Harlequin Ichthyosis is a severe autosomal recessive congenital disease that is caused by a mutation in the ABCA12 gene. Neonates often present with distinctive physical traits such as cracked plates of thickened skin and irregular facial features. It is a rare disease and the incidence is estimated to be about 1 in 300,000 live births. The disease is commonly fatal, with infants often failing to survive for up to a week.
The availability and access to medical care for this disease differs greatly between countries, especially between developing and developed countries. In the summer of 2018, a baby with Harlequin Ichthyosis was born in a hospital in Northern Nigeria. Reports from local news networks and internet blogs state that on sight of the newborn, the child’s mother and the majority of the medical staff fled the delivery room.
If the mother of the affected baby in Nigeria had been aware of her child’s disease before birth … she may have been less distressed upon sight of her newborn.
Following the stampede, a diagnosis given by a doctor familiar with the disease seemed belated and insufficient to reassure the fleeing mother and medical staff. As expected, this case drew public curiosity and speculation, not only because of the striking physical appearance of the child but also due to the pervasive ignorance of the disease even among medical professionals.
In the United Kingdom, the response to the disease is qualitatively different as evident in the experience of the UK patient. The patient was not her mother’s first child to be affected by the disease. Although she knows little about the circumstances of her older siblings’ birth, she imagines that the medical staff extended necessary support to her parents regarding the management of the disease. It is possible that her mother may have received genetic counselling after the birth of her affected children, and pre-natal diagnosis before the patient’s own birth, making her better prepared emotionally and psychologically to care for her child.
Quite possibly, if the mother of the affected baby in Nigeria had been aware of her child’s disease before birth, through pre-natal screening or diagnosis, she may have been less distressed upon sight of her newborn.
Pre-natal diagnosis
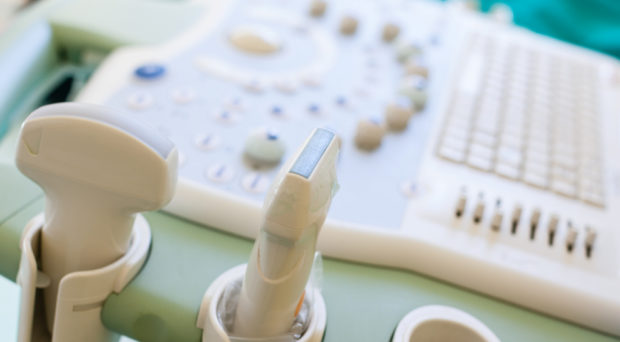
Pre-natal diagnosis of Harlequin Ichthyosis would require taking fetal skin biopsies by fetoscopy. Alternatively, and perhaps preferably for the mother, 3D or 4D sonography could be used to reach a probable diagnosis based on physical characteristics.
These techniques would normally only be used in cases with pregnant women who have previously had children with the disease. However, there have been instances where abnormal findings in 2D sonography have led to the use of 3D sonography for more detailed examination, and ultimately to the diagnosis of the disease.
In the NHS, although 2D sonography is the standard routine scan, 3D or 4D ultrasound scanning would usually incur an extra cost. In a developing nation like Nigeria, there is an acute lack of general medical equipment and much less specialized equipment required for the pre-natal diagnosis of a rare disease like Harlequin Ichthyosis. According to The Point Nigeria, the vast majority of the tertiary healthcare facilities in the country have inadequate equipment to diagnose and treat serious illnesses.
Even in the event that equipment was readily available, there are still a number of barriers to accessing pre-natal care in Nigeria. The practice of purdah, a stringent form of wife seclusion, , particularly in Northern Nigeria has been a notable impediment to accessing care. According to Wall, women who are subject to the strict version of this practice are hardly ever seen in public.
Another possible contributing factor is the low level of public awareness and education about the need for pre-natal examinations. Research has found that better maternal education correlates with an increased use of maternal healthcare facilities. It could therefore be argued that if the Nigerian Government invested more in maternal healthcare education, there could be an increase in the number of patients who make use of pre-natal facilities, and consequent improvement in early diagnosis.
Managing Harlequin Ichthyosis
The management of Harlequin Ichthyosis is complex and requires the joint expertise of a multidisciplinary team. Although in the past, infants with Harlequin Ichthyosis usually fail to live beyond the neonatal period, advancement in intensive care and the use of an integrated approach have increased survival rates.
The long-term management of the disease is more straightforward than in the neonatal period and usually involves taking routine baths and using hydrating skincare products in order to make sure that the skin is adequately moisturized. Because patients who survive past childhood are usually able to lead relatively normal lives, it can be said that the most crucial period of management is in infancy.
It is clear that for medical professionals, effective management of a rare disease involves a continuous learning cycle.
As with many rare diseases, medical professionals are still learning how best to manage Harlequin Ichthyosis. In 2014, a query was submitted to the United Kingdom’s National Institute for Health and Care Excellence (NICE) about the optimal physical environment for infants born with the disease. The question came about because reputable systematic reviews had shown that there was irresolution on treatment outcomes.
It is clear that for medical professionals, effective management of a rare disease involves a continuous learning cycle. The UK patient praised the doctor that treated her as she grew up with his willingness to learn every day, review research, and apply new knowledge to her treatment. She stated that, unfortunately, at some point she had to move to a new GP practice, and she was disappointed that her new doctor did not know much about the disease. This highlights how continuity of care can mean so much to a patient with a rare disease.
In Nigeria, there are a myriad of challenges to the management of rare diseases. The lack of medical staff contributes greatly to this. Despite having an approximate population of nearly 191 million people, as of 2010 there were estimated to only be about 0.4 physicians and 1.60 nurses and midwives per 1000 people. Coupled with the alarmingly high child mortality rate in the country, one can only imagine what this could mean for children with Harlequin Ichthyosis.
Because a large number of births in the country happen at home and in the care of traditional birth attendants, the management of the disease would also depend on whether the patient is actually ever brought into a hospital system for post-natal diagnosis or care. Unlike the UK patient who gratefully remarked that she had received free healthcare all her life, some parents in Nigeria would not be able to afford the associated cost of healthcare.
Social stigma is also an important contributing factor because parents may isolate the child in fear of the community’s reactions. Families with striking skin diseases are usually considered to be outcasts. In traditional African societies, it is commonly believed that rare and serious illnesses are not merely a chance or genetic occurrence, but rather, they are due to spiritual affliction or occur as punishment by deities for disobeying traditions. Generally, victims of these traditional beliefs are shunned and isolated by community members. It is likely that this was a factor in the flight of both the mother and medical staff in the Northern Nigeria case.
How can we do better?
The case in Nigeria gives cause for concern. It underscores the need for higher ethical standards among medical professionals. Even in the midst of a dire lack of resources, their conduct can still make the difference in whether a patient lives or dies. Had the medical personnel maintained calm and professional despite the newborn’s unusual physical appearance, the mother might have been reassured and offered relevant information and counselling.
When the UK patient was informed about the case in Nigeria, she attributed it to ignorance, saying, “I understand that it was not a pretty sight, but the child was still a human being just like them”. Governments and global health institutions around the world must do more to promote knowledge and provide capacity for the management and care of rare diseases like Harlequin Ichthyosis. Regardless of their health status, no newborn should ever have to endure the unimaginable agony of abandonment by their own mother and medical staff. These are the very people that should be there to offer love, care and support.
Comments