
Non-communicable diseases (NCDs), like cardiovascular diseases and diabetes, represent the primary cause of mortality worldwide. An increasing volume of NCDs in low- and middle-income countries (LMICs) now accounts for the majority of recent surges in the global NCD burden.
Simultaneously, increasing humanitarian crises in LMICs have resulted in the global forced displacement of people reaching record highs, with the average length of displacement now greater than 20 years. Until recently, the problem of NCDs in conflict-affected populations was largely neglected. However, with growing awareness of the challenges NCDs represent in humanitarian settings, clinical guidance has been developed for chronic NCD care in LMICs.
Since 2014, the non-governmental organization (NGO) Médecins Sans Frontières (MSF) has supported the Jordanian health system by providing multidisciplinary, primary level NCD care to Syrian refugees and vulnerable Jordanians living in Irbid, Jordan. This week in BMC Health Services Research, Ansbro et al. describe their experiences with MSF, adapting the RE-AIM framework to evaluate MSF’s program of NCD care.
RE-AIM is a framework consisting of five elements, Reach, Effectiveness, Adoption, Implementation, and Maintenance. The framework was originally developed to encourage program planners, evaluators, funders, and policy-makers to be more attentive to essential program elements, to improve sustainable adoption, and promote the implementation of effective, generalizable, evidence-based interventions. In this study, through the use of mixed methods, Ansbro et al. examined the RE-AIM five key elements of the MSF Syrian refugee NCD program.
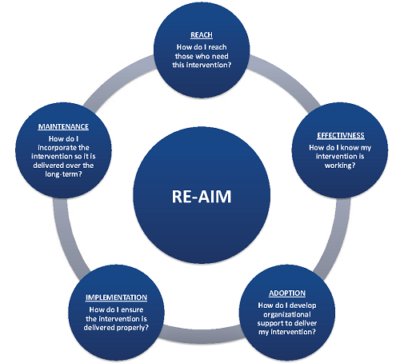
Reach, Effectiveness, and Adoption
Most areas of the program were viewed as acceptable to patients, staff, and stakeholders. Although the care was free, patients were burdened with indirect costs, like paying for transport, to attend clinics, potentially outweighing the benefits of ‘free’ care.
The program achieved good clinical outcomes for treating patients with hypertension and diabetes. However, more research in the future that uses longer follow-up periods is needed to understand the prevalence or outcomes of major complications of NCDs.
Implementation
A key challenge for implementation was the impact of Syrian patients’ experiences of war, loss, and social suffering on their engagement with NCD care. Staff also shared concerns that they could not manage medical problems in isolation from the psychosocial issues patients faced and they felt ill-equipped to handle patients’ war-related trauma.
Patients and staff also reported that the referral pathways for specialist services were troublesome and confusing. Funding for specialist referral pathways was limited, even though MSF managed to secure additional funding. This highlights the need for future programs to securely implement specialist referral pathways, ensuring they are designed to be affordable and accessible from the start.
Maintenance
A key challenge for maintaining the program was cost. High costs were partly responsible for the program’s limited coverage and scope. However, there is room for adaptations. For example, MSF introduced nurse task sharing, which could lead to cost savings.
Another challenge here is the availability of highly qualified family medicine specialists, for the management of patients with complex needs. While MSF had access to a large number of highly qualified Jordanian staff on this occasion, this is often not the case in all humanitarian crisis settings. This issue is difficult to address, but the authors propose potential workarounds, like telemedicine, as a possible solution for future programs.

Research in humanitarian crisis settings is extremely difficult. Not only do governments and humanitarian organizations face significant challenges in effectively tackling NCDs in LMICs, but the evaluation of interventions in humanitarian settings is equally as challenging. Still, this study demonstrated that RE-AIM is a valuable tool to guide complex interventions in humanitarian crisis settings. Ansbro et al. bridge a knowledge gap in the delivery of care in humanitarian settings, however, more research is urgently needed to strengthen responses to NCDs in humanitarian crisis settings. Future programs need to focus on simplifying care models, reducing costs, and harnessing telehealth resources.
Comments