Blood marker predicts cognitive decline
A new blood marker associated with Alzheimer’s disease has been identified in a study of more than 200 twins. The researchers conducted proteomic analyses of plasma samples, and compared the results with cognitive function tests over the following decade.
People think it may be hard to reverse 20 years of potential damage to your brain…but if you could start much earlier in that process, then you might be able to find something that works
Dr Steven Kiddle
Levels of one protein, the mitogen-activated protein kinase MAPKAPK5, were found to be reduced in those with lower scores in cognitive function tests. While longer follow-up is required to assess whether MAPKAPK5 levels predict the development of Alzheimer’s disease, these results suggest that the protein is a promising early biomarker.
The global incidence of dementia is expected to treble by 2050, and blood-based predictive biomarkers are urgently needed so that the disease can be identified at the earliest possible stage. Lead author Dr Steven Kiddle explained that:
“People think it may be hard to reverse 20 years of potential damage to your brain…but if you could start much earlier in that process, then you might be able to find something that works”
Kiddle et al., Translational Psychiatry
Identifying COPD in primary care
Chronic obstructive pulmonary disease (COPD) is a major cause of disability and death worldwide, but opportunities to diagnose COPD are often missed. Now, UK researchers have developed a risk score to identify COPD in primary care.
The study analyzed patient records from almost 500 primary care practices across the UK, and COPD risk factors were identified.

These risk factors were then used to create a score – taking variables including smoking status, comorbidities, infection and medication use into account – which was then validated in an external sample.
As this new score is based on routinely-recorded information, following further validation it could be used to identify those at high risk of COPD for referral to specialist investigation.
Haroon et al., BMJ Open Respiratory Research
Is hormonal contraceptive use linked to herpes infection risk?
New findings from a study conducted in Uganda suggest that use of the injectable hormonal contraceptive DMPA could increase the risk of herpes simplex virus 2 (HSV2) infection. While there is a known association between DPMA and HIV infection, its impact on the acquisition of other sexually-transmitted diseases (STD) is less well understood.
In the Ugandan study, women who were HIV-negative and HSV2-negative at baseline were assessed annually for HSV2 infection, and those using DMPA were found to have significantly increased risk of HSV2 infection compared with those who were neither pregnant nor using hormonal contraception.
These findings provide further evidence of an association between hormonal contraceptive use and STD risk in sub-Saharan Africa, and the authors emphasize that access to a wide choice of contraceptive methods should be a public health priority.
Grabowski et al., The Lancet Global Health
Overcoming resistance in metastatic melanoma
Survival rates in those with melanoma have increased dramatically in recent years, owing to the development of targeted therapies such as vemurafenib. However, many patients become resistant to vemurafenib after a few months, and research efforts are currently directed at identifying how we can overcome treatment resistance.
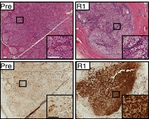
Now, researchers have conducted an extensive analysis of vemurafenib resistance in a patient with metastatic melanoma. Using whole-exome sequencing, they found a plethora of mechanisms underlying resistance, with different mechanisms occurring in distinct metastases. Additionally, patient-derived xenograft experiments revealed that many mechanisms of resistance occur within each metastatic tumor.
Taken together, these findings highlight heterogeneity in the pathways underlying vemurafenib resistance in metastatic melanoma, and suggest that multiple mechanisms must be targeted to overcome resistance and improve clinical outcomes.
Kemper et al., EMBO Molecular Medicine
Telomere shortening in schizophrenia
Telomere shortening occurs in a number of age-related diseases, including diabetes, cardiovascular disorders, and Alzheimer’s disease. New research conducted in Poland suggests that telomere length could also play a role in schizophrenia.
The authors measured telomere length in blood cells taken from patients with early and chronic schizophrenia. The severity of symptoms and number of hospital admissions were found to correlate with telomere length, and a model taking disease duration, sex, age, hospital admissions and psychotic episodes into account revealed an association between these factors and telomere length.
These preliminary findings suggest that psychotic symptoms could be linked to telomere shortening, providing a possible explanation for why those with schizophrenia have a shorter life expectancy. The authors conclude that:
“The connection between chronicity and severity of schizophrenia and telomere length, as well as the possible consequences, premature cellular senescence, and increased cardiovascular mortality risk, reinforce the need for effective therapy of schizophrenia”
Comments