Dementia is a growing public health problem that affects over 30 million people worldwide – a figure predicted to double by 2030, according to the World Health Organization. Providing quality care for this population is an issue that health care authorities all around the world are facing.
Evidence-based practice recommendations can aid physicians in diagnosing and managing dementia, which can be difficult and time-consuming. Having useable guidelines can ultimately result in better care for patients.
Members of the 4th Canadian Consensus Conference examined available evidence to reach a consensus on final recommendations for scientists working globally in the field. A new supplement published in Alzheimer’s Research & Therapy contains free-to-access background papers that support each recommendation made by the group.
In an introductory article, Supplement Editor Serge Gauthier explains each topic that was examined, which includes:
Neuroimaging
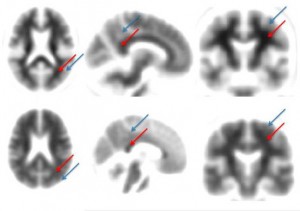 The neuroimaging group engaged in a comprehensive review of existing and developing technologies. Despite the extremely promising nature of amyloid imaging, the group advised against widespread clinical adoption of this modality until its role in diagnosis and prognosis can be more fully understood. Its use in cognitively normal individuals is particularly fraught with ethical and practical hazards. Recommendations about directions for future research in magnetic resonance imaging (MRI) (functional MRI, MR spectroscopy etc.) and amyloid imaging is also explained.
The neuroimaging group engaged in a comprehensive review of existing and developing technologies. Despite the extremely promising nature of amyloid imaging, the group advised against widespread clinical adoption of this modality until its role in diagnosis and prognosis can be more fully understood. Its use in cognitively normal individuals is particularly fraught with ethical and practical hazards. Recommendations about directions for future research in magnetic resonance imaging (MRI) (functional MRI, MR spectroscopy etc.) and amyloid imaging is also explained.
Diagnostic criteria
Many changes to the diagnostic criteria for the dementias and prodromal conditions have been advanced in recent years. The definitions group recommended the adoption of the diagnostic criteria of the National Institute on Aging/Alzheimer’s Association (NIA/AA) Working group for dementia, probable and possible Alzheimer’s disease (AD) and mild cognitive impairment due to AD.
Therapeutics
The pharmacology group reported that while there have been no new cognitive enhancing pharmacological agents approved for use since the last consensus conference in 2007, the role of cholinesterase inhibitors in severe AD and dementia associated with Parkinson’s disease is now established. Recognizing the increased incidence of strokes and all cause mortality associated with antipsychotic medications in people with dementia, recommendations are made based on the balance of risks and benefits to the individual or others.
Knowledge translation
Despite the expanding need for physicians to have access to usable evidence-based practice recommendations, Knowledge Translation (KT) is often seen as a daunting, if not confusing, undertaking for researchers. The KT group offer a brief introduction to the processes around KT including terms and definitions, and outline some common KT frameworks including the Knowledge to Action Cycle, and the PARiHS and CFIR frameworks. Practical steps are also outlines for planning and executing a KT strategy, particularly around the implementation of recommendations for practice.
Early onset dementia
The early onset dementias (EOD) group recommended a broader differential diagnosis for EOD compared to late onset dementia, as delays in diagnosis are common, and result in an increased social impact that requires special care teams. The etiologies underlying EOD syndromes should take into account the family history and comorbid diseases, such as cerebrovascular risk factors, that may influence the clinical presentation and age at onset. A ‘personalized medicine’ approach to diagnosis should be considered depending on the age at onset, clinical presentation, and comorbidities. This background paper will be published in the supplement shortly.
For more information on Alzheimer’s Research & Therapy, or to submit a manuscript, please visit the journal website or contact the Editorial Office. To keep up to date with the latest articles published in the journal, sign up for Article Alerts and follow us on twitter.

Comments