
Over the past two decades, the global community has achieved remarkable progress on infant and child health. Since 1990, the under-five mortality rate has fallen by half, while the share of children receiving basic vaccines has increased across the board.
Still, around 5.9 million children die each year before reaching their fifth birthday, including 4.5 million that die in the first year of life. Newborn babies are especially vulnerable to infections. Currently, 19.5 million children are missing key immunizations, leading to preventable illness and death. What’s more, progress on global vaccination coverage has come to a standstill at 86%.
Currently, 19.5 million children are missing key immunizations, leading to preventable illness and death
Similarly, although breastfeeding is widely acknowledged as one of the single most effective infant health interventions, just 45% of infants are exclusively breastfed for the first six months, as recommended by the World Health Organization (WHO). Recent estimates suggest that universal breastfeeding could prevent 800,000 child deaths per year, while a substantial body of research has shown that breastfeeding protects against infections and malnutrition and improves children’s neurocognitive development.
The Sustainable Development Goals (SDGs), which were unanimously adopted by all 193 UN Member States in 2015, call on countries to “end preventable deaths of newborns and children under 5 years of age” and to reduce disparities in illness rates. As the global community aims to fulfill these promises by 2030, what more can be done?
Overcoming barriers
Remarkable public health campaigns promoting immunizations and breastfeeding dramatically increased both practices—yet too many children are still left behind due to social conditions that prevent parents from pursuing these key measures. Long work hours without leave or flexibility can make it impossible for parents to bring children to clinics for immunizations.
Requirements to return to work full-time shortly after giving birth, with neither infant care nearby nor the ability to pump and refrigerate breastmilk, create insurmountable barriers to breastfeeding for millions of families. To accelerate progress in the coming decades, countries must do more to address the ways the social and economic environments constrict or promote parents’ ability to provide care.
Ensuring that all parents receive paid leave from work during the first year of life is an important step in this direction; across economies, paid leave has been found to reduce infant mortality. In a 2016 study of twenty low- and middle-income countries, each additional month of paid maternity leave was associated with a 13% reduction in infant deaths. Two likely contributors to this effect are that paid leave enables parents to take their infants to the clinic for critical immunizations and post-natal care and that it supports mothers to breastfeed longer.
For both purposes, the length of leave matters. In a 2015 study, researchers found that each additional week of paid maternity leave increased the probability that an infant would receive the third dose of the DTP vaccine, which is typically administered no earlier than 14 weeks, by 2.17 percentage points. By contrast, the study did not find a significant relationship between increases in paid maternity leave and the probability of children receiving the BCG vaccine, which is typically administered right after birth before the infant leaves the hospital. The findings suggest that paid parental leave can improve vaccination uptake in the countries where it’s needed most, and that more generous leave policies have the greatest potential for impact.
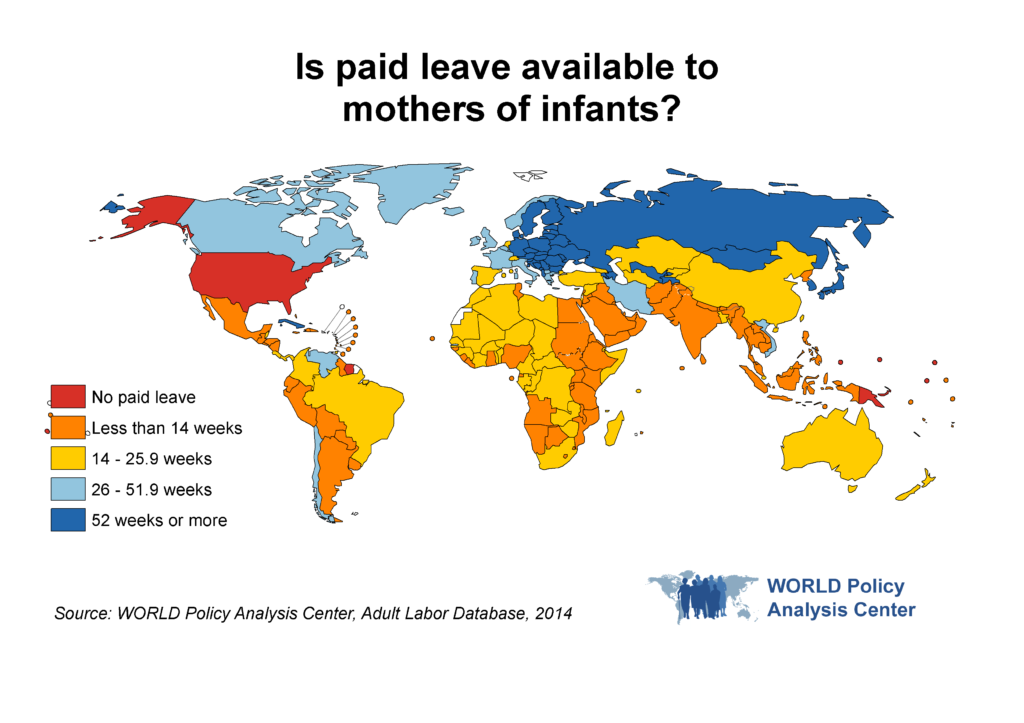
Similarly, extending paid maternal leave leads to an increase in breastfeeding duration. The WHO recommends at least six months of exclusive breastfeeding for infants to achieve the maximum health benefits. Evidence on policy impact can help us understand how much leave is needed to make a difference for infant health and evaluate how many countries are meeting this standard. In addition, for countries that cannot currently afford to provide long periods of leave, we can look at whether they nevertheless can facilitate these infant health interventions through other policies, such as paid leave for children’s health needs or paid breastfeeding breaks for working mothers.
 Focusing on the policy environment has been remarkably successful in other fields. Take education. It’s important to encourage parents to equally support their daughters and sons to complete their education. But in many settings, where parents can only afford to send one child to school, girls are more likely to be kept home than boys, whether from gender bias or from the expectation that they will have less earning potential than their brothers in adulthood. When countries make school tuition-free, however, enrollment rates soar—and the gender gap narrows substantially.
Focusing on the policy environment has been remarkably successful in other fields. Take education. It’s important to encourage parents to equally support their daughters and sons to complete their education. But in many settings, where parents can only afford to send one child to school, girls are more likely to be kept home than boys, whether from gender bias or from the expectation that they will have less earning potential than their brothers in adulthood. When countries make school tuition-free, however, enrollment rates soar—and the gender gap narrows substantially.
Since 1990, numerous countries have changed their education policies so that it’s easier for parents to send all their children to school, and global progress towards gender parity reveals that their efforts are paying off.
The same principle applies when it comes to infant and child health. The world has come a long way on infant health in the past 25 years, and we know what parents can do to improve infant health outcomes—but we need to create an environment that makes it possible for them to work, support their families, and take these steps. Paid leave is a powerful example of a policy that has the potential to strengthen infant health outcomes by supporting parents to provide the best care they can.
Comments