
We are approaching the 100th anniversary of the demonstration that the brain is an oscillatory organ, and the first recording of a human electroencephalogram (EEG). German psychiatrist Hans Berger was a keen observer who recognized that the first oscillations he detected (eponymously named ‘Berger waves’, and later ‘alpha waves’) were reactive to the stimulation of the patient, and sensitive to the presence of illnesses such as dementia.
The enthusiasm generated by Berger’s discovery soon gave way to skepticism: his interest in cerebral energetics and psychic phenomena led him to speculate about using EEG to quantify the energy of a human thought, and transmitting thoughts from one individual to another.
For much of the past 100 years, the relationship between psychiatry and the study of cerebral oscillatory activity continued to be marked by swings from enthusiasm (generated by exciting research findings) to skepticism (generated by the challenge of relating results to fundamental brain processes).
Electrophysiology research arguably generates more research results than any other brain imaging technology, owing to the low cost of performing EEG studies and the low burden on research subjects. Interpretation of the results of these studies, however, has consistently been bedeviled by the absence of a consistent physiologic framework in which to interpret results.
Recognizing the function of brain oscillations
This situation has begun to change as we recognize that the major function of synchronized brain oscillations is to organize brain networks. Mood and thought are not just chemistry – they are oscillations, and patterns of oscillation may help to diagnose psychiatric illness and predict response to treatment.
In the Neuromodulation Division at the University of California, Los Angeles, we are testing the hypothesis that the mechanism of action of antidepressant treatments arises from their ability to reshape brain networks by altering patterns of rhythmic oscillations.
Neuromodulation treatments such as transcranial magnetic stimulation may act at the level of brain networks, exerting ‘top down’ influences to change neuronal firing patterns and neurochemistry. Meanwhile, antidepressant medications may act at the level of the synapse, exerting ‘bottom up’ influences on firing patterns to reshape brain networks. Changes in oscillations may be the bridge across multiple levels of complexity in the brain, transmitting treatment effects bidirectionally between synapses and whole brain networks (see figure below, click on the image to enlarge it).
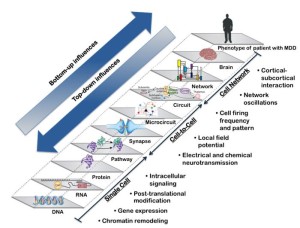
A continuum of factors contributes to the depressive phenotype in major depressive disorder, ranging from genetic polymorphisms through function in brain networks.
The multiple levels of biological structures, ranging from the genome to brain networks and ultimately culminating in the phenotype(s) of major depressive disorder, represent a spectrum of increasing biological complexity (shown in the center of the diagram from bottom left to top right).
These structures can be grouped into three general categories of organization: those existing at the level of the single cell, those involving cell-to-cell communication, and those involving ensembles of cells that form circuits and networks.
Each of these categories of structural organization is characterized by certain physiologic functions, shown on the right. The three levels of structural and functional organization are not entirely autonomous: the effects of genetic and molecular factors are translated bottom up to influence the clinical phenotype of major depressive disorder, whereas the influence of brain functional networks are translated top down to influence cellular communication and intracellular processes.
The spectrum of structures and functions presented in the figure are intended to be illustrative of general physiologic principles and are not an exhaustive list of structural and functional features of interest in major depressive disorder.
An opportunity to push the boundaries of our knowledge
This is an exciting time for electrophysiologic research in psychiatry. We have the potential as never before to understand the role of oscillations in brain health and disease. It is in this rich research milieu that we are launching the new journal Neuropsychiatric Electrophysiology.
We welcome your original research contributions and thoughtful reviews of the literature to push the boundaries of our understanding of how electrophysiologic techniques can enhance our effectiveness in treatment of neuropsychiatric illnesses.
Comments