
BMC Medicine is now welcoming submissions for an article collection on childhood malnutrition
Mental health
Both obesity and mental health are chronic conditions; but are they associated? Dr. Charlotte Hardman presented data from the Millennium cohort study, which includes more than 19,000 children born between 2000 and 2002. By conducting mental health and anthropomorphic assessments at different time points, her group showed a gradual increase in emotional problems and obesity throughout childhood and adolescence, with significant comorbidity at ages 11 and 14 relative to earlier years. These findings serve to highlight the importance of early intervention.
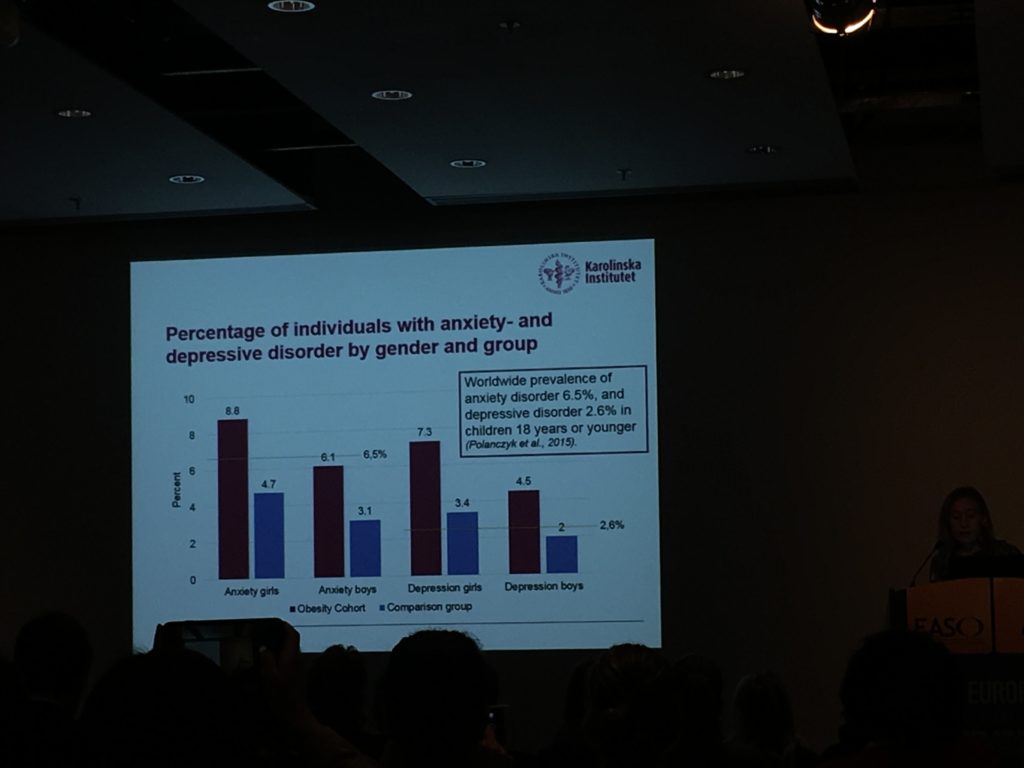
Dr. Louise Lindberg presented a Swedish nationwide study of children aged 6-17 years to assess the association between obesity and anxiety/depression, using the Swedish Childhood Obesity Treatment Register. This study revealed both anxiety and depression to be more prevalent in obese children compared to the general population. The associations remained in sensitivity analyses, suggesting that obesity is an independent risk factor for these conditions.
Dr. Kajsa Järvholm investigated these associations in adolescents undergoing bariatric surgery, through the Adolescent Morbid Obesity Surgery (AMOS) study. Five years post baseline, the surgery group had received significantly more psychiatric drug treatment. Continued, repeated monitoring of mental health is necessary in adolescents to assess the long-term outcomes of bariatric surgery.
Precision nutrition and macronutrients
Prof. Iris Shai provided a great update on the field of precision nutrition, noting that intra-individual differences in response patterns. The Mediterranean diet was shown to mobilize specific ectopic fat deposits (visceral, hepatic, cardiac and pancreatic fats –the most sensitive organs for weight loss); however, total weight loss was the same as those not on this diet. There are also gender differences in the response to diet; for instance, both are likely to experience similar weight and waist circumference changes, but men tend to lose more visceral and deep-subcutaneous fat deposits than women (who have more subcutaneous fat to begin with).
