
Every year mosquito-transmitted viruses such as Dengue, Chikungunya and, most recently, Zika cause several hundred million infections. The unpredictable nature of these outbreaks, combined with the enormous genetic diversity of these viruses, makes it challenging to prepare vaccines or antivirals for current and future threats. Currently there are very few vaccines and no antiviral drugs available for treatment. Wouldn’t it be great to have a common strategy against many of these viruses?
One thing most of these viruses have in common is that they are transmitted by a limited number of Aedes mosquito species, especially Ae. albopictus and Ae. aegypti. These mosquitoes are rapidly increasing their territories due to climate change and globalisation, facilitating the large outbreaks of viruses such as chikungunya and Zika we’ve seen in the past decade.
It had been observed by several research groups that the presence of a mosquito bite, or even just saliva, increased viral dissemination and morbidity.

My colleagues and I at the University of Leeds have just published results of our investigation into the mechanism underlying this intriguing observation.
Our model system
To investigate the impact of mosquito bites, we allowed Ae. aegypti to bite a small piece of mouse skin. Bitten or resting skin was then injected with a very small volume of mosquito-cell derived Semliki Forest virus. This way, we mimic natural infection in a highly reproducible model.
How the immune system benefits the virus
We found that the rapid, local immune response to the mosquito bites is actually beneficial for the virus. An oedematous bump, well known to occur after a mosquito bite, retains virus in the skin. Here, a strong innate immune response is orchestrated to fix the damage caused by the mosquito bite. However, unwittingly this immune response also results in giving the virus an early and powerful advantage.
This boost in viral infection by mosquito bites is due to the recruitment of immune cells. The first round of recruited cells are the neutrophils. These highly mobile cells come in very early to initiate tissue repair and fight off infection. Neutrophils do not seem to become infected themselves, but do contribute to oedema which retains the virus in the skin.
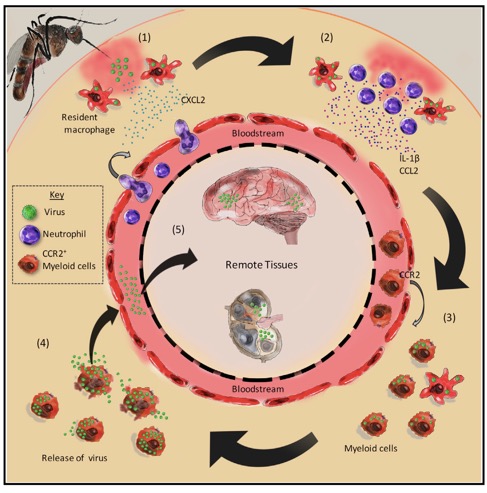
The recruitment of a second wave of immune cells, the monocytes and macrophages then occurs. Macrophages gobble up anything possibly dangerous to initiate a suitable immune response. However, these macrophages become infected and produce large amounts of virus which contributes to the spread of virus around the body, including to the brain, where they cause disease in our mouse model.
How to prevent this
When we depleted neutrophils with an antibody, or prevented migration of macrophages into the bite site by using a knockout mouse with immobile macrophages, we blocked bite-enhancement.
We investigated whether bite-enhancement was a direct effect of the mosquito saliva by comparing its potency to various inflammatory drugs that recruit similar cell types via completely different mechanisms. This included a synthetic mimic of bacterial lipoprotein (PAM3CSK4) and the vaccine adjuvant alum. Interestingly, mosquito saliva enhanced viral infection in a manner similar to these tested compounds.
We thought this early and local immune response might give us a useful target for prevention of disease. Therefore, we tested this idea by targeting one of the components of this local immune response, the potent pro-inflammatory molecule IL-1ß, by pre-treating the mice with a blocker that prevents activation of IL-1ß.
We were able to reduce the bite enhancement effect and improve disease outcome by inhibiting the inflammatory response that occurs at the bite site.
A potential future clinical application of these findings
Our current research focuses on improving our understanding of early events in the bitten skin and what aspects of mosquito bites impact local inflammation. In addition, we are testing ways to modulate this early immune response to improve disease outcome.
As these viruses are mainly transmitted by the day-biting Ae. albopictus and Ae. aegypti, it is likely you would notice that you have been bitten within a few hours. This could provide a time window that is long enough to modulate the early immune response, for instance by applying a cream. Although it is best not to get bitten at all, we hope that applying anti-inflammatory cream onto mosquito bites could prevent bite-enhancement and thus reduce disease caused by many different viruses.

One Comment