Why use animal models?
In autism research, animal models provide a valuable tool to fill the gap in knowledge about altered brain mechanisms that lead to the manifestation of behavioral deficits characteristic of autism spectrum disorder (ASD).
Generation of animal models for ASD, relies on findings evolving from genetic and environmental studies, which inform us about the insults responsible for the ASD phenotype. Insults (e.g., genetic mutation) are mimicked in the species of choice to model the deficits we observe in individuals with ASD and to allow a methodical investigation of altered mechanisms at the molecular, cellular, and brain level.

For example, studies in animal models can address questions about the biological effects of a specific genetic mutation on (1) the strength of interaction between nerve cells (known as synaptic plasticity), (2) the integrity of communication between brain regions that work together to regulate specific behavior (known as brain circuits) and (3) on cognitive, motor and social behaviors. Answers to these questions provide the platform for future studies focused on drug discovery and development
Animal models are also being used for testing translatable biomarkers, which are measures that can be assessed comparably in both human and animal subjects. Once identified, these biomarkers can serve as tools to examine the efficacy of potential therapeutics in animal models, predict their effect in human subjects, and inform clinical trials.
Research at the Seaver Autism Center
At the Seaver Autism Center for Research, we are characterizing mouse and rat models with mutations in several ASD risk genes, including in the SHANK3, leading to Phelan McDermid Syndrome (PMS) and in the FMR1 gene, leading to Fragile X syndrome. By taking the approach described above, we discovered that treatment with IGF-1 in a mouse model with a mutation in the Shank3 gene ameliorates synaptic plasticity and motor deficits.
These findings formed the basis of clinical trials with IGF-1 in individuals with PMS, which established the feasibility of IGF-1 treatment in PMS, providing proof of concept to advance knowledge about developing targeted treatments for the synaptic dysfunction associated with ASD.
Another example comes from our recent study on a rat model for ASD, the Shank3-deficient rat, which also harbors a mutation in the Shank3 gene. These rats exhibit social behavior and attentional deficits, recapitulating the neuropsychiatric features of PMS. The nature of the model’s deficits led us to test the effect of the pro-social hormone, oxytocin, on the synaptic plasticity and behavioral deficits.
We found oxytocin significantly improved social memory, attention, and synaptic plasticity deficits, suggesting that oxytocin may have therapeutic potential for both social and non-social deficits in individuals with PMS, supporting our ongoing clinical trials with oxytocin in these individuals. At the Center, we are also using this model to develop electroencephalogram-based (EEG) biomarkers that we can employ in future studies to test the efficacy of novel therapeutics.
Stem Cells
The study of stem cells has also gained a lot of attention in autism research. Stem cells can be generated from blood or skin samples and be differentiated to nerve cells, which are examined in the lab. Stem cells-derived nerve cells overcome the issue of limited access to living neurons, enable the identification of altereted molecular and cellular mechanisms, and allows for testing of drug effciancy at the individual level.
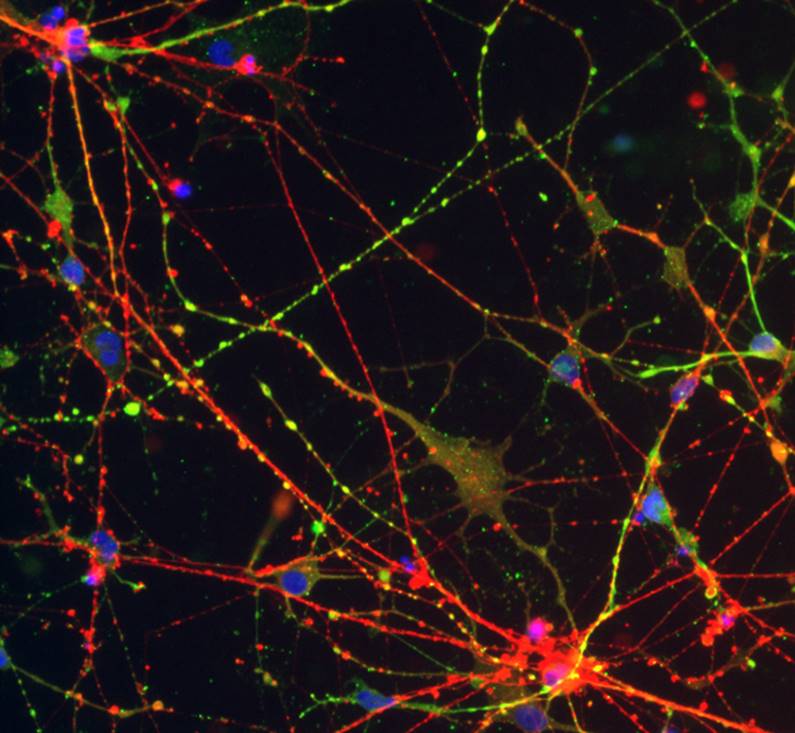
Stem cells are also efficient for carrying out high-throughput screening of small molecules, which can accelerate the discovery of new molecules with potential therapeutic effect. At the Seaver Center, we continue to develop the use of stem cells in autism research, and enroll every affected individual that visits our clinic, his/her parents, and when available, unaffected sibling in this research.
Tune into The Mount Sinai Hospital Facebook on the 5th of June at 11am EST / 3pm GMT to hear myself, Dr. Harony-Nicolas’s, speak in more depth about the topic of animal and cell models used in Autism research at the Seaver Center.
Learn more about the Seaver Autism Center at www.seaverautismcenter.org
Discover more of the current research ongoing in this field at Molecular Autism.
Comments