With respect to macronutrients, Dr. Carlos Celis-Morales discussed the association between macronutrient intake (fat, carbohydrates and sub-types) and risk of all-cause mortality and cardiovascular disease, using data from the UK Biobank. Lower intake of protein, starch, mono- and polysaturated fats and fibre and higher intake of sugar and saturated fat are associated with higher risks for both outcomes. At the other end of the spectrum, higher intake of protein and lower intake of fibre are also associated with higher risks for these outcomes. Based on the findings, they developed risk matrices for the outcomes based on quantity of macronutrient intake.

ACTION-IO
A number of participants in the ACTION-IO project presented results from this interesting survey. ACTION-I0 is an 11-country project looking at the barriers to effective obesity care by surveying both patients and health care providers, and the results thus far show discrepancies. 81% of people with obesity think weight loss is their responsibility, whilst only 30% of health care providers concur; likewise, 81% of people of obesity say they have made at least one serious effort to lose weight in the past, but health care providers feel this is only true for 35% of them.
One of the most striking results, however, is that it takes people with obesity ca. 6 years to have their first discussion about their weight with a health care provider. Additionally, 68% of people with obesity consider obesity a chronic disease, whilst this percentage is 88% for health care providers. This misalignment in perceptions clearly needs to be resolved.

COSI report
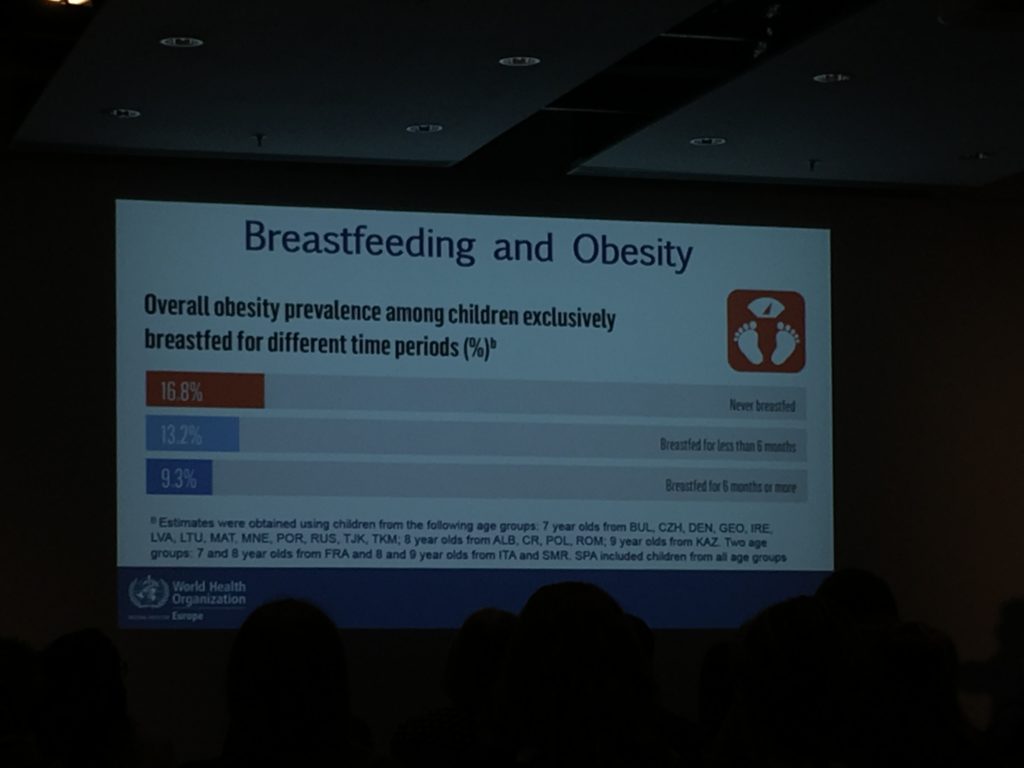
Representatives from the WHO presented results from the global COSI (Childhood Obesity Surveillance Initiative). The two reports presented examined the association between breastfeeding and obesity, and the prevalence of severe obesity amongst school-aged children. The findings highlighted a protective effect of breastfeeding against obesity; in particular, obesity is less prevalent in those who are breast fed for at least 6 months. Additionally, there are global differences in the prevalence of severe obesity – being particularly high in Southern Europe. Prevalence was also higher in boys.
This was an excellent meeting, highlighting the importance of recognising obesity as a chronic disease; promoting the benefits of breast feeding; evaluating the impact of the food industry on obesity; and valuing the patient perspective (with the launch of the European Coalition for People living with Obesity).
BMC Medicine is now welcoming submissions for an exciting new article collection on childhood malnutrition: ‘Stunting, undernutrition and obesity: the triple threat of childhood malnutrition’. We invite primary research articles and front-matter content investigating the problems and underlying mediating factors of this global health issue, and highlighting the impact of potential solutions.
Comments