
Visual signs and symptoms in patients with the visual variant of Alzheimer’s disease
 Visual variant Alzheimer’s disease (VVAD) is becoming a more frequent cause of age-related reading difficulties in the absence of any ophthalmologist-identified abnormalities in refraction, the cornea or general eye health. Unlike standard Alzheimer’s disease, VVAD initially presents with an array of visual rather than cognitive or memory-related symptoms making the ophthalmologist the first port of call for accurate diagnosis of the condition. As a result, understanding the typical symptoms VVAD patients present with at standard eye test appointments could improve early diagnosis rates for the disease.
Visual variant Alzheimer’s disease (VVAD) is becoming a more frequent cause of age-related reading difficulties in the absence of any ophthalmologist-identified abnormalities in refraction, the cornea or general eye health. Unlike standard Alzheimer’s disease, VVAD initially presents with an array of visual rather than cognitive or memory-related symptoms making the ophthalmologist the first port of call for accurate diagnosis of the condition. As a result, understanding the typical symptoms VVAD patients present with at standard eye test appointments could improve early diagnosis rates for the disease.
Recently, a retrospective study by Kaeser and colleagues aimed to identify the common symptoms of VVAD from the files of ten patients diagnosed with the condition. In all of the patients, VVAD diagnosis was previously confirmed by detailed neuro-ophthalmologic examination, neurological testing, neuro-physical testing and a cerebral magnetic resonance imaging (MRI). Overall, the analysis demonstrated that the most common symptom present in these patients at initial identification of VVAD was compromised near vision causing reading difficulties, writing difficulties and a visual blur sensation. Furthermore, detailed testing confirmed a high frequency of dyslexia, color vision but not color identification impairment, compromised visual perception (simultanagnosia) and visual field defects (incomplete homonymous hemianopia) in these VVAD-diagnosed individuals. MRI scans confirmed the presence of parieto-occipital cortical atrophy in all ten individuals.
Taken together, these detailed analyses clearly indicate the importance of the ophthalmologist and attendance at standard eye care appointments in successful early diagnosis of VVAD. Particularly in cases where patients present with reading difficulties that cannot be explained by general eye health.
Helicobacter pylori infection, dementia and primary open-angle glaucoma: are they connected?
 The link between neurodegenerative dementia, glaucoma and infection with the Gram-negative pathogenic bacterium, Helicobacter pylori, has been the subject of numerous contradictory investigations. In order to try and get to the bottom of this problem, Tsolaki and colleagues conducted a prospective diagnostic study that specifically focused on finding a link between Alzheimer’s disease, frontotemporal-dementia, Parkinson’s disease, Lewy body dementia, primary open angle glaucoma and Helicobacter pylori infection.
The link between neurodegenerative dementia, glaucoma and infection with the Gram-negative pathogenic bacterium, Helicobacter pylori, has been the subject of numerous contradictory investigations. In order to try and get to the bottom of this problem, Tsolaki and colleagues conducted a prospective diagnostic study that specifically focused on finding a link between Alzheimer’s disease, frontotemporal-dementia, Parkinson’s disease, Lewy body dementia, primary open angle glaucoma and Helicobacter pylori infection.
Results from this study clearly demonstrate that the prevalence of H. pylori infection is greater in individuals suffering from dementia or primary open angle glaucoma compared to the general population. Furthermore, primary open angle glaucoma was found to occur more frequently in individuals suffering from Alzheimer’s or Parkinson’s disease. Frontotemporal-dementia and Alzheimer’s dementia were more common in patients diagnosed with primary open angle glaucoma than in healthy individuals.
In conclusion, this study demonstrates that the investigated neurodegenerative conditions are clearly linked to each other and to H. pylori infection. Further research into the molecular and biochemical links between these conditions could improve both diagnosis and routine patient care in the future.
Efficacy of selective laser trabeculoplasty for normal tension glaucoma: 1 year results
 Normal tension glaucoma (NTG) is a unique condition whereby progressive optic nerve damage occurs despite the pressure in the eye remaining in the normal range. In some countries, including Japan and Korea, NTG is the most prevalent form of primary open angle glaucoma. Primary open angle glaucoma can be treated with medication or with selective laser trabeculoplasty (SLT). Despite its safety and efficacy, the use of SLT in the treatment of NTG is under-represented in the literature. Research conducted by Lee and colleagues aimed to explore the sustainable nature of SLT efficacy one year after its application in NTG patients. The results of this longitudinal study indicated that one isolated session of SLT was able to achieve a 15% reduction in intraocular pressure and a 27% reduction in the use of medicated eye drops to control the condition. These findings suggest the future potential of the procedure as an efficient means on controlling NTG disease progression.
