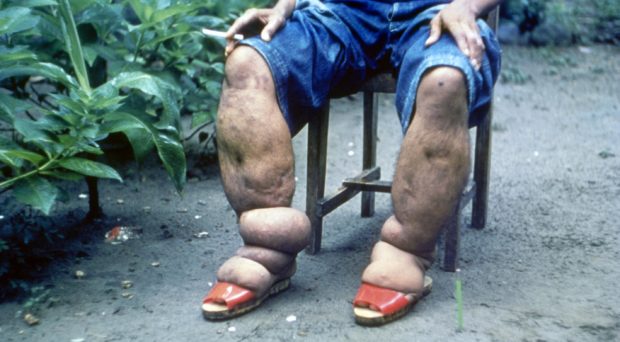
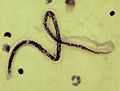
Lymphatic filariasis is a Neglected Tropical Disease that currently threatens 856 million people across 52 countries. It is usually acquired in childhood and, whilst people often remain asymptomatic on the outside, it does damage the lymphatic system. In chronic cases, it can lead to tissue swelling – commonly called elephantiasis. The majority of lymphatic filariasis cases are caused by the parasitic roundworm Wuchereria bancrofti.
The good news is that lymphatic filariasis can be eliminated by annual mass drug administration (MDA) programs. The WHO’s Global Program to Eliminate Lymphatic Filariasis (GPELF) has administered 6.7 billion treatments since 2000 and has been successful in eliminating lymphatic filariasis in 14 countries. However, 52 countries still require preventative chemotherapy and there are some regions that have not yet begun the MDA program.

Furthermore, not everyone can be part of the MDA. GPELF has deemed MDA unsuitable for certain groups such as pregnant women and children under 2 years of age. Yet Madhusmita Bal and colleagues report that filarial infection during pregnancy has serious implications on the child’s immune response and consequently its susceptibility to filarial infection.
Bal and colleagues followed 57 children up to the age of 8 to assess whether their immune responses varied over time. They measured the levels of filaria-specific IgG1, IgG2, IgG3 and IgG4 antibodies and the cytokines IL-10 (modulates immune response) and IFN-ɣ (promotes immune response to infections) in the plasma.
Children who were born to women that had lymphatic filariasis during pregnancy show a higher rate of acquisition of filarial infection than those that were not. The marked differences in the levels of the different subclasses of IgG antibody, IL-10 and IFN-ɣ between the two groups of children could explain the difference in susceptibility to infection.
Children born to women who had lymphatic filariasis during pregnancy displayed higher levels of IL-10, IgG1 and IgG4 compared to those children whose mothers were not infected during pregnancy (they showed higher levels of IFN-ɣ and IgG3). Amongst the former group of children there was also a negative correlation between IL-10 expression and IFN-ɣ levels. This ‘priming’ of the immune response began in the uterus where IL-10 and IgG4 passed from the mother to the child through the placenta. IgG3 antibodies mediate the killing of parasites whilst IgG4 is an immune modulating antibody often leading to ‘tolerance’ of parasites, therefore children of infected mothers are at a disadvantage from the time they are in the womb.
Whilst this study is limited by sample size, it does indicate the profound effect that filarial infection during pregnancy can have on the life of the child after birth. Bal and colleagues stress the importance of providing filarial treatment for young women and children in order to achieve global elimination targets, and especially call on MDA programs to ensure that women of child bearing age are targeted for prevention therapy, so that they can be free from infection when they do become pregnant.

Comments