Chemotherapy during late stages of pregnancy may affect future fertility of the unborn child
Chemotherapy during the later stages of pregnancy is generally thought to have no significant detrimental effect on fetal development. As a woman’s reproductive lifespan is determined before birth, it is important to understand the effects of chemotherapy on the ovaries of the developing female fetus.

Female egg cells develop from germ cells, which are enclosed within ovarian follicles. Follicle development begins 17 weeks into the pregnancy and is not complete until birth. Researchers used a novel in vitro method of mouse cell culture to investigate the effects of etoposide, an anti-cancer drug, on ovarian development.
It was found that prior to follicle formation, presence of etoposide reduced both follicle production and follicle health. After the complete development of the follicle, etoposide had little effect on follicle health and numbers. Albeit preliminary, these findings suggest that exposure to etoposide could have long term effects on the future fertility of the female fetus, potentially reducing the fertility window and likelihood of conception.
Stimulating melanoma phagocytosis with the innate immune system amplified by TLR agonists
Anchoring molecules which bind phagocytic receptors to the cell surface of tumors enables the immune system to recognize, and attack, tumor cells. This effect can be further optimized by applying LPS, a TLR-4 agonist which is toxic to humans, to the tumor cell surface. Caisovà and colleagues present a study conducted to optimize this therapy for human treatment.
A mouse-model which had been transplanted with B16-F10 melanoma cells was used to test several combinations of TLR agonists and phagocytosis-stimulating ligands, to find the most effective treatment with low toxicity to humans.
Of all the combinations studied, it was found that R-848 and covalently anchored mannan-SMCC had the best therapeutic effect, reducing tumor size in vivo. The addition of heat-killed Listeria monocytogenes further increased mouse survival rate to 83.3%. Furthermore, binding of poly(I:C) to tumor cells protected against re-transplantation with no pathological symptoms observed for over a year after treatment.
HOX genes a potential therapeutic target in treating mesothelioma
Mesothelioma is a malignancy of the lung mesothelium cells usually associated with asbestos exposure. Upon diagnosis, treatment options are limited and the prognosis is generally poor. Morgan et al. identify HOX genes as potential therapeutic target in primary mesothelioma tumors.
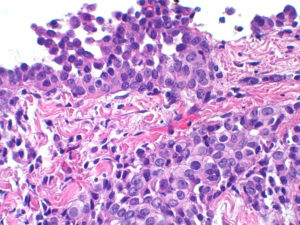
In some malignant cells, HOX genes become dysregulated, increasing cell proliferation. It was shown that treating mesothelioma-derived cell lines with HXR9, a peptide antagonist of HOX protein, leads to tumor cell death (apoptosis) whilst leaving healthy cells intact. Next, HXR9 treatment was tested in mice with mesothelioma. A significant inhibition of the tumor growth was observed, implying that HOX genes may be an important therapeutic target in mesothelioma therapy.
Improving quality of life after prostate cancer diagnosis with community-based sport
The FC Prostate Community Trial (FCPC) – a randomized, controlled, parallel-group trial currently being conducted in Denmark – aims to determine the effects of recreational football on rehabilitation in men who have been diagnosed with prostate cancer.
Previously, exercise has been shown to improve disease-specific quality of life and reduce treatment-related toxicity in prostate cancer patients. This study investigates the effect of 1 hour of recreational football training sessions twice weekly on cancer-specific quality of life, lean body mass, fat mass, bone mineral density and content, and well-being. The trial is currently ongoing and is expected to be completed in November 2017.
Senior author, Julie Midtgaard, talks more about the Study protocol here.

Monitoring and tailoring cancer therapy with biomarkers

Different drugs elicit a different response depending on the patient; understanding the reasons for this may not only improve treatment, but the development of future anti-cancer drugs. Tailoring treatment to the individual ensures the optimum patient response, reducing disease progression and drug toxicity. Currently, using biomarkers to tailor cancer therapy focuses on the prognosis and prediction of disease.
A review by Shahil Amin and Oliver Bathe discusses the potential of using biomarkers in an alternative way, to assess a patients’ response to treatment. The authors explore the implications of treatment response biomarkers which, they argue, may not only benefit individual patients, by minimizing exposure to drugs which may be ineffective or toxic, but could also revolutionize how drugs are developed and clinical trials are conducted.
Significant dose-response relationship between alcohol consumption and prostate cancer risk
A meta-analysis and systematic review by Zhao et al. identifies a significant dose-response relationship between alcohol intake and risk of developing prostate cancer. The study aimed to reduce misclassification error, which occurs when participants who are defined as non-drinkers may have consumed alcohol regularly in the past. The study showed that when misclassification error is eliminated, there is a significant increase in prostate cancer risk in low-moderate drinkers when compared to those who abstain from alcohol.

In studies with no misclassification error, an alcohol consumption of 1.3-24mg per day may increase prostate cancer risk by as much as 24%. This presents an increase in 16% when compared to studies which include former drinkers in the abstinence group. As well as providing important data regarding the long term effects low alcohol consumption has on health, this study highlights the effect misclassification errors can have on data.
Comments