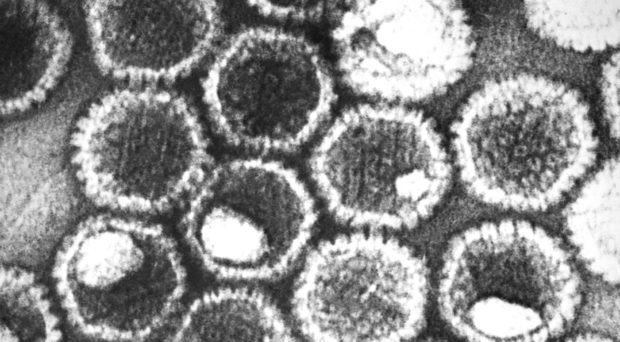
Your paper ‘Nanoparticle exposure reactivates latent herpesvirus and restores a signature of acute infection’ has been voted as the winner of the 2018 Particle and Fibre Toxicology best paper award – congratulations! Can you briefly explain what your study is about?
Both inhalation of environmental nanoparticles and persistent herpesvirus-infection have been implicated to contribute to the development of chronic lung disease. Based on this, we hypothesized that the combination of nanoparticle exposure and virus infection leads to a different outcome than exposure to each factor alone. To evade the immune system, some viruses hide in specific cells of their host and persist there – this is referred to as a latent infection. Exposure to nanoparticles in addition to a latent virus infection may result in the disruption of the immune system and reactive the dormant virus.
Can you explain the set-up and conclusions of your study?
To test this hypothesis, we conducted cell based studies in latently infected human and mice cells and animal studies using a mouse model of latent herpes infection. In cell cultures, nanoparticle exposure of latently infected cells induced virus replication and the expression of viral proteins. In the lungs of latently infected mice, an increase in viral proteins was detected after nanoparticle exposure and metabolic and gene expression analyses also revealed patterns resembling acute infection. Our results therefore indicated that under conditions of persistent herpesvirus infection, the second hit by nanoparticle exposure restores a molecular signature characteristic for acute virus infection. Nanoparticle exposure boosts the production of viral proteins and induces an inflammatory response in the lung – a pattern which might finally result in severe tissue damage and long-term harm.
Nanoparticle exposure boosts the production of viral proteins and induces an inflammatory response in the lung
Why is it important to explore the effects of nanoparticle exposure, particularly with latent infections?
Usually, healthy, noninfected animals are investigated for studying health effects related to nanoparticle exposure, however, persistent herpesvirus-infection is omnipresent in human society (e.g. 80% adults carry human herpesvirus). Additionally, a number of studies imply that not only particle exposure but especially herpesviruses might contribute to the development of chronic lung diseases such as idiopathic pulmonary fibrosis. A coincidence of these two factors might generate escalations not observed in single hit models.
How transferrable are the results of your study with humans?
In our publication, we show that nanoparticle exposure can trigger herpesvirus reactivation from latency, not only in mice but also in human cells, indicating that this process might not be restricted to rodents but also apply to humans. Meanwhile, we have initial epidemiological data supporting our hypothesis that high (nano)particle burden can cause latent herpesvirus reactivation.
The initial epidemiological data supports the from ‘model particles’ deduced hypothesis, because in a well characterized cohort, increased anti-human herpesvirus antibody concentrations were found to be associated with exposure to high ambient particle number concentrations.
What research are you currently working on and what do you expect to investigate in the future with long-term studies?
Besides the epidemiological translation, we are working on the identification of the mechanism by which nanoparticle inhalation leads to the reactivation of latent virus, and hope to identify therapeutic means of intervention.
Comments