 In an exciting research article published today in Genome Medicine, Andrew Teschendorff and colleagues provide evidence that the risk of cancer can be predicted by analyzing DNA methylation patterns in cells collected years in advance of the onset of disease. Their approach could provide the basis for a new clinical test with the ability to predict cancer risk in cells that appear morphologically normal.
In an exciting research article published today in Genome Medicine, Andrew Teschendorff and colleagues provide evidence that the risk of cancer can be predicted by analyzing DNA methylation patterns in cells collected years in advance of the onset of disease. Their approach could provide the basis for a new clinical test with the ability to predict cancer risk in cells that appear morphologically normal.
 In this study, researchers from University College London, Innsbruck Medical Universityand Central Manchester University Hospitals sought to determine whether normal cells collected from cancer patients prior to disease development have genomic markers that can predict future risk. Specifically, the authors focused on DNA methylation markers, which together with other types of chemical modification of DNA known collectively as epigenetic changes, are thought to contribute to the initiation and progression of complex diseases such as cancer.
In this study, researchers from University College London, Innsbruck Medical Universityand Central Manchester University Hospitals sought to determine whether normal cells collected from cancer patients prior to disease development have genomic markers that can predict future risk. Specifically, the authors focused on DNA methylation markers, which together with other types of chemical modification of DNA known collectively as epigenetic changes, are thought to contribute to the initiation and progression of complex diseases such as cancer.
The researchers applied their analysis to cervical cancer, which represents a unique model for conducting prospective studies of this kind, due to the availability of cytologically normal cells collected before cancer onset. Cervical cell samples were taken from women aged 19-64 years who had undergone two rounds of cervical cancer screening within a three year interval, as part of the ARTISTI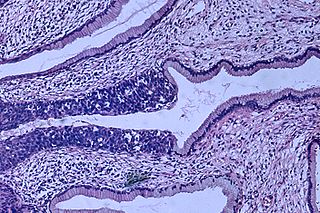 C trial. Teschendorff and colleagues found differences in the DNA methylation profiles of cells collected from women who had developed cervical cancer after three years, compared with those who had remained disease-free. Applying a novel statistical method, the authors show that the risk of cervical cancer can be predicted in independent data sets on the basis of these cellular DNA methylation differences. They conclude that DNA methylation changes, in combination with human papilloma virus (HPV) infection, are a key factor in determining cervical cancer risk.
C trial. Teschendorff and colleagues found differences in the DNA methylation profiles of cells collected from women who had developed cervical cancer after three years, compared with those who had remained disease-free. Applying a novel statistical method, the authors show that the risk of cervical cancer can be predicted in independent data sets on the basis of these cellular DNA methylation differences. They conclude that DNA methylation changes, in combination with human papilloma virus (HPV) infection, are a key factor in determining cervical cancer risk.
This research lends further support to studies indicating that epigenomic variation is associated with complex disease risk, particularly cancer. In addition, the landmark study suggests that early screening of methylation changes in normal cells could be useful for predicting the risk of future neoplastic transformation. This finding could have implications for the development of preventive strategies and improved clinical diagnostic tests.
One Comment