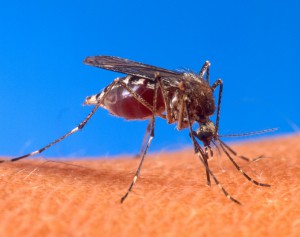
 Dengue, chikungunya, and now Zika virus. All potentially lethal and economically costly reemerging and emerging diseases caused by pathogens transmitted by Aedes aegypti, one of the most widespread and stealthy mosquitoes on the globe. In addition to these, despite the millions of people saved in the last couple of decades, malaria, transmitted by Anopheles mosquitoes, is still a major problem in sub-Saharan Africa, and south-east Asia.
Dengue, chikungunya, and now Zika virus. All potentially lethal and economically costly reemerging and emerging diseases caused by pathogens transmitted by Aedes aegypti, one of the most widespread and stealthy mosquitoes on the globe. In addition to these, despite the millions of people saved in the last couple of decades, malaria, transmitted by Anopheles mosquitoes, is still a major problem in sub-Saharan Africa, and south-east Asia.
Traditional methods, such as insecticidal sprays, are not sufficient to control the mosquitoes, and that control is further threatened by pesticide resistance. The best control method, the elimination of the larval breeding sites of the mosquitoes, is hampered by insufficient resources and the difficulty of keeping a community focused continuously on keeping their environment mosquito free. A dengue vaccine, Dengvaxia, developed by Sanofi Pasteur, has been recently approved and licensed in Mexico, the Philippines and Brazil. However, the efficacy of this vaccine is lower to serotype 2, and requires three injections. A vaccine for chikungunya is in the early trials phase, and a Zika vaccine, while it could be easier to produce based on the West Nile virus vaccine, is still only under discussion. In the face of these difficulties, novel genetic intervention methods have been proposed and developed, going back to the 1940s.
The pioneers were Frederic L. Vanderplank and Alexander S. Serebrovskii, who separately proposed and developed methods in the 1940s, where decreased fitness of heterozygous offspring between two competing strains (underdominance) can be utilized to replace one strain (e.g. a wild type) with another (e.g. one that does not transmit disease). In the 1950s, the USDA has developed methods to irradiate and sterilize massive numbers of male pest insects (the sterile insect technique) to control pests (such as the screwworm fly) by the act of sterile released male insects mating with wild females. This continues to today. These methods were adapted to mosquitoes such as Aedes aegypti and Anopheles in the 1970s, and field trials were initiated. In addition to issues with reduced fitness of irradiated males, the field trials had to be terminated in the face of widespread negative publicity and politicized public distrust. A golden opportunity was lost for a long time at that moment.
Work continued quietly at a slower pace at research labs and at institutions such as the International Atomic Energy Institute in Vienna. In the early 2000s, the Bill & Melinda Gates Foundation initiated their Grand Challenges in Global Health program. One of those challenges was the development of genetic methods to control mosquitoes transmitting diseases. A consortium of research labs across multiple institutions and countries responded to this challenge, in which I was fortunate to play a tiny part in.
The novel methods were all area-wide interventions that relied on the mass release of modified male mosquitoes to disseminate specific genes into the wild mosquito population. Some of these methods were designed to be self-limiting, such that any introduced genes will eventually disappear from the population. Sterile insect releases such as those developed in the 1970s, the RIDL (release of insects carrying a dominant lethal gene) transgenes developed by Luke Alphey at Oxitec Limited, as well as autosomal homing endonuclease gene belong to this category.
Other methods were designed to be self-sustaining, such that introduced genetic elements persist and increase in their frequency in the population, potentially invading it entirely, and spreading spatially. Underdominance, the release of Wolbachia-infected mosquitoes, Medea elements, transposons, and Y-linked homing endonuclease genes belong to this category. These elements, called a gene drive, can then spread other genes that make mosquitoes refractory, or immune to transmit disease.
A highly efficient novel gene drive system has been developed by Ethan Bier and Anthony A. James and was recently published in PNAS. This system uses a Clustered Regularly Interspaced Short Palindromic Repeats (CRISPR), which copies a genetic element from one chromosome to its homolog with >=98% efficiency, to spread anti-malarial genes in a laboratory population of Anopheles stephensi. Despite the promises of such an efficient system, regulatory and ethical questions arose immediately, related to the potential unforeseen and unwarranted consequences of such highly efficient gene drive systems, and the lack of a method to arrest or reverse the effects of a previous introduction.
A similar system, albeit less efficient and therefore less controversial, capitalizes on the unexpected side effect of infection by a specific Wolbachia strain (wMel-Pop) on Aedes mosquitoes. Wolbachia are intracellular bacteria that are ubiquitous in arthropods, with a complex relationship involving many species-specific strains. Wolbachia bacteria can display cytoplasmic incompatibility, where non-infected females can only successfully reproduce with non-infected males, but infected females can reproduce with any male, providing a fitness advantage to infected females, and thereby spreading Wolbachia. In addition, Wolbachia infected female Aedes aegypti were found to have a reduced ability to transmit dengue as well as chikungunya viruses. Field trials with several strains conducted in Australia, Brazil, Vietnam, Colombia and Indonesia have been particularly promising, showing that some strains can invade and persist in the population while others lead to a large reduction of local mosquito populations. However, the use of Wolbachia faces significant challenges due to the potential loss of Wolbachia from the mosquito population due its fitness cost, and the potential evolution of the viruses for increased transmissibility even in Wolbachia-infected mosquitoes.
Perhaps the genetic control method that has been the most thoroughly tested and validated has been the “Oxitec solution”, i.e. the Aedes aegypti mosquitoes engineered with a dominant lethal gene, along with a suppressor gene that acts in the presence of tetracycline. These mosquitoes will happily breed in the lab while fed tetracycline as larvae, but their offspring die in nature in the absence of this antibiotic. When such male mosquitoes are released in the wild, they seek out and mate with wild-type females, whose offspring will inherit the gene and die as larvae, leading to a highly effective population control. The technology has been tested and evaluated in small scale releases and laboratory trials in the Cayman Islands, Malaysia, and Brazil. Areas where the Oxitec mosquitoes have been released have reported an up to 90% reduction in the number of Aedes aegypti, and very large decrease in the number of dengue cases. Oxitec scientists, such as Derric Nimmo, have diligently run numerous ecological and safety trials, including the effect of realistic amounts of tetracycline on the survival of Oxitec females, based on the potential environmental contaminations with tetracycline from human and animal sources. The results are all encouraging, and the Brazilian government has recently invited Oxitec to scale up their trials to a larger population. Public perception and reception in the areas where releases occurred are overwhelmingly positive, even calling the Oxitec mosquitoes the “Friendly mosquito”. By all indication, these “Friendly mosquitoes” are ready to control the mosquitoes transmitting dengue, chikungunya and Zika virus at a large scale!
As I’m writing this, the WHO Director-General has declared the Zika virus outbreak in Brazil and South America a public health emergency of international concern. Every day brings new insight into the spread and capabilities of Zika virus, such as the news of sexual transmission of the virus from a returning traveler within the United States. My hope is that Zika virus will provide the public and the affected governments the final push to embrace genetic control methods as part of an Integrated Pest Management programme, and provide the resources and support to scale up production to control these mosquitoes at a regional or even country-wide basis. Then both would-be and current parents can stop worrying about mosquitoes and the pathogens they transmit.
Disclaimer: The author has worked at Oxitec Limited during a single year in 2007, but does not own shares of the company nor is in any financial or professional collaboration with the company currently.

Comments