To date, humans have uncovered a number of natural principles and issues such as the origin and mysteries of the universe, the earth and even life. We have simultaneously developed innumerable non-natural products for human use.
However, we have not yet succeeded in creating a man-made, cost-effective alternative to red blood cells (RBCs) despite the performance of extensive research and numerous clinical trials.
A life-saving intervention
The cellular health of the host requires an oxygen (O2) supply that matches the O2 requirements of its tissue. An insufficient O2 supply results in ischemia, subsequently inducing tissue and/or organ injury, frequently observed in critically ill patients.
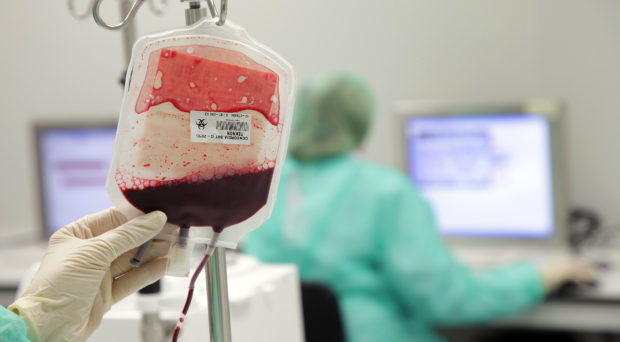
RBC transfusion, first performed over 300 years ago, remains a fundamental life-saving intervention in medicine.
Hemoglobin, which is enclosed in RBCs as an O2 carrier, plays the most important role in supplying O2 to the tissues. Accordingly, RBC transfusion, first performed over 300 years ago, remains a fundamental life-saving intervention in medicine.
Until the early 1980s, RBC transfusion was considered to be practically risk-free and a truly effective intervention in patients with active bleeding or anemia due to a variety of reasons in the intensive care field.
However, the threat of potentially-fatal transfusion-related infections, i.e., human immunodeficiency virus, has led physicians throughout the world to obviate this conventional intervention to the extent that is possible.
Research in the literature
In 1999, Canadian investigators examined the effects of a restrictive RBC transfusion strategy in comparison to a liberal strategy in critically ill patients. They indicated that a restrictive strategy was at least as effective as and possibly superior to a liberal transfusion strategy in critically ill patients with some exceptions.
Although several debates are currently ongoing, most physicians now agree that a restrictive strategy to limit RBC transfusion is a valuable approach in the treatment of stable patients with anemia.
However, we need to be cautious when interpreting the results of the Canadian study as it indicated some exceptions.
Even though we have seen extraordinary advances in medical science and related technology over the last several decades, clinical practices have been determined based on the balance between the benefits and related risks of intervention.
They found that a restrictive transfusion strategy was significantly associated with reduced mortality in younger patients and in those with less severe conditions. In other words, a liberal RBC transfusion strategy might be more effective for older patients and patients with more severe conditions.
Even though we have seen extraordinary advances in medical science and related technology over the last several decades, clinical practices have been determined based on the balance between the benefits and related risks of intervention.
RBC transfusion by itself is not an exception. The level of hemoglobin that works in some patients may not work in others. Indeed, a previous cohort study of intensive care unit patients suggests that restrictive RBC transfusion policies may not be uniformly applicable in the clinical setting.
World Blood Donor Day
In 2012, the World Health Organization (WHO) released a document entitled, “Blood donor selection – Guideline on assessing donor suitability for blood donation”. In this guideline, the authors noted that a careful process to assess the suitability of donors is essential for protecting the safety and sufficiency of the blood supply, and safeguarding the health of both ‘recipients’ and ‘donors’. We should therefore understand that blood transfusion not only improves the recipients’ conditions but also affects the donors’ health.
Away from the discussion of whether restrictive or liberal RBC transfusion strategies should be applied, natural human blood is needed to save the lives in emergency and long-term treatment settings, even in the 21st century.
If you believe yourself to be in good health, you should donate your blood to prove it and to save lives at the same time.
Comments