Normal tension glaucoma (NTG) is a unique condition whereby progressive optic nerve damage occurs despite the pressure in the eye remaining in the normal range. In some countries, including Japan and Korea, NTG is the most prevalent form of primary open angle glaucoma. Primary open angle glaucoma can be treated with medication or with selective laser trabeculoplasty (SLT). Despite its safety and efficacy, the use of SLT in the treatment of NTG is under-represented in the literature. Research conducted by Lee and colleagues aimed to explore the sustainable nature of SLT efficacy one year after its application in NTG patients. The results of this longitudinal study indicated that one isolated session of SLT was able to achieve a 15% reduction in intraocular pressure and a 27% reduction in the use of medicated eye drops to control the condition. These findings suggest the future potential of the procedure as an efficient means on controlling NTG disease progression.
Visual outcomes after bilateral trifocal diffractive intraocular lens implantation
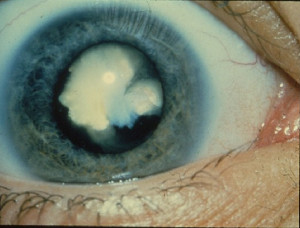 Cataracts are becoming an increasingly common health problem within the aging population, resulting in lens clouding and reduced vision in one or both eyes. New models of intraocular lenses are frequently introduced to cataract surgery with the aim of providing the best possible near, intermediate and far vision. A prospective, non-randomized, observational study conducted by Carballo-Alvarez and colleagues aimed to assess the visual effects of a new trifocal diffractive intraocular lens implantation after bilateral cataract surgery.
Cataracts are becoming an increasingly common health problem within the aging population, resulting in lens clouding and reduced vision in one or both eyes. New models of intraocular lenses are frequently introduced to cataract surgery with the aim of providing the best possible near, intermediate and far vision. A prospective, non-randomized, observational study conducted by Carballo-Alvarez and colleagues aimed to assess the visual effects of a new trifocal diffractive intraocular lens implantation after bilateral cataract surgery.
Overall, the new lens is comprised of two diffractive structures that add powers of + 3.50 D for near vision and + 1.75 D for intermediate vision. The results of the study indicate that implantation of this lens is associated with significant improvements in intermediate vision without exertion of compromising effects on near or far vision. Furthermore, contrast sensitivity was found to be adequate with no reports of any adverse photic events after implantation. Taken together these findings indicate the future potential of the new lens as a suitable option for improved vision and rapid patient recovery after cataract surgery.
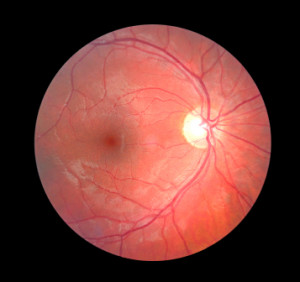
Polypoidal choroidal vasculopathy, or PCV, is a debilitating pathology of the eye whereby lesions develop underneath the retinal pigment epithelium. The condition typically leads to the formation of polyps, or abnormal mucous membrane-associated protruding tissue growths, on the eye. Currently the recommended treatment for PCV consists of a combination of antivascular endothelial growth factor injections and standard dose verteporfin photodynamic therapy (PDT). However, full dose PDT is associated with adverse side effects such as reduced vision and poor blood supply to the choroid (choroidal ischaemia), making half-dose PDT therapy a more attractive future treatment option.
Wong and colleagues conducted a prospective, non-comparative interventional study to investigate the efficacy of half-dose PDT in the treatment of PCV when combined with an intravitreal drug, ranibizumab. Patients were followed up for 12 months and assessed for polyp regression rate, vision changes, thickness of the central foveal and need to repeat the half dose PDT therapy intervention. The results of the study indicated that half dose PDT- ranibizumab combination therapy was remarkably effective in the treatment of PCV characterized by the formation of single small polyps. However, treatment effectiveness was reduced in PCV cases characterized by multiple polyps or development of a branched vascular network. Future studies are required to determine the efficacy of half dose PDT- ranibizumab therapy over time, its safety in comparison to full dose therapy and the lesion types it can be successfully applied to.
Nice Blog….Keep writing