
As the weather heats up here in the UK, you may have seen the recent news coverage of research which found that hot temperatures increase the risk of gestational diabetes. Following on from our blog last year where we looked at diabetes in general, in this blog we focus on the studies registered at ISRCTN that aim to predict, prevent and treat gestational diabetes.
Gestational diabetes is a type of diabetes that develops during pregnancy and usually disappears after giving birth. It affects about 6% of all pregnant women. It occurs when the body can’t produce enough insulin to meet the extra needs due to pregnancy. Most women with gestational diabetes have otherwise normal pregnancies, but it can cause problems leading to difficulties during delivery.
Put to the test
Women are usually screened for gestational diabetes using the oral glucose tolerance test (OCTT) around their 24th to 28th weeks of pregnancy. This involves a blood test before eating or drinking, drinking a sugary drink and then giving another blood sample to see how the body handles sugar.
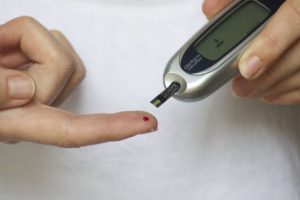
While the need for screening is broadly accepted, there is a debate as to what form this should take, with some advocating universal screening of all pregnant women and others selective screening of high-risk subgroups only. Risk factors include having a body mass index (BMI) above 30, previously having a baby who weighed 4.5 kg or more at birth, and having had gestational diabetes in a previous pregnancy.
This study at Galway University Hospitals (Ireland) compared screening all pregnant women in primary care with screening in secondary care. It was hoped that uptake rates would be improved if screening was offered in a setting more accessible to the patient, but uptake was found to be poor.
Would it be possible to detect gestational diabetes earlier in pregnancy? Researchers at Southend Hospital (UK) are carrying out a study to find out whether it would be possible to complete an OGTT in the first trimester of pregnancy (between 11 and 14 weeks of pregnancy).
Earlier detection of gestational diabetes could lead to earlier treatment, but what does treatment involve?
An ongoing study in Greece is also looking at whether other blood markers such as adiponectin and leptin can also be used as early indicators for developing gestational diabetes. Earlier detection of gestational diabetes could lead to earlier treatment, but what does treatment involve?
OptiMUM nutrition
After being diagnosed, just like with type 2 diabetes, the first step is to look at diet and lifestyle. Making changes to the diet can help control blood sugar levels. For example, the Irish OptiMUM Nutrition study is testing an online dietary intervention for all pregnant women, and those who are diagnosed with gestational diabetes are given specific diet and lifestyle advice in line with guidelines.

The Mediterranean diet is also a recurring theme, with three Spanish studies, one completed and two ongoing, testing diets rich in olive oil, nuts, fruit and vegetables, and avoiding red or processed meat, fast food and sweets. The WELLBABE study at Newcastle University (UK) tested a rather more drastic diet – a calorie reduction to 1,200 kcal for 4 weeks – to see whether this reduced liver fat and improved the blood sugar control of pregnant women with gestational diabetes.
Physical activity lowers your blood sugar level, so regular exercise can be an effective way to manage gestational diabetes, with the HEALTHY study recommending three exercise classes per week and the PEARs study also offering a specially designed smartphone application for extra motivation.

Women affected by gestational diabetes are also at an increased risk of developing type 2 diabetes later in life. A study at the National University of Ireland assessed an intensive lifestyle intervention program, Croí MyAction, for reducing the risks of developing type 2 diabetes among women with previous gestational diabetes (registered at ISRCTN, protocol in Trials). However, participant recruitment has proved to be far more difficult than initially anticipated, as discussed in BMC Medical Research Methodology.
Treatments and supplements
If their blood sugar level is not under control after a week or two of dieting and exercise, patients may be offered medication such as metformin. Metformin reduces the amount of glucose the liver releases into the bloodstream and makes the body’s cells more responsive to insulin.
The Mild GDM study at St Mary’s Hospital (UK) tested whether metformin should also be given to women with lower blood sugar levels. This follows from recent updates to guidelines suggesting that the threshold used to diagnose gestational diabetes should be lowered.
Another drug currently under investigation is liraglutide, which mimics the action of the natural hormone GLP-1 and triggers the release of insulin. It is hoped that daily injections of liraglutide combined with an intensive lifestyle change program will prevent gestational diabetes in women who have previously had it or who are obese without being diabetic.

A variety of supplements have also have been tested to see whether they can prevent or treat gestational diabetes, including inositol, vitamin D, omega-3 fatty acids, and probiotics, although the latter were found to not reduce blood sugar levels.
The take home message
It is estimated that there are 415 million people living with diabetes worldwide – 1 in 11 of the world’s adult population – and this is expected to rise to 642 million by 2040. Given the links between gestational diabetes and type 2 diabetes, more research is definitely needed to prevent and treat diabetes in all its forms.
Comments