The human malaria parasite has developed partial resistance to every drug used to treat it, particularly the first-line treatment, ACT (artemisinin combination therapy).
In order to curb the further spread of ACT resistance, in 2010 the World Health Organization recommended that all suspected malaria cases receive a parasite-based diagnosis (rather than presumptive treatment based on external symptoms such as a fever) before issuing anti-malarial medication.
This was challenging for most local clinics because a parasite-based diagnosis relies primarily on observing blood samples under a microscope; a time consuming process that uses expensive equipment and training, which is neither readily available nor cost-effective for a small-scale health clinic.
However, rapid diagnostic tests (RDTs) have been developed that are quick, easy and cheap to use. These tests resemble pregnancy tests, with an indicator band appearing on the display when a malaria-infected blood sample is present. The RDT works by detecting antigens (an umbrella term for proteins that indicate an infection) produced by the malaria parasite, and induce a chemical reaction which causes the indicator band to fluoresce.
Between 2010 and 2015, sales of RDTs from manufacturers worldwide tripled from 90 to 270 million, and in 2015 RDTs constituted 74% of diagnostic testing used for suspected malaria cases. By reducing the number of anti-malarial medications given without first confirming the presence of the parasite, the rate of overtreatment declined, and the probability of developing anti-malarial resistance reduces.
Understanding the duration of antigen persistence is critical for correctly interpreting RDTs from recently-treated individuals
After a successful anti-malarial treatment, the malaria parasites clear from the bloodstream and the treated individual begins to feel better within a couple of days.
At this point, an issue with the use of RDTs for diagnosis purposes arises. The antigens produced by the recently-cleared malaria parasites persist in the blood after treatment for a period of time, and this duration of antigen persistence has been widely reported to be highly variable. Therefore, subsequent RDT tests can still appear positive if a recently-treated individual is tested, despite the fact that they are no longer infected with malaria.
Additional problems can occur if the individual falls ill with a fever for a second time; if the test returns positive, the clinician may assume that they have been re-infected with malaria, but the possibility exists that the individual has been infected with a non-malarial fever-causing illness (for example, dengue virus or tuberculosis) but the antigens from the previous malaria infection still persist in large enough quantities to return a positive RDT.
Understanding the duration of antigen persistence is critical for correctly interpreting RDTs from recently-treated individuals, and reduces the probability of clinicians mismanaging non-malarial fevers contributing to ACT resistance.
In a recent publication in Malaria Journal by the Malaria Atlas Project at Oxford University, the authors systematically collated studies documenting the persistence of RDT positivity after treatment, and applied a Bayesian survival model to the dataset to measure the amount of time RDTs remained positive after treatment.
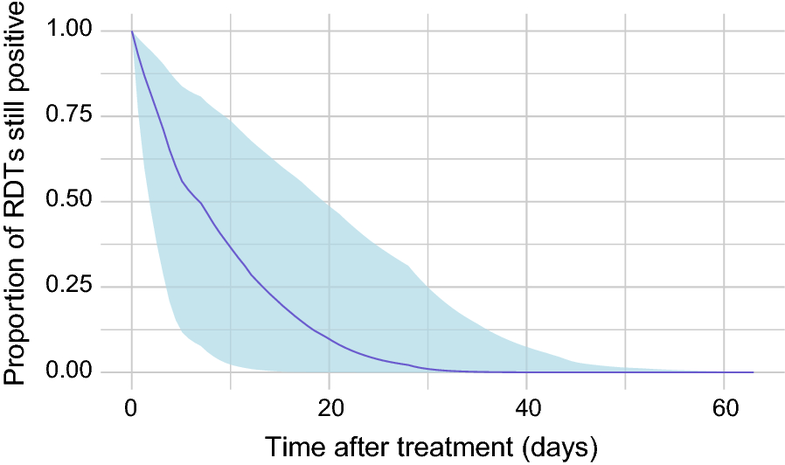
The authors found that approximately half of RDTs remained positive for more than a week after treatment, and a small fraction remained positive for more than three weeks after treatment.
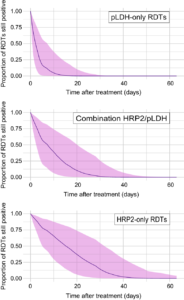
RDTs come in a variety of forms, typically testing for either or both types of malaria antigens: histidine-rich protein II (HRP2); and Plasmodium lactate dehydrogenase (pLDH) enzyme. This study found that between these two types of RDTs, HRP2-detecting RDTs showed persistent positivity for much longer than pLDH-detecting RDTs (or combination RDTs that detect both HRP2 and pLDH simultaneously) after successful anti-malarial treatment.
In addition to these findings, the study explored collated studies on the age ranges of the sampled patients, and found children experienced longer durations of persistent positivity than adult patients. This is most likely due to pediatric malaria infections frequently being associated with a higher blood parasite density, and adults in high malaria exposure areas typically develop immune responses to malaria that keeps their blood parasite density low.
The results from this study suggest that clinicians should treat positive RDT results from recently-treated patients with caution, particularly if the patient is young and the clinician only has access to RDTs that detect HRP2.
Fortunately, with malaria prevalence continuing to decrease in most areas of the world, reinfection after successful treatment is becoming less and less likely for human populations. RDTs have contributed in no small part to this development, but their correct usage is instrumental in continuing this trend. Over-diagnosis of malaria leads to over-prescription of anti-malarial drugs and a systematic mismanagement of non-malarial fevers globally. On an individual level, it is of utmost importance to provide the best diagnosis possible for a patient in order to achieve an optimal health outcome.
Comments