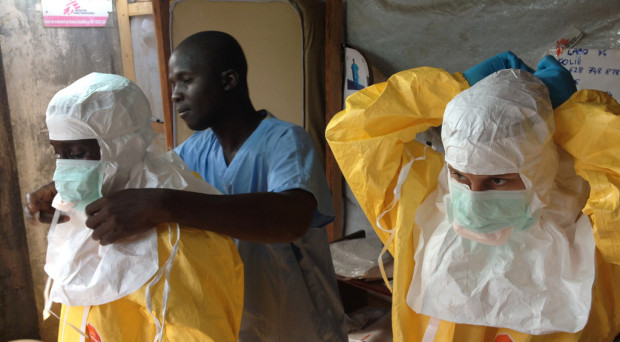
The recent Ebola outbreaks in some parts of West Africa (Guinea, Liberia and Sierra Leone) riveted the world and put a spotlight on the need for concerted effort and significant investment in research and capacity building efforts.
It pushed researchers, scientists, policy makers and nations, across the world in general and the three countries in particular, to think hard on how to effectively control the spread of a disease for which no specific pharmaceutical intervention (such as vaccine or drug treatment) exists. Thus, factors that inhibit its control needed to be rapidly identified, and managed, to ensure a successful control outcome.
As of the April 2, 2015 update by the Centers for Disease Control and Prevention, the disease has accounted for 25,228 cases (suspected, probable and confirmed), and 10,462 fatalities. The following media headlines were unmistakable during the high moments of the 2014 Ebola outbreaks:
As Ebola virus spreads in West Africa, some blame health workers
“Ebola’s Deadly Spread in Africa Driven by Public Health Failures, Cultural Beliefs”
“As Ebola virus spreads in West Africa, some blame health workers”
“Kissing corpses is helping spread Ebola, expert says”
“Ebola patients flee as Liberia clinic looted”
“There is no such thing as Ebola”
“Eight killed in Guinea town over Ebola fears”
Can cultural practices affect Ebola spread?
A recent study published in BMC Medicine investigates the role of cultural belief systems, customs, and health care settings on the transmission dynamics of the 2014 Ebola outbreaks, using data from Guinea.
African culture generally prides itself on strong family ties, hospitality, and intra- and extra- community relations, where, for instance, each individual household cares for its immediate and extended family members.
African culture generally prides itself on strong family ties, hospitality, and intra- and extra- community relations, where, for instance, each individual household cares for its immediate and extended family members. Hugs and handshakes are common ways of greeting or expressing support and love for loved ones and acquaintances.
Another major aspect of the African culture is the rituals associated with burying the dead. This “proper burial” typically involves having extended family members and acquaintances of the deceased (which, in general, means pretty much all members of the local community) in very close proximity and contact with the corpse of the deceased, as people pay their last respects which they believe must be done in specific ways.
All the aforementioned constitute a cultural and traditional belief system and custom that are held in most African societies (particularly in the rural areas, where the 2014 Ebola outbreaks were concentrated).
This beautiful culture is embedded in a system in which the health-care system is, itself, generally weakened due to factors such as poverty, famine, corruption, and, in some places, years of wars. Such factors (particularly corruption and wars) have led, in some cases, to mistrust of governments and people in authority.
The aforementioned belief systems – particularly Africa’s culture of touching as a means of expressing natural support to sick loved ones – and the weakened healthcare system (and the absence of pharmaceutical intervention) provided the perfect breeding ground for the 2014 Ebola outbreak to blossom. No matter the culture, it is hard to see a loved one sick and yet be unable to help. Imagine, having a sick mother or child dying of the Ebola virus disease, and yet you have to stay away.
However, there are not enough well-trained public health response teams or clinicians to come and help the dying mother or child. As evident during the early stages of the 2014 Ebola outbreaks, the already-overwhelmed healthcare system could not accommodate an additional sick person. Owing to the lack of health-care facilities, Ebola-infected patients stay away from much-needed professional help and care, thereby posing a risk to their immediate families and the local community at large.
Our paper highlights the fact that detrimental cultural belief systems and customs do amplify the transmission of the Ebola disease in the three affected countries. Furthermore, using data from Guinea, we showed that the main contributors to the number of Ebola cases were Ebola-infected deceased individuals and symptomatic infected patients. We found that individuals in the later stages of infection are the greatest contributors to Ebola spread.
This suggests mitigation measures, such as the early intervention and proper identification (contact tracing) of individuals who have been in contact with Ebola-infected humans, could be effective in controlling the spread of Ebola.
How can we reduce Ebola transmission?
The study shows that significant reduction of new Ebola cases can be achieved by increasing health-care workers’ daily shift hours, limiting hospital visitation and educating the populace to abandon detrimental traditional/cultural belief systems. However, given the known effects long work hours can have on the efficiency of health-care workers, a fine balance between reducing the contacts between Ebola-infected patients and the health-care workers, and having more health-care workers to minimize the need for long-hour shifts, need to be reached.
Despite the enormous public health and socio-economic impact of the disease (and the aforementioned absence of pharmaceutical intervention), it is reassuring to know, via mathematical modeling, that the disease is, in fact, controllable using basic non-pharmaceutical measures alone.
Control of the infection, however, requires contributions from many facets of the society, including mounting (and sustaining) an effective public health education campaign at the grassroots level. The impact of community grassroots movements, with empowerment of community leaders and chiefs, given the appropriate training, cannot be over-emphasized. They, perhaps unlike their governments, can help minimize the public mistrust and anger against people in authority.
the global public health community, and the three main affected countries, cannot afford to be complacent
As the global public health agencies – spearheaded by the World Health Organization – and the affected nations continue to mount a concerted effort to combat (or end) the 2014 outbreaks, the victims of such a devastating disease (such as the orphans and the survivors) should not be forgotten. The public health education campaign must continue in order to prevent a major resurgence. To this end, the global public health community, and the three main affected countries, cannot afford to be complacent.
One Comment