This week, the National Institutes of Health (NIH), 10 biopharmaceutical companies and several non-profit organizations launched an unprecedented partnership to transform the current model for identifying and validating the most promising biological targets of disease for new diagnostics and drug development.
Currently in the US, developing a drug from early discovery through Food and Drug Administration (FDA) approval takes well over a decade and has a failure rate of more than 95%. As a consequence, each success can cost $1 billion or more. It was therefore recognised that new approaches were required, and that collaborative efforts might be a way to increase the collective odds of success.
Through the Foundation for the NIH, the Accelerating Medicines Partnership (AMP) will invest more than $230 million over five years in the first projects, which focus on Alzheimer’s disease, type 2 diabetes, and the autoimmune disorders rheumatoid arthritis (RA) and systemic lupus erythematosus (SLE).
Alzheimer’s disease
Alzheimer’s disease (AD) is the most common form of dementia. As people are living longer than ever before, dementia is a growing public health problem that affects over 30 million people worldwide – a figure predicted to double by 2030, according to the World Health Organization.
The development of biomarkers for AD, specifically peripheral biomarkers that require less invasive tests, has seen a revival of interest. However, despite progress in recent years, a validated set of biomarkers still has not emerged. The AMP is focusing on identifying biomarkers to provide early diagnosis and so allow for treatments that may delay or prevent AD.
The journal Alzheimer’s Research & Therapy has recently published a special series on Peripheral Biomarkers, exploring current issues in the search for blood biomarkers and discussing biomarker approaches that have already produced data that may help to advance the field. New research published in the series includes a paper highlighting the level of calmodulin as a potential biomarker for mild-AD and in differentiating it from other types of dementia, as well as research exploring the platelet membrane proteome as a source of blood-based biomarkers in AD. View the full series here.
The AMP also aims to conduct large-scale, systems biology analyses of brain tissue samples of human patients with AD to validate biological targets that play key roles in disease progression. This should increase the understanding of molecular networks involved in the disease to help identify new potential therapeutic targets.
Autoimmune disorders
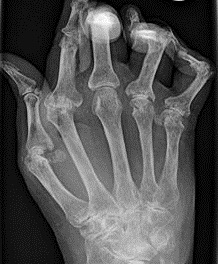 The field of rheumatology has seen many advances in the knowledge of disease mechanisms in RA and SLE. Both are autoimmune disorders with flaws in immune function and regulation; symptoms include joint pain and swelling, fatigue and periodic fever.
The field of rheumatology has seen many advances in the knowledge of disease mechanisms in RA and SLE. Both are autoimmune disorders with flaws in immune function and regulation; symptoms include joint pain and swelling, fatigue and periodic fever.
Most people with RA have only a partial response to available drugs, so there is a need for further development. A study published last year in the journal Arthritis Research & Therapy found that a hepatocyte growth factor antagonist (NK4) inhibits inflammatory cytokine production by CD4+ T cells, thus highlighting its potential use in the treatment of RA. Spleen tyrosine kinase (SYK) inhibition is another promising avenue for treatment and a novel orally bioavailable small molecule inhibitor was recently developed. In the case of SLE, no effective targeted therapies exist for the most severe forms. However the disease has a complex self-perpetuating cycle, which creates opportunities for targeted treatment inventions at multiple steps.
The AMP will integrate several new or developing technologies to analyse cells involved in autoimmunity in new ways; collecting tissue (e.g. synovium) samples for molecular analysis, and developing computational tools to integrate different data types to characterize molecular pathways. The data could facilitate the identification and validation of biological targets for other autoimmune diseases, such as multiple sclerosis and Crohn’s disease.
Open access
With a focus on expediting translation of scientific knowledge into next generation therapies, the AMP has agreed that all generated data and their analyses will be made publicly available to the broader community.
This is a key mission shared by the open access journals Arthritis Research & Therapy and Alzheimer’s Research & Therapy. To keep up to date with the latest articles and news from these journals, follow us on Twitter: @ArthritisRes, @AlzheimersRes.
Comments