
Music during cesarean section can reduce stress and anxiety in new mothers
Cesarean section is a common surgery that, like most surgical procedures, can cause stress and anxiety in patients. Stress and anxiety in women undergoing cesarean section is especially concerning due to negative effects on post-operative recovery, lactation, and newborn development. More non-pharmacological treatments are needed to reduce stress and anxiety in pregnant women.
Music has long been considered to have stress-reducing effects, and numerous trials have shown that playing music during the surgical process reduces pain and anxiety in patients undergoing a variety of surgical procedures. Although there have been a few studies on music during cesarean section, there is no strong evidence of an effect on validated or objective measures of stress and anxiety of patients. Therefore, Hepp et al. carried out a randomized controlled trial to examine if music during cesarean section reduces both validated patient-reported and objective measures of stress and anxiety.

Three hundred and four patients were randomized to hear music from their choice of genre or no music during standard cesarean surgery. Both groups had high self-reported anxiety before the start of the procedure, but the group that heard music reported a significantly greater reduction in anxiety at the end of the procedure. Measurement of a stress hormone at the end of the procedure showed that stress sensation during surgery was significantly lower in the group that heard music.
Together, these results show that playing music during surgery is a relatively easy way to reduce stress and anxiety in new mothers giving birth by cesarean surgery.
Can treatment and care practices influence normal birth outcomes?
Previous studies have suggested that the use of medical interventions during labor and birth has slowly increased over the course of the last two decades in over 20 developed countries. Although medical interventions can be beneficial to mothers and their newborns, they do pose additional risks. As such, new policies and reforms have been implemented internationally in favor of normal birth, which is defined as an unassisted vaginal birth without labor induction, epidural, anesthesia, or episiotomy. Despite the increased interest in facilitating normal birth, few studies have assessed the factors that inhibit it. This study aimed to evaluate both the modifiable and non-modifiable factors influencing the outcome of normal birth.
The authors, Prosser et al., obtained data from the Having a Baby in Queensland Survey. The original survey included all women who gave birth between 2011 and 2012 in Queensland, Australia and evaluated women’s maternity care experiences. From this data, the authors determined that the non-modifiable factors that reduced the likelihood of normal birth included gestational diabetes, high blood pressure, previous cesarean section, the number of previous births, age, and later-term pregnancies. The leading modifiable factors that contributed to increased rates of normal birth included continuity of care through labor, freedom of movement, and a non-supine position.
The authors also assessed the model of care and found that midwifery-led care (both public and private), GP shared care and standard public care resulted in the highest rates of normal birth while private obstetrics care resulted in the lowest rates of normal birth within the study sample. Interestingly, these results also account for both obstetric and social risk factors, leading the authors to argue that these disparities might be a result of the philosophical differences between the two models of perinatal care.
Overall, the authors concluded that treatment and care practices can influence normal birth outcomes and normal birth may increase with the appropriate facilitation.
Breastfeeding experience among obese women – challenges and how to overcome them
It is well known that “breast is best” and that breastfeeding is beneficial to both mothers and infants, with increased duration of breastfeeding providing increased benefits. However, many women face challenges in initiation and/or continuation of breastfeeding for a wide variety of reasons. One group that has been shown to have a lower rate and duration of breastfeeding is mothers with obesity. These women may face barriers which include complications during delivery delaying the initiation of breastfeeding, physical discomfort, and reduced body confidence.
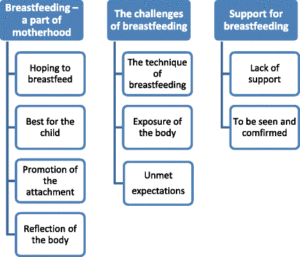
Ing-Marie Claesson and colleagues conducted a qualitative study focusing on 11 obese breastfeeding women in Sweden in order to understand their points of view, which is crucial to developing effective ways to support these women. Although some women had reservations, most intended to breastfeed, viewing it as an integral and natural part of motherhood.
The participants identified three categories of challenges. First, there were difficulties in finding a position that worked both for their own bodily comfort and their infant’s ability to nurse. Some women felt that infants had more difficulty nursing from their larger breasts. Second, the need to expose at least some part of their bodies in order to breastfeed discouraged some of the women, especially from breastfeeding in public. This was linked to low overall self-esteem, which was affected by being obese. Lastly, the unexpected difficulties in breastfeeding led to frustration and disappointment, which in some cases led to giving up.
The women also discussed the support they did or did not receive from healthcare providers. Some participants felt that the focus on the infant’s weight gain led to a pressure to switch to formula. Other participants recalled that support from healthcare providers who did not focus on their obesity increased their confidence and strengthened them as breastfeeding mothers. These experiences highlight the need for individualized support that helps women with obesity overcome the practical difficulties of breastfeeding without the focus being on the mother’s weight.
Eating Disorders and Pregnancy: what are the barriers for identification during the perinatal period?
Eating disorders (EDs) can affect up to eight percent of pregnant women and are associated with an increased risk of adverse outcomes. Pregnant women suffering from Anorexia Nervosa face risks such as premature birth, miscarriage, and low birth weight, while pregnant women suffering from Binge Eating disorder face increased risk for delivering a baby with a higher birth weight. Due to these risks, early identification of EDs is necessary for tailoring antenatal care needs. In this study, the obstacles of disclosing and identifying EDs were evaluated from the perspective of both pregnant women and health care professionals.
Bye et al., found that although women reported an overall reduction in eating disorder symptoms during pregnancy, over half of the participants experienced some symptoms, most commonly binge eating and restricting calories. Despite these symptoms, only 26% disclosed to a health care professional. The authors then developed five themes based on interviews conducted with women who did not disclose their symptoms: stigma, lack of opportunity, preference for self-management, current ED symptomatology, and illness awareness.

After surveying pregnant women, Bye et al. conducted a focus group with healthcare students and professionals, including both midwives and health visitors. Many of the healthcare providers felt that they lacked adequate knowledge on EDs in pregnancy because it wasn’t included in their training at all or training was limited. Some also thought that this contributed to the lack of knowledge of the relevant policies and management guidelines for EDs.
The authors concluded that the leading factor inhibiting disclosure amongst pregnant women was stigma. Similarly, healthcare students and professionals felt they were ill-equipped to help those they had suspected might have an ED. As a result, the authors argue that improvements in eating disorder education is needed amongst prenatal healthcare providers to give them more confidence in the identification of eating disorders, decrease stigma, and lead to better guidelines for how to address the disorder. See our blog post by the authors of this study where they discuss specific activities that could raise both professional and public awareness about eating disorders in order to improve pregnancy outcomes and patient experiences.
Comments