
On our third night in the village, we are woken up by the wail of a grieving father. His three-year-old son has just succumbed to malaria during the night and he has come in desperation to seek help. This happened in a village where treatment was freely available and tragically reminds us that the fight against malaria requires societal and educational interventions as much as scientific and technical ones.
The next morning over a traditional fonio breakfast, faces are groggy and still carry the night’s tragedy. Our team, composed of two clinicians, two microscopists and myself in charge of entomology, is readying for our days’ work in Faladje, a small village in central Mali.
Humans are the sole reservoir of the deadliest malaria parasite Plasmodium falciparum, and it is this parasite that our research focuses on. These parasites can only infect new people after spending a couple of weeks inside a mosquito. This fact means that every new case of malaria originates from an infectious mosquito bite. In the Lawniczak Lab at the Sanger Institute where I am a postdoc, we are interested in the interactions between malaria parasites and vector mosquitoes. My project in particular is focused on how parasites behave inside of people to increase their chances of ending up inside of a mosquito, and thus eventually a new person.
Humans are the sole reservoir of the deadliest malaria parasite Plasmodium falciparum.
There are several different “stages” of parasite that live inside the human red blood cells. The stages that cause fever and death are replicating inside of red blood cells, then bursting and infecting new red blood cells. Other stages, known as gametocytes, are waiting to be taken up by a mosquito where they will mate and develop over the next ten days or so. It is the gametocytes that are the focus of the project I’m here to carry out in Mali.
A paradox lies in the fact that some people can transmit parasites to mosquitoes even when none can be seen in their blood. We are researching whether gametocytes are at higher densities in the skin where mosquitoes actually get their bloodmeals from, than in the freely circulating blood. To do this, we compare gametocytes inside mosquitoes that have fed on blood naturally versus artificially. Natural feeding is the kind that is making you itchy right now…a mosquito lands on you, inserts her proboscis, and finds a capillary to puncture and drink from. Artificial feeding is where we take blood from the vein and feed it to mosquitoes through an artificial membrane, visible in the photo below.

This work requires working with very tiny amounts of biological material. Although a mosquito can drink her weight in blood, it’s still a very small volume to work with (a blood meal is around two microliters). I have spent the better part of the last year at the Sanger Institute setting up molecular assays capable of detecting the sexual stage gametocytes and characterising their genetics with so little material.
Conducting this research poses some ethical questions. Although harmless, naïve mosquito bites are uncomfortable and sometimes painful. We have obtained ethical approval from an Internal Review Board and have conducted a comprehensive community consent procedure with local notaries in the village and set up some very strict inclusion criteria and individual consent procedures. The village will benefit from our presence for the time we are there, with free treatment for any disease and all included patients will be included in a comprehensive follow up for 28 days. On my first inclusion I am nevertheless nervous. I have conducted field work before but it is the first time I’m leading it and the first time we are feeding mosquitoes directly on children in this village.
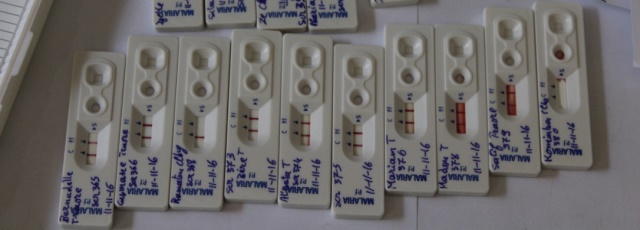
M. is the first patient included in our study, his blood is positive for P. falciparum according to the rapid diagnostic test (see above) and contains gametocyte transmission stages. He is a quiet 11 year-old boy. I first bring him to the insectary with his mother and explain the procedure in simplified French; I then carry out a mosquito feed on myself to demonstrate how simple the procedure is to both of them. After taking a blood sample in the clinic, I bring him back to the insectary for the mosquito feed.
M., now free of malaria, is joking around and curious to understand the function of literally every piece of equipment in the insectary.
We place two pots of mosquitoes on M.’s calves, the five-minute feed seems endless in spite of the microscopist’s and my efforts to distract M. from the itch. M. comes back the next day and I realise I had been wrong, far from quiet, M., now free of malaria, is joking around and curious to understand the function of literally every piece of equipment in the insectary. M. now frequently visits us at the insectary with a few of his friends. On their last visit I was transferring samples to the liquid nitrogen tank and they were observing the fog bubbling out of the container from a distance. Although this will need replication, I think I made an initial discovery: liquid nitrogen has a universal appeal.

Since M.’s first visit, we have treated 800 patients and included more than 20 in the study and the protocol has become a lot smoother. We hope to get some indication as to the hidden biology of the sexual stages of malaria within the next six months.
As malaria biologists, we sometimes get lost in the fascination of studying biological problems, and lose touch with real world issues caused by these deadly parasites. Coming to work every morning for the past weeks to witness dozens of febrile children waiting for treatment has served a powerful reminder of the real burden of malaria and the importance of ridding the world of this affliction.
Publication:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5031309/pdf/12936_2016_Article_1538.pdf
Further links:
Arthur Talman’s page: https://www.sanger.ac.uk/people/directory/talman-arthur-m
Mara Lawniczak’s personal page: https://www.sanger.ac.uk/people/directory/lawniczak-mara-k-n
Vector Parasite Interactions group page: https://www.sanger.ac.uk/science/groups/lawniczak-group
Yourgenome Malaria lifecycle: https://www.yourgenome.org/facts/what-is-malaria
Comments