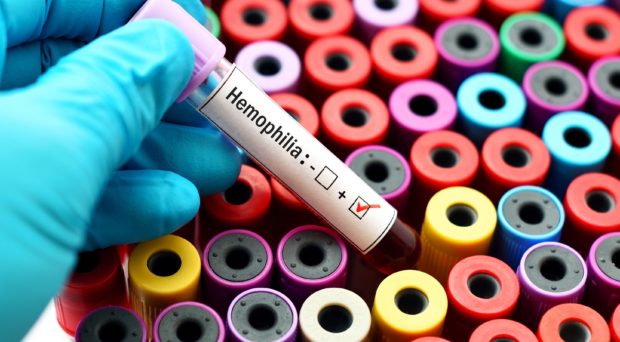
Bleeding disorders often arise when there is a problem with the clotting process. Hemostasis is the process by which the body arrests bleeding via the damaged blood vessels and it involves three major steps: vasoconstriction, formation of a temporary blockage (platelet plug), and blood coagulation. When injury causes a blood vessel to bleed, vascular constriction limits the flow of blood to the injured area. The vessel wall injury, via a series of reactions, triggers the attachment and activation of platelets which aggregates at the site of injury. Platelets adhere to collagen which becomes exposed in the endothelial cell lining of blood vessels at the site of injury creating the platelet plug. Initial platelet adhesion is to von Willebrand factor, a major component in the blood coagulation process. Coagulation factor VIII circulates in the blood stream in an inactive form when bound to von Willebrand factor.
When injury to a blood vessel occurs, factor VIