EuroSciCon held their 10th annual ‘Histopathology: advances in research and techniques’ meeting at the Royal College of Pathologists in London on April 12th. The meeting was attended by histopathologists from across Europe, as well as by BMC Clinical Pathology. Topics ranged widely, from the introduction of the newest technologies to the best ways to utilise older techniques (the full agenda is available here). A particular focus was using methodological advances to drive discovery of new biomarkers for cancer and other diseases.
 A recurring theme was the utilisation of new technologies in histopathology. Eveline Sjöstedt demonstrated how advances in histopathology can be applied to large scale research projects, presenting an update of progress with the Human Protein Atlas. The largest research project in Sweden, it aims to systematically explore the human proteome through high-throughput generation of affinity-purified antibodies. As well as exploring protein expression levels in normal human cells, the project aims to reveal the changes in protein levels in tumour cells, hopefully identifying new cancer biomarkers. For a project of this scale to work, samples need to be processed en masse in a quick and efficient fashion. As Dr Sjöstedt explained, creating such a high-tech process often means conducting rather low-tech experiments. For example, is it ok to leave slides sitting in water for a week before they are analysed (yes), or to prepare antibodies a week before they are used (no).
A recurring theme was the utilisation of new technologies in histopathology. Eveline Sjöstedt demonstrated how advances in histopathology can be applied to large scale research projects, presenting an update of progress with the Human Protein Atlas. The largest research project in Sweden, it aims to systematically explore the human proteome through high-throughput generation of affinity-purified antibodies. As well as exploring protein expression levels in normal human cells, the project aims to reveal the changes in protein levels in tumour cells, hopefully identifying new cancer biomarkers. For a project of this scale to work, samples need to be processed en masse in a quick and efficient fashion. As Dr Sjöstedt explained, creating such a high-tech process often means conducting rather low-tech experiments. For example, is it ok to leave slides sitting in water for a week before they are analysed (yes), or to prepare antibodies a week before they are used (no).
Closer to the frontline of medical research, two talks outlined how advances in histopathology are leading to more accurate diagnosis and prognosis for cancer patients. Rebecca Brais, consultant histopathologist for Cambridgeshire NHS, discussed the advances her team have made in pancreatic cancer diagnosis. Pancreatic cancer is paticularly difficult to diagnose; symptoms present late and tumours metastasise early. Worse, biopsies from pancreatic tumours look almost identical to those taken from patients with chronic pancreatitis. Traditionally, pancreatic cancer biopsies have been cytology based but Dr Brais and her team have been pioneering a new histology based biopsy method, which has a considerably higher specificity when assessing if a tumour is malignant or benign. It is also far quicker to assess this type of biopsy (just over 30 minutes per case, compared to over 2 hours for cytology biopsies), resulting in considerable time and cost savings.
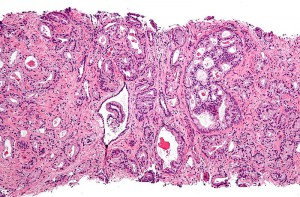
While diagnosis is the big issue with pancreatic cancer, the difficulty with prostate cancer, as Jeremy Clark of the University of East Anglia explained, is making a prognosis. Prostate cancer is present asymptomatically in many men (as Dr Clark put it, you are more likely to die with prostate cancer than of it). Given that removal of the prostate gland is a severe step (resulting in lifelong impotence and incontinence) there is a strong need for a marker to assess the necessity for treatment when prostate cancer is detected. Using FISH analysis of individual chromosomes in prostate tumour biopsies, Dr Clark and his group have identified a gene translocation which, when duplicated, is associated with a poor prognosis. Alongside this, they are developing techniques to collect prostate cells from urine, allowing a prognosis to be made without extracting the prostate gland.
The meeting featured reports of both basic and clinical research, raising the question of how best to bridge the gap between these two research disciplines. Manuel Salto-Tellez discussed this in the context of the translational research lab he has set up at Queen’s University Belfast. The lab links basic research scientists with practising clinicians, with histopathology being the key connection between them. Professor Salto-Tellez also discussed the importance of focusing on tissues as a whole rather than just individual genes when developing new biomarkers.
If there was one thread linking the diverse range of subjects discussed at this meeting it was that, for all the advances created by the development of new technologies and the refinement of old techniques, there is still no substitute, as speaker after speaker stated, for skilled histopathologists. As much as the field is changing then, it seems some things still stay the same.
BMC Clinical Pathology looks forward to seeing the next developments in this ever-changing research area.
Comments