
Distribution and symmetrical patellofemoral pain patterns as revealed by high-resolution 3D body mapping: a cross-sectional study
Describing pain symptoms can be a difficult task. Patellofemoral pain (PFP) is a broad term that is used to describe pain and stiffness in the knee, around the patella and the kneecap, making it difficult to perform everyday activities. This affects a large number of adolescents and young adults. Causes of PFP can originate from several components of the knee, but patients experiencing pain are often unaware of the cause of their knee pain and therefore communicating PFP can be as general as pointing to the area around the knee.
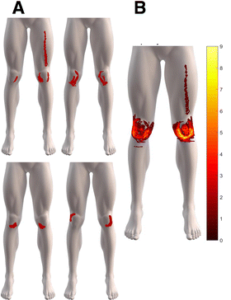
In an attempt to overcome this issue, Shellie A. Boudreau developed a new system which allows patients to communicate pain through visual representation using high resolution 3D body mapping in conjunction with 2D line drawings. Together with Micheal Rathleff, PFP expert, and colleagues they have used this technique to acquire 2D drawings of pain patterns and also symmetrical pain patterns in adolescents and young adults with PFP.
Results found that the majority of complaints were common in the lower peripatellar region. The vast majority of subjects presenting with bilateral knee pain demonstrated symmetrical knee pain patterns. This study provides a window into the possible pain patterns that may exist within PFP and provides a rationale to further explore the significance of these knee pain patterns in larger cohorts.
Clinical classification in low back pain: best-evidence diagnostic rules based on systematic reviews
 Low back pain is a common problem that affects most people at some point in their life and can stem from several parts of the lumbar spine, including the intervertebral discs, sacroiliac joints, facet joints, bone, muscles, nerve roots, muscles, peripheral nerve tissue, and central nervous system sensitization. So how we do we classify diagnosis and treatment strategies for the different sub-groups of low back pain?
Low back pain is a common problem that affects most people at some point in their life and can stem from several parts of the lumbar spine, including the intervertebral discs, sacroiliac joints, facet joints, bone, muscles, nerve roots, muscles, peripheral nerve tissue, and central nervous system sensitization. So how we do we classify diagnosis and treatment strategies for the different sub-groups of low back pain?
With better evidence to identify patho-anatomy, Tom Petersen, Mark Laslett and Carsten Juhl published a systematic review of diagnostic accuracy studies in an attempt to develop evidence-based Clinical Diagnostic Rules (CDRs) for identifying common sources and causes of low back pain. To identify the most common patho-anatomical disorders in the lumbar spine for use in clinical practice, Petersen’s group identified 64 studies to successfully construct promising CDRs for symptomatic intervertebral disc, sacroiliac joint, spondylolisthesis, disc herniation with nerve root involvement, and spinal stenosis.
In some of these categories sufficient evidence was found to recommend a CDR, whilst other categories had preliminary evidence and will require further studies. Therefore the findings of this study suggest that evidence-based clinical diagnosis can potentially reduce the need for invasive or expensive diagnostic methods; however, further research is necessary to evaluate these findings in a primary care setting.
Good Life with osteoArthritis in Denmark (GLA:D™): evidence-based education and supervised neuromuscular exercise delivered by certified physiotherapists nationwide
 Osteoarthritis is considered one of the leading causes of disability, and substantial evidence increasingly supports the use of exercise as a first line of treatment for the disease. In this study, Soren Skou and Ewa Roos from the University of Southern Denmark have evaluated the aims of Good Life with osteoArthritis in Denmark (GLA:D), which is a training scheme established in 2013 to reduce hip/knee pain caused by osteoarthritis, reduce the number of people taking painkillers, improve physical function, improve quality of life and reduce the number of patients on sick leave.
Osteoarthritis is considered one of the leading causes of disability, and substantial evidence increasingly supports the use of exercise as a first line of treatment for the disease. In this study, Soren Skou and Ewa Roos from the University of Southern Denmark have evaluated the aims of Good Life with osteoArthritis in Denmark (GLA:D), which is a training scheme established in 2013 to reduce hip/knee pain caused by osteoarthritis, reduce the number of people taking painkillers, improve physical function, improve quality of life and reduce the number of patients on sick leave.
