
BMC Women’s Health – Incorporating end-users’ voices into the development of an implant for HIV prevention: a discrete choice experiment in South Africa and Zimbabwe
 AIDS-related illnesses are the top cause of death for women aged 15-49 globally, with 18.8 million women and girls currently living with HIV. Young women in sub-Saharan Africa are twice as likely as young men to get infected due to socio-cultural, economic, and political inequalities. While HIV prevention medication has come a long way, remembering to take a daily tablet can be challenging. Injectable pre-exposure prophylaxis (PrEP) offers longer lasting and more convenient protection but still requires frequent visits to the clinic, which is why implant alternatives are being tested. But would women want to use them?
AIDS-related illnesses are the top cause of death for women aged 15-49 globally, with 18.8 million women and girls currently living with HIV. Young women in sub-Saharan Africa are twice as likely as young men to get infected due to socio-cultural, economic, and political inequalities. While HIV prevention medication has come a long way, remembering to take a daily tablet can be challenging. Injectable pre-exposure prophylaxis (PrEP) offers longer lasting and more convenient protection but still requires frequent visits to the clinic, which is why implant alternatives are being tested. But would women want to use them?
A recent study published in BMC Women’s Health gathered feedback from 800 women aged 18-30 in South Africa and Zimbabwe on their implant preferences using discrete choice experiments (DCEs). DCEs are a widely used survey method in market research and health economics that allows to identify preferences for various products or services. This approach enabled the researchers to prioritize the essential attributes of the implant and explore the trade-offs that women would be willing to make. Women were presented with five attributes of hypothetical implants, which were based on prior exploratory qualitative research. These attributes included rod length, number of rods and insertion sites on the body, duration, flexibility, and biodegradability (i.e., dissolvability). The survey asked participants to choose between pairs of hypothetical implants and whether they would use the product they chose.
The study found that women prioritized a longer duration of protection (2 years over 6 months) and considered the number of insertion sites and physical flexibility of the implant as important features to ensure discretion of the implant. Biodegradability was considered the least important attribute. The authors concluded that developers should take these preferences into consideration when designing an implant that women would actually want to use.
BMC Genomics – De novo transcriptome assemblies of C3 and C4 non-model grass species reveal key differences in leaf development
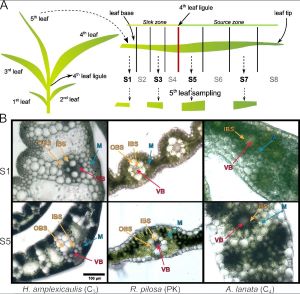
Photosynthesis is the process through which plants create sugars from light, CO2, and water. C3 photosynthesis is the most common type but is constrained by a tendency of photosynthetic enzymes to fix oxygen molecules instead of CO2. This phenomenon, known as photorespiration, squanders the plant’s energy. C4 photosynthesis, which evolved nearly 70 times in angiosperms circumvents photorespiration and lowers the rate of photosynthesis in certain environments. Intermediate species that have characteristics of both C3 and C4 photosynthesis – the so-called C3 Proto-Kranz (PK) photosynthesis – are rare but have provided valuable insights into the evolution of C4 photosynthesis. Despite decades of research, there are still many questions about the genetic changes that occurred during the evolution of C4 photosynthesis from a C3 ancestor.
In a study recently published in BMC Genomics, high-confidence protein-coding leaf transcriptomes were generated from three closely related non-model grass species in the Otachyriinae subtribe. Transcriptomes were assembled across four different leaf segments that capture different stages of development. An analysis of differentially expressed genes (DEG) found that immature segments showed a higher transcriptional dynamic than mature segments. This pattern was observed in both C4 and PK leaves, but the trend of decreasing DEG was reduced in the C3 leaf segments. Interestingly, only the C4 species maintained high levels of DEG until a later stage of development, suggesting that the C4 leaf takes more time to complete the necessary anatomical differentiation prior to the activation of the photosynthetic machinery.
The authors conclude that the developmental program in C3, PK, and C4 species is evolutionarily conserved, and that the recruitment of new pathways in C3 species may have contributed to the changes observed in C4 species. This study provides a valuable contribution to the existing genomic resources and new tools to investigate the evolution of photosynthesis.
.
BMC Medical Ethics – Equivalence of care, confidentiality, and professional independence must underpin the hospital care of individuals experiencing incarceration
 Providing healthcare for prisoners is a complex and challenging task that presents unique ethical, legal, and practical challenges. Healthcare professionals need specialized training to work with incarcerated people, balancing the responsibility of providing excellent medical care with maintaining security in the healthcare setting.
Providing healthcare for prisoners is a complex and challenging task that presents unique ethical, legal, and practical challenges. Healthcare professionals need specialized training to work with incarcerated people, balancing the responsibility of providing excellent medical care with maintaining security in the healthcare setting.
A recent debate article in BMC Medical Ethics explores the difficulties of providing hospital care that respects prisoners’ rights and dignity. While prisoners are entitled to healthcare services, the quality of these services can vary widely between countries or even facilities. The authors emphasize that following medical ethics guidelines is crucial in prison medicine, and highlight the challenges of maintaining confidentiality, professional independence, and equivalence of care in hospital settings. Healthcare professionals must ensure that security guards do not interfere with patient-provider interaction, and their independence from prison administration is necessary to minimize the risk of conflicting loyalties.
To improve healthcare for incarcerated individuals in hospitals, the authors suggest that healthcare and security staff must work together while respecting each other’s roles and responsibilities. Clear communication is vital for better health outcomes and efficient hospital functioning. Patients should also receive clear information about the rules and living conditions while in hospital to ensure compliance. Additionally, the authors recommend independent expert groups regularly monitor and accredit on-site and off-site in-patient facilities for incarcerated individuals to ensure that medical ethics guidelines are being followed.
BMC Health Services Research – Should I stay or should I go? Why nurses are leaving community nursing in the UK
 This year, the UK has been facing the biggest health worker strike actions since the beginning of the NHS, causing significant disruption of health care. With inflation at a 40-year high, health workers are demanding an increase in wages to match increased cost of living. According to the Royal College of Nursing (RCN), notoriously low pay has led to over 25,000 nurses to leave in the past year. Community nurses, who provide healthcare services to people in their homes or in community settings (nursing homes, clinics, and health centers) are particularly affected. But is low pay the only reason for this mass exodus we are witnessing?
This year, the UK has been facing the biggest health worker strike actions since the beginning of the NHS, causing significant disruption of health care. With inflation at a 40-year high, health workers are demanding an increase in wages to match increased cost of living. According to the Royal College of Nursing (RCN), notoriously low pay has led to over 25,000 nurses to leave in the past year. Community nurses, who provide healthcare services to people in their homes or in community settings (nursing homes, clinics, and health centers) are particularly affected. But is low pay the only reason for this mass exodus we are witnessing?
In a study published in BMC Health Services Research, scientists from the University of Sheffield, Division of Nursing & Midwifery, recently explored the differences in individual and organizational factors between community nurses who intend to leave and those who intend to stay in the profession. This cross-sectional online survey included questions on demographics, missed care, staffing levels, job satisfaction, and intention to leave. The survey found that 54.5% of respondents were dissatisfied with their job, and 27.6% of those who reported being dissatisfied intended to leave their job. The study identified four factors that have the highest impact on community nurses who intend to leave: excessive overtime, a reduced proportion of permanent staff, poor management and support, and poor working conditions.
The results of this study are consistent with similar research conducted in South Africa, Canada, and Saudi Arabia and reveal inherent problems in the organisational structure of health care settings. The authors suggest that policy initiatives should focus on ensuring that community nursing services have sufficient resources and funding to employ a safe and required number of staff at appropriate grades to reduce workload, burnout and increase job satisfaction.
BMC Cancer – Glycosylation spectral signatures for glioma grade discrimination using Raman spectroscopy
 Glioma is a tumor that originates in the glial cells of the brain and spinal cord and is classified based on the type of glial cell they arise from. Glioblastoma is the most common and aggressive type of glioma with an average survival time of 12-18 months after diagnosis. Tumor classification used to rely solely on histological staining, but the current gold standard also includes molecular characterization. Nevertheless, more convenient and less biased techniques are needed to ensure the correct classification and treatment of glioma.
Glioma is a tumor that originates in the glial cells of the brain and spinal cord and is classified based on the type of glial cell they arise from. Glioblastoma is the most common and aggressive type of glioma with an average survival time of 12-18 months after diagnosis. Tumor classification used to rely solely on histological staining, but the current gold standard also includes molecular characterization. Nevertheless, more convenient and less biased techniques are needed to ensure the correct classification and treatment of glioma.
A recent study published in BMC Cancer discusses the potential use of confocal Raman spectroscopy (RS) combined with machine learning for objective and label-free diagnosis of glioma. RS is a non-invasive technique that determines the vibrational modes of molecules to identify their unique fingerprint. Using RS in combination with machine learning the authors successfully discriminated glioma grades and identified biomolecular changes during glioma progression at three different levels: tissue, serum, and single cell/multicellular spheroid level.
More specifically, RS was able to detect changes in the intensity of biomolecules, including proteins, hemoglobin, DNA, collagen, lipids, and glycans. The changes in glycosylation patterns were found to be important in glioma progression and contribute to the immunosuppressive nature of the glioma micro environment. The study also shows that liquid biopsies from patient serum samples could be used for glioma diagnosis and therapeutic monitoring as a minimally invasive alternative to solid biopsies. Finally, different cell lines could be discriminated with high accuracy using RS, indicating that grade discrimination may be achievable on single live cells. The authors conclude that targeting single cells with RS could provide an additional benefit to current single-cell technologies in the era of cancer personalized medicine.
Comments