The Global Polio Eradication Initiative is nearer than ever to eradicating polio, which would make it the second human pathogen to ever be driven extinct, after smallpox. Paralytic polio struck hundreds of thousands of children globally each year when the World Health Assembly announced the push for eradication in 1988, while we are down to only 42 reported cases in 2016.
Paralytic poliomyelitis is caused by three related viruses that are all called polioviruses, so the program could accurately be described as three eradication programs. Of the three types of poliovirus, only Type 2 poliovirus has been certified as eradicated, after not being observed since 1999.
Two vaccines have been instrumental in the achievement of these monumental reductions in paralysis burden: the oral polio vaccine (OPV) and the inactivated polio vaccine (IPV). The inactivated polio vaccine contains killed polioviruses and provides excellent protection against paralysis but not infection, so it is less effective in interrupting poliovirus transmission in a population.
Whenever OPV2 is used, it carries some risk of starting new lineages of vaccine-derived poliovirus; however, the definite need to interrupt the observed transmission always outweighs the possible problem of seeding new transmission.
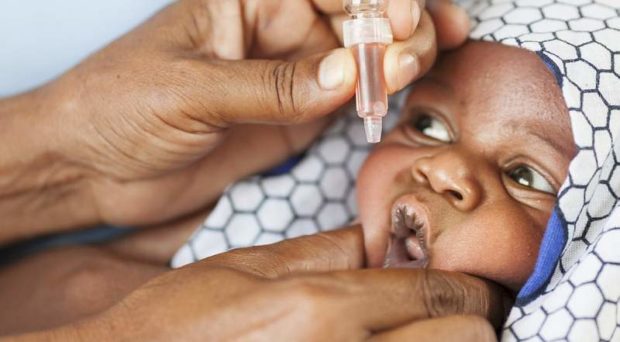
The oral polio vaccine, in contrast, is a live, attenuated vaccine that infects the recipient with a substantially weakened form of poliovirus, inducing much stronger immunity against future re-infection. OPV is also cheaper and simpler to administer than IPV, and so OPV has been the workhorse vaccine in the push for eradication.
While OPV has been an effective and safe tool in the eradication push, it is a form of live poliovirus, albeit substantially weakened. In populations with low immunity and poor sanitation or overcrowding, the OPV virus strains can transmit between people, and can evolve back to a stronger virus more like wild poliovirus. When this occurs, the resulting virus is called a vaccine-derived poliovirus. The final stage of the polio eradication endgame thus involves the global withdrawal of OPV, so that neither wild nor vaccine-derived polioviruses survive.
Because wild Type 2 poliovirus has not been seen in 18 years, the Type 2 vaccine (OPV2) was the first OPV strain to be withdrawn, in April 2016. However, OPV2 must still be deployed in response to any observed circulation of vaccine-derived poliovirus. The tension here is clear: whenever OPV2 is used, it carries some risk of starting new lineages of vaccine-derived poliovirus; however, the definite need to interrupt the observed transmission always outweighs the possible problem of seeding new transmission. To help policymakers prepare for this eventuality and manage this trade-off, we set out to quantify the risk of OPV2 use over time.
Modeling disease transmission
This risk depends on many unknown factors: for example, how likely OPV2 recipients are to infect non-immune people they contact, how quickly OPV2 recovers wild-type properties through evolution, and how frequently people move between communities around the outbreak response. We evaluate this risk under these uncertainties by modeling a set of poliovirus transmission scenarios. In each, we vary these unknowns over values consistent with historical clinical data, field studies, and past polio outbreaks.
In each scenario, we evaluate the probability that the OPV2 virus will survive by transmitting, and how this probability grows over time as more unimmunized children are born.
The disease model investigates OPV2 transmission among populations in West Africa. This is one region among a few where polio eradication has proven particularly difficult, and focusing here allows us to leverage past work calibrating the model in this region. Each population initially has immunity consistent with their local vaccination history. New individuals are born susceptible to infection and are individually tracked through life as they age, travel to other regions, and possibly become immune through vaccination or infection. OPV2 is deployed into one of these populations after some time has passed, and recipients may transmit the virus to non-immune contacts.
In each scenario, we evaluate the probability that the OPV2 virus will survive by transmitting, and how this probability grows over time as more unimmunized children are born. In the most pessimistic scenarios, OPV2 virus frequently survives as soon as 18 months after OPV2 withdrawal; under more optimistic assumptions, it may be 4-5 years before the virus is likely to survive.
There are ways to mitigate this risk. As this risk only grows over time, it is critical to maintain intense disease surveillance to catch transmission as soon as possible, particularly focusing where medical systems are impaired by violence or social upheaval. Upon discovery of virus, rapid and widespread response with OPV2 provides the best chance of both interrupting the observed transmission and raising local immunity enough to minimize onward transmission of OPV2.
Remnant vaccine-derived Type 2 lineages have already been discovered (1, 2, 3), and outbreak responses are ongoing. The success of these responses is critical to the final stages of polio eradication. What we learn will also inform strategies for the future withdrawal of OPV Types 1 and 3, after certified eradication of the wild viruses. The polio eradication initiative is in its endgame phase, and despite continuing challenges, we remain optimistic that the work of the thousands of dedicated individuals in this program will succeed, and we look forward to a polio-free world.
Comments