
BMC Bioinformatics – Novel deep learning model for more accurate prediction of drug-drug interaction effects
The most efficient therapy to many diseases is often the result of a combination of drugs. Administration of more than one molecule in cases of cancer, hypertension, asthma and AIDS can lead to an increase in drug efficiency and decrease in toxicity and resistance by the target cells. Nevertheless, different molecules can also interact in a detrimental way for the body. Hence the importance of being aware if multiple drugs are prescribed to patients. Different studies have been carried out, trying to foresee possible drug-drug interactions inside the body. In vivo testing is often limiting because it requires a long time to screen different compounds. In silico studies, instead, have proved to be more powerful.
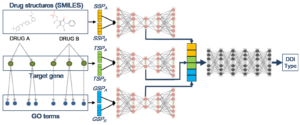
Computational methods, usually, take into account known characteristics of molecules, such as structure, target and side effects. An article published this month by Lee et al. in BMC Bioinformatics shows the formulation of a new deep learning model to predict drug-drug interaction, that takes into consideration three concepts: target similarity profiles (TSP), Gene Ontology (GO) term similarity profiles (GO term gives information about the gene function, where it acts inside the cell and in which biological process it is involved) and Structural similarity profiles (SSP). Three similarity profiles are traced for any given drug pair. These are then joined together to provide an estimation of the level of interaction between the two molecules. This approach allowed the authors to identify, with the same or greater accuracy, drug-drug interactions that were characterized using different methodologies.
BMC Cancer – Molecular features of lung adenocarcinoma in young patients
Incidence of lung cancer in the population increases with age and it is rarely diagnosed in young people. It has been shown that clinic-pathological features of lung cancer in younger and older patients are not the same. However, previous research in the field has not shown conclusive results and still remains elusive.
In this study carried by researchers of Zhejiang University (China), specimens of cancer cells from 89 young patients (35 years old or younger) with adenocarcinoma were analyzed. The majority of patients were women and only 1 in 10 were smokers.
Prognosis was also seen to vary according to the mutations involved in cancer onset.
Next-generation sequencing was used to identify the mutation of 59 cancer-related genes. The most frequently mutated genes identified were ERBB2 (Receptor tyrosine-protein kinase erbB-2) and EGFR (epidermal growth factor receptor). Fusion of ALK (Anaplastic lymphoma kinase) and ROS1 (receptor tyrosine kinase) genes was also characterized as responsible for oncogenesis. No significant correlation was seen between the mutations (or fusion) identified, the gender or the smoking habit of the patient. Overall, a prevalence of ERBB2 mutations was characterized in well/moderately differentiated tumors, while EGFR mutations and ALK fusions were identified in moderately/poorly differentiated tumors. Prognosis was also seen to vary according to the mutations involved in cancer onset.
BMC Pregnancy and Childbirth – Why rural women do not use primary health centers for pregnancy care: evidence from a qualitative study in Nigeria

Maternal mortality rates in developing countries are still unacceptable and although policies were made by local governments, around 830 women still die every day because of pregnancy or childbirth complications. 99% of these deaths happen in developing countries and they are, in most cases, preventable.
Nigeria is one of the countries with the highest maternal mortality rate, with peaks in rural areas. In 2014, the government launched a program to provide primary health care for vulnerable populations. Despite the efforts, rural pregnant women did not make use of this service and are not receiving medical support during pregnancy and delivery.
Women also reveal that often the quality of care is not adequate
A qualitative study in BMC Pregnancy and Childbirth investigated the reasons underlying women’s dangerous choice of not using the primary health care facilities provided. Discussion through focus groups allowed the authors to identify some major themes behind this trend. Participants underlined the difficulty in reaching the health centers, as paved road are non-existent and it is risky to use the bad roads available. Difficulty in obtaining a mean of transportation and distance to the facilities were also identified as important barriers.
Furthermore, participants stated that those clinics are not open at all times and taking a trip there and finding them closed discouraged them from using the health care facilities on other occasions.
Strikingly, women also reveal that often the quality of care is not adequate; there is not medication to alleviate the pain, waiting times are long, the environment is not friendly and the healthcare professionals are not supportive or competent. This, in addition to the belief that traditional medicine and divine intervention would do just as much as the staff of the health centers, pushes women to avoid seeking this type of professional help. Finally, participants also mentioned that the cost of care is arbitrary and often these facilities request patients to buy consumables from them, which can be expensive.
All things considered, this study suggests that the governmental solution to maternal mortality is still far from being adequate. Improvement in facility accessibility and in the quality of care would motivate women to rely on professional help during pregnancy. However, much work still needs to be done in this direction.
BMC Palliative care – Designing and developing a co-produced theoretical and evidence-based online support for family caregivers of people with dementia at the end of life

The majority of people with dementia live in the community but receive care mostly from family members or friends. Caring for a loved person affected by this condition can be extremely challenging, especially with the progression of the disease and towards end of life.
Researchers from the University College of London designed and developed an online palliative care support website, targeting real problems of carers of people with dementia at the end of life. Among the negative effects of taking care of a relative with dementia are depression, poor physical health and poor quality of life. Researchers are positive that this tool will help carers in their role and help to improve their overall well-being.
BMC Musculoskeletal Disorders – Corticosteroid injection for plantar heel pain: a systematic review and meta-analysis
Heel pain caused by plantar fasciitis can be insistent and impair daily activities, such as walking or running. Around 7% of the population suffers from this condition. In many cases, rest or change of habits can be sufficient to relieve the symptoms with time. However, if symptoms persist, it can be necessary to resort to different approaches, such as physiotherapy or Corticosteroid injections as they help lessen pain and inflammation. It is still unclear why Corticosteroid injections are prescribed so often, since evidence of their mode of action are still lacking.
The Corticosteroid injections would act as a placebo
A systematic review published in BMC Musculoskeletal Disorders gathered together trials and studies on the topic and elucidated in which occasions injections are effective and when they are wrongly prescribed. The review showed that Corticosteroid injections prove to be effective in the short term, in comparison to autologous blood injection, orthotics or physiotherapy. However, in the long term, platelet-rich plasma or dry needling seem to have better results. Therefore, the Corticosteroid injections would act as a placebo. Remarkably, the effect of the steroid injections seems, therefore, minimal. Further clinical trials could provide us with a better understanding of the most effective ways of treatment for this condition.
Comments