Of the 216 million cases and 445,000 deaths worldwide from malaria in 2016, most are caused by falciparum and, to a lesser extent, vivax malaria. However, two further malaria species, Plasmodium ovale and Plasmodium malariae, are widely distributed through the tropical world.
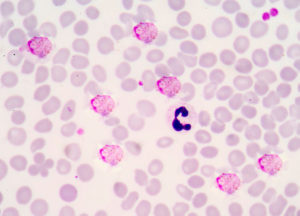
The more common species, P. ovale, causes an estimated 15 million cases of febrile illness each year and probably contributes significantly to the economic burden of malaria. Because this infection is rarely fatal, and is often misdiagnosed microscopically as falciparum malaria, there is relatively little research into ovale malaria.
Because this infection is rarely fatal, and is often misdiagnosed microscopically as falciparum malaria, there is relatively little research into ovale malaria.
Ovale malaria has the ability to relapse many months after initial infection due to the presence of hypnozoites, sleeping forms of the parasite located in the liver.
In imported infections to non-endemic areas, the long latency (the period between initial infection and presentation with symptoms) may result in delayed or missed diagnoses as physicians do not link the fever to travel months or years beforehand. In endemic areas, the hypnozoite forms may reduce the efficacy of elimination efforts.
Relapses make ovale, like vivax, malaria better suited to reduced transmission than falciparum malaria. It is likely to prove more difficult to eliminate and become a greater proportion of malaria as malaria control is achieved.

In this study, we used UK national surveillance data, containing 52,242 cases of imported malaria over a 28-year period, to investigate ovale and malariae malaria imported to the UK. This blog focuses on ovale malaria.
Because the UK is a non-endemic area, we are able to draw conclusions on latent periods and seasonal trends as people are not exposed to reinfection in the UK. These trends would be impossible to establish in endemic zones due to continuous exposure to malaria and the possibility of reinfection. We collated our data with that from the International Passenger Survey to investigate travel and temporal trends.
Because the UK is a non-endemic area, we are able to draw conclusions on latent periods and seasonal trends as people are not exposed to reinfection in the UK.
Ovale infection makes up 6% (3157 cases) of malaria imported to the UK and presents a median of 76 days after leaving an endemic area. Most infection is acquired in West and East Africa and mortality is very low; only one patient is known to have died of ovale malaria in the UK in this 28-year period. This supports UK guidance that the infection can usually be managed as an outpatient.
Imported case numbers remain broadly stable in the UK, but this is on the background of a 380% increase in traveller numbers to West Africa, thus total attack rates fell fivefold between 1993 and 2015 from 0.62 to 0.13 per 1000 trips.
For control efforts the most interesting finding relates to varying latency period. In West Africa, malaria is highly seasonal. We found that patients presenting with ovale malaria in the UK during West African malaria season had a significantly shorter latency than those presenting outside this period. A similar finding has been shown in vivax malaria, which also has a hypnozoite form.
Together, these data suggest that relapse synchronizes with the peak malaria transmission season in the country of acquisition. This is of potential evolutionary benefit to the parasite as it maximise the chance of transmission to mosquito and subsequent human hosts, allowing the parasite to get through periods of low malaria transmission.
This finding was not seen in ovale cases imported from East Africa, where malaria transmission is less seasonal, and may have implications for malaria eradication efforts. The peak in ovale infection during the West African malaria season is probably made up both of increased transmission and increased relapse.
Together, these data suggest that relapse synchronizes with the peak malaria transmission season in the country of acquisition.
Targeting transmission control measures during the malaria season may have a smaller effect on cases than would be expected if relapse happened randomly through the year. Conversely, giving anti-hypnozoite drugs just before the West African malaria season may have a larger effect than predicted if randomness of relapse is assumed.
These results highlight the need for further consideration in control efforts of ovale malaria, a disease of which we know relatively little. This disease may become a major hindrance to malaria eradication efforts unless it is considered as a discrete part of the problem, not just a bystander.
Comments