syndrome. Even though WNS doesn’t pose a threat to humans or other animals, fungal spores can be transmitted on shoes, clothing, and recreational equipment. It is imperative that hikers and recreators are aware of the danger PD poses to native bats so they avoid transmitting the disease. The future of Washington bats rests with all of us, and we all need to work to halt the spread of this devastating disease.
Knowing when a mosquito species is most likely to be dominant at any particular time of the season will allow us to better prepare for the diseases it may spread
(by Jackie Ferguson, Sarah Kroontje, and Svetlana Pankova)
 Mosquitoes are the most deadly creatures on Earth, in fact, they have killed more people throughout history than all the wars combined! Being able to predict when a species of mosquito will be dominant will allow the CDC to better prepare for the possible spread of diseases. With the increasing threat of mosquito-borne diseases spreading across the world, it is crucial that we remain ahead of these diseases. Some of the diseases that mosquitoes are capable of transmitting in our area (i.e. Cheney, WA) are West Nile virus disease and malaria. By collecting mosquitoes in a CDC light trap and measuring temperature, we were able to make correlations between the abundance of particular species and changing temperature. We observed a positive correlation between temperature and the abundance of mosquitoes present. An increased abundance of mosquitoes means that there is a heightened risk of being infected by these diseases. The application of DEET when going outdoors, hanging mosquito traps, and removing standing water are steps that can be taken to prevent mosquito bites. With threats such as malaria and West Nile virus still prevalent in the world, having more knowledge to better prepare for potential outbreaks is essential to human well-being.
Mosquitoes are the most deadly creatures on Earth, in fact, they have killed more people throughout history than all the wars combined! Being able to predict when a species of mosquito will be dominant will allow the CDC to better prepare for the possible spread of diseases. With the increasing threat of mosquito-borne diseases spreading across the world, it is crucial that we remain ahead of these diseases. Some of the diseases that mosquitoes are capable of transmitting in our area (i.e. Cheney, WA) are West Nile virus disease and malaria. By collecting mosquitoes in a CDC light trap and measuring temperature, we were able to make correlations between the abundance of particular species and changing temperature. We observed a positive correlation between temperature and the abundance of mosquitoes present. An increased abundance of mosquitoes means that there is a heightened risk of being infected by these diseases. The application of DEET when going outdoors, hanging mosquito traps, and removing standing water are steps that can be taken to prevent mosquito bites. With threats such as malaria and West Nile virus still prevalent in the world, having more knowledge to better prepare for potential outbreaks is essential to human well-being.
The above summaries provide a glimpse of the kind of exposures future health professionals can gain to disease ecology as undergraduate students. If they remember what they learned in my class, I’m sure that they will take detailed travel histories of their patients. I also hope that their experience will enable them one day in the future to connect the dots, recognize the connections between their patient’s symptoms and their potential exposure, and avert unnecessary tragedies that come from missed diagnoses.

Comments