A total of 9,825 participants from the GLA:D registry were included and the findings show that education and supervised exercise improved pain intensity and quality of life. Moreover, the results show that fewer patients took painkillers and were on sick leave following the scheme. Given its positive impact, GLA:D has now been established nationwide and emphasizes the importance of exercise as a lifestyle change to improve general health and quality of life.
The transverse abdominal muscle is excessively active during active straight leg raising in pregnancy-related posterior pelvic girdle pain: an observational study
 Pelvic girdle pain (PGP) is a condition that commonly affects the pelvic joints during pregnancy, and causes pain and discomfort. To investigate the contraction patterns of muscles in the pelvis, Jan Mens and Annelies Pool-Goudzwaard carried out a cross-sectional observational study to examine the thickness of the transverse abdominal muscle (TrA) using ultrasound imaging in women with PGP during active straight leg raising (ASLR). In their cohort, PGP started during pregnancy in 84% of the participants and 3 weeks post-delivery in 16% of the participants.
Pelvic girdle pain (PGP) is a condition that commonly affects the pelvic joints during pregnancy, and causes pain and discomfort. To investigate the contraction patterns of muscles in the pelvis, Jan Mens and Annelies Pool-Goudzwaard carried out a cross-sectional observational study to examine the thickness of the transverse abdominal muscle (TrA) using ultrasound imaging in women with PGP during active straight leg raising (ASLR). In their cohort, PGP started during pregnancy in 84% of the participants and 3 weeks post-delivery in 16% of the participants.
The authors observed no significant differences in the mean TrA thickness at rest between women with and without PGP; however, interestingly, a significant excessive contraction of the TrA was observed during ASLR in patients with PGP. Therefore these findings appear to suggest that exercise may not be the solution for patients with long-lasting pregnancy-related PGP.
Individuals’ explanations for their persistent or recurrent low back pain: a cross-sectional survey
 It has been estimated that globally approximately 40% of people experience low back pain. Although most research investigates the physical causes of low back pain, Setchell and colleagues from the School of Health and Rehabilitation Sciences, Australia, took a novel approach to explore individual belief systems regarding what causes low back pain to persist.
It has been estimated that globally approximately 40% of people experience low back pain. Although most research investigates the physical causes of low back pain, Setchell and colleagues from the School of Health and Rehabilitation Sciences, Australia, took a novel approach to explore individual belief systems regarding what causes low back pain to persist.
The study indicated that persistent low back pain is perceived as structural with “no mechanical fix”, permanent and complex, and often described as very negative. Interestingly, it also appears that these beliefs about low back pain stemmed overwhelmingly from health professionals and the internet as a source of understanding of their LBP. The findings of this study highlight the importance of understanding underlying causes of low back pain, perhaps shifting the thinking within healthcare and looking beyond singular causes.
Specific or general exercise strategy for subacromial impingement syndrome–does it matter? A systematic literature review and meta analysis
 Subacromial impingement syndrome (SIS) accounts for up to 50-70% of shoulder pain and occurs when the tendons of the rotator cuff become trapped and compressed during shoulder movement. Using a systematic review and meta-analysis approach, Alison Shire and colleagues identified six randomized control trials (a total of 231 patients) that used specific exercise strategies to treat patients experiencing symptoms of SIS. They evaluated whether implementing specific exercises resulted in a more superior effect, as determined by improvements in pain, function and quality of life (QoL), compared with general exercises in a resistance training program.
Subacromial impingement syndrome (SIS) accounts for up to 50-70% of shoulder pain and occurs when the tendons of the rotator cuff become trapped and compressed during shoulder movement. Using a systematic review and meta-analysis approach, Alison Shire and colleagues identified six randomized control trials (a total of 231 patients) that used specific exercise strategies to treat patients experiencing symptoms of SIS. They evaluated whether implementing specific exercises resulted in a more superior effect, as determined by improvements in pain, function and quality of life (QoL), compared with general exercises in a resistance training program.
Interestingly, the results showed no significant difference to support the use of specific exercises over general exercises in the outcome measures in patients experiencing SIS. Low quality and inconsistent data were indicated as one of the main reasons for not being able to detect differences, and the authors provide recommendations for the design of future trials to address this issue.
Comments