
The mobile phone has rapidly morphed into a device with multiple uses and is set to become a useful tool for the diagnosis of parasitic diseases. Their use as simple microscopes has been explored for several years. For example, in 2011 a group from the University of California, Davies described the development of two attachments that transform a smart phone into a 350x microscope (with post-processing) or a visible-light spectrophotometer. DIY instructions for doing the same were also posted in 2011.
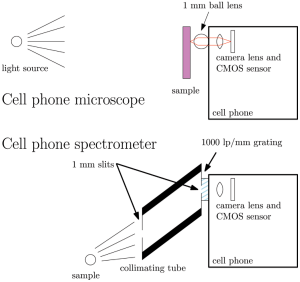
In Tanzania researchers have assembled a home-made version of the Californian device that cost about $8 and used it to look for helminth eggs in stool samples, and earlier this year Schistosome eggs in urine samples have been reported to be detected using a mobile phone and a Foldscope in Ghana.
More recently, members of a team at Pacific Northwest National Laboratory have developed a simple and extremely cheap microscope using a mobile phone and a glass bead. As demonstrated in their video a glass bead is held in place over the camera lens of the phone by a simple device made using a 3D printer. They claim the materials required to convert a phone into a microscope cost less than $1, making it ideal for use in low income settings, though this does not, of course, include the 3D printer or the smart phone. Detailed instructions, including a source for the various sizes of beads that produce magnification of 100x, 350x and 1000x and 3D printer software to print the holder that takes the bead and a microscope slide are provided free of charge. So far this device does not seem to have been tested in the field for identification of such things as helminth eggs or malaria infected erythrocytes; an exciting project for a BugBitten reader to take on!
The low tech approach
Meanwhile, researchers at the University of Houston have developed a lens made from a plastic-like polymer, polydimethylsiloxane. Droplets of the honey-like substance harden when heated and the curvature of the droplets makes them good lenses. With manufacturing costs at $3 per lens this is another cheap option and, as the droplet is fixed to the camera lens with an adhesive, no special holder is required. However with a magnification of only 120x its uses for parasite identification may be more limited.
A more sophisticated use of mobile phones for parasite identification has, however, been developed and recently tested in Cameroon.
iPhones for Loa loa detection
Filarial roundworms (nematodes) are the cause of diseases such as elephantiasis (lymphatic filariasis), Loa loa filariasis and river blindness (onchocerciasis). The adult females shed tiny thread-like larvae known as microfilariae into the blood stream or skin and these are passed on in a blood meal to mosquitoes, horseflies or blackflies respectively.
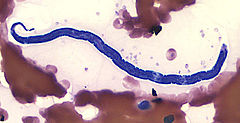
Mass treatment of populations in areas endemic for filarial nematode infections, using ivermectin alone, or in combination with albendazole, is the mainstay of strategies aimed at elimination of filariasis. Although this is very effective for treatment of onchocerciasis and lymphatic filariasis, ivermectin can cause severe side effects in Loa loa-infected people who have circulating levels of 30,000 microfilariae / ml and above. These include potentially fatal encephalopathy caused by dying microfilariae, Thus, in areas where were these worms are co-endemic mass drug administration has been suspended, hindering elimination campaigns.
A way round this problem would be to identify people with heavy Loa loa infections and exclude them from the mass drug treatment, a strategy called test and NOT treat, but quantitative screening requires a trained microscopist to detect and count microfilariae in thick blood smears and it is slow and not practical in many field settings. This is where the mobile phone comes in.
The CellScope Loa
An international team led by Daniel Fletcher and Thomas Nutman have developed a method of quantifying the number of live microfilariae in a 200 µm thin layer of blood based on the displacement of red blood cells caused by their wriggling movement. Their latest publication describes a prototype, known as CellScope Loa, which represents a considerable improvement on their original design. It performed extremely well by comparison with manual gold standard microscopy performed by trained technicians when tested on thick blood smears from patients in Cameroon (correlation factor (r) = 0.99). It was 94% specific and 100% sensitive for people with above the threshold of microfilariae load that could cause severe adverse effects after ivermectin treatment.
The CellScope Loa consists of a 3D printed lid that holds an iPhone and lens module and a 3D printed base that houses a movable carriage to house a blood loaded capillary tube, an LED array to provide illumination, control electronics and a USP port to supply power to the device. Blood taken from a finger prick is loaded into a capillary tube and inserted into the carriage.
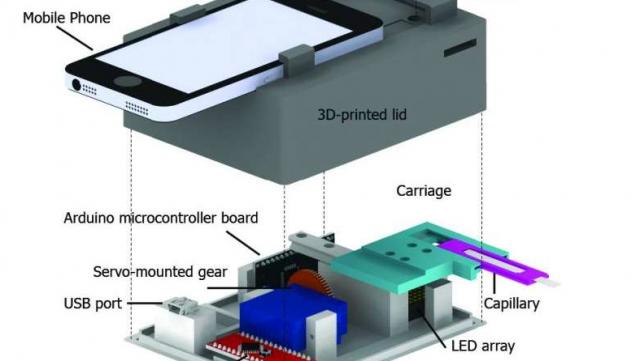
Five second movies are taken at 5 different points as the capillary tube is moved along past the lens and an image-processing algorithm locates and counts microfilariae by detecting movement of erythrocytes caused by wriggling microfilariae. The total time taken to collect a blood sample and analyse it is only 3 minutes.
Loa loa microfilariae can be distinguished from those of the other major filarial worms in Cameroon because the peak circulation of Loa loa microfilariae in periphery vessels occurs between 10am and 2pm whereas circulation of Wuchereria bancrofti microfilariae(one of the causative agents of lymphatic filariasis) peaks at night and Onchocerca microfilariae (the causative agents of river blindness) are usually in the skin or lymphatic system.
The development of CellScope Loa is a remarkable achievement made possible as result of collaboration with engineers, clinicians and local health workers. Although this is only a prototype the researchers are confident that few regulatory barriers would prevent its use as part of mass drug administration campaigns in Central Africa. It is to be hoped that aspects of scale up for manufacturing, including cost reduction, will be developed rapidly.
Reflection
It is clear that the combination of a mobile phone camera and magnifying lens offers opportunities for pictures or videos taken in remote locations by untrained workers to be immediately sent to diagnostic laboratories or analysed on the spot, thereby speeding up effective treatment or enhancing research projects. I look forward to reading about further advances of this technology.

quite educative on the subject