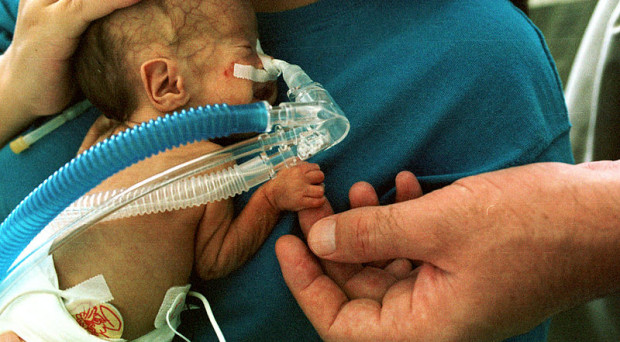
Short term outcomes, such as brain hemorrhage, oxygen dependency, duration of hospital stay, and mortality of pre-term infants, are influenced by a wide range of factors. These include gestational age, birth weight, sex, antenatal factors, and the condition of the infant at birth and during the first few hours of life.
Administration of antenatal steroids, use of surfactant, better temperature control and humidity have all contributed to improved survival of these babies. On the other hand, poorly-controlled maternal hypertension during pregnancy, perinatal infection, and fetal distress are known to be risk factors for worse outcomes.
The normal hemoglobin level at birth for preterm infants varies from 15-20g/dl. These levels and blood volume of the infant can be improved by delaying clamping of the umbilical cord for 30 to 120 seconds at delivery. Though the increased blood volume is noted soon after delivery, the raised hemoglobin becomes apparent after several minutes to hours following birth.
Providing additional placental blood to the preterm infant by delaying clamping of the umbilical cord appears to be associated with better stability of the circulatory state, and reduced risk of respiratory distress syndrome, brain hemorrhage, necrotising enterocolitis, and requirement for blood transfusion. However, this has not shown to have improved survival of preterm infants and thus this was the aim of our study.
We studied the relationship between hemoglobin level at birth and short term outcomes, as well as mortality of preterm infants. The study included babies who were born at ≤ 32 weeks at Homerton University Hospital, London. There were nearly 900 infants in the study with a mean gestational age of 28.3 weeks and birth weight 1,140g (about 2.5lbs).
Low hemoglobin levels at birth were associated with worse outcomes.
Low hemoglobin levels at birth were associated with worse outcomes such as brain hemorrhage, necrotising enterocolitis, oxygen dependency at 36 weeks (post conceptional age), retinopathy of prematurity, and death before discharge from neonatal unit.
After adjusting for severity of prematurity and birth weight, the low hemoglobin was still associated with increased mortality. The risk of mortality was increased four-fold if the hemoglobin level at birth was 18g/dl. Low levels were also associated with risk of receiving a blood transfusion but weren’t associated with the duration of the hospital stay or the number of days in intensive care.
Our research has therefore shown that low hemoglobin levels at birth are associated with mortality and the need to receive blood transfusions in babies born at less than 32 weeks of gestational age. Delaying umbilical cord clamping at delivery could be used to improve an infant’s blood volume and hemoglobin level which may improve overall survival for babies in the group investigated.
The association between hemoglobin level at birth and long-term neurodevelopmental outcomes still needs further research. In the meantime, measurement of hemoglobin levels at birth could be incorporated into mortality prediction scores such as Clinical Risk Index for Babies (CRIB) and Score For Neonatal Acute Physiology (SNAP) to further increase the sensitivity of prediction.
Comments