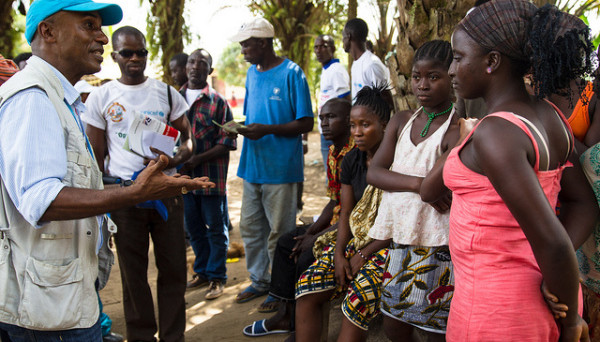
What do you do?
As a medical anthropologist in West Africa, I teach, research and do advocacy on community-based responses to epidemic and pandemic events, post-conflict reconstruction and humanitarian intervention in Guinea, Liberia, Sierra Leone and Côte d’Ivoire.
What roles have anthropologists traditionally played in response to epidemics?
In books and journals, academic anthropologists have drawn attention to traditional practices, local health cultures and practices of care giving. In epidemics and other humanitarian emergencies, applied anthropologists have played a major role in working with international agencies to conduct research about the impacts of epidemics on local populations and to learn how communities are responding.
During Ebola, anthropologists were often asked to take part in health communications – persuading local communities to change practices in order to prevent the spread of epidemics, respond appropriately, and challenge myths or suspicions around disease spread. They helped encourage cooperation with governments or humanitarian and medical organizations.
We need to develop new ways for anthropologists and epidemic responders to work with each other.
Unfortunately, applied anthropologists’ recommendations have been marginalized within the organizations that hired them, while academic anthropologists have, at times, been seen as sniping from the side-lines in the midst of crises. We need to develop new ways for anthropologists and epidemic responders to work with each other.
How could anthropologists contribute more effectively in the future?
Social science concerns need to be treated on a level with clinical and public health concerns. In the current model of epidemic response, when an outbreak occurs, experts plan a response, and anthropologists are brought in later to address challenges confronted during implementation. Anthropologists need to be integrated into epidemic response much earlier on, during planning phases.
Second, communications around epidemic events need to be switched from a one-way, top-down model to one that allows for open dialogue between local communities, national governments and international agencies.
Local communities, especially in low- and middle-income countries, often have extraordinary capacities for understanding rapidly changing local health conditions like those that take place during epidemics. They have many mechanisms for taking on board new information and changing local practices quickly, and a clear investment in doing so. Anthropologists can play a role in facilitating communication, but the real focus of epidemic response should be local communities.
How can Western healthcare workers work effectively with communities during epidemics?
Today, in most parts of the world, traditional healers and healing practices coexist with a widespread acceptance of conventional medicine. Local populations often have very sophisticated understandings of Western pharmaceuticals, interventions and research.
Western healthcare workers are vulnerable to media representations of epidemic hotspots as healthcare ‘hearts of darkness’. To be effective, they need to engage with traditional health workers as healthcare experts who are concerned with more than just the epidemic response.

Traditional health workers are often also concerned – far more than Western healthcare workers – with managing the long-term implications of the epidemic, overall morbidity and mortality, and impacts on health systems and environments. Western healthcare workers are often very narrowly focused on managing epidemic cases, to the exclusion of other health issues.
When Western workers encounter local resistance, they should note that these concerns reflect a complex set of concerns involving the credibility of the response, the legitimacy of the government, environmental and economic concerns, and local experiences with past epidemics as much as they reflect attitudes towards specific diseases like Ebola or Zika.
How can we ensure that research is done ethically and sensitively but still rapidly enough to control disease in communities affected by certain outbreaks?
Too many resources are being redirected towards replicating existing social science research during emergencies, rather than using existing research to inform epidemic scenarios.
Too many resources are being redirected towards replicating existing social science research during emergencies, rather than using existing research to inform epidemic scenarios. Consider Zika. There’s an enormous amount of anthropological research that has been done on the interaction between national health systems and reproductive health across Latin America, particularly on ethically and legally sensitive issues like childbearing, terminating pregnancy and child mortality.
We need to use what we have better and direct resources towards filling in knowledge gaps that are of vital concern in the present moment.
What’s the one change you’d make in the world to make us better prepared for epidemics?
In order to make epidemic response faster, more sensitive, more effective and more evidence-based, qualitative research (based on qualities that can be observed but not measured numerically) must be given equal standing with quantitative research (based on numbers and things that can be measured).
Local communities must be given a leading role in shaping and changing epidemic response policy. Establishing a permanent platform for anthropological response to epidemic and humanitarian emergencies would go a long way towards achieving those goals.
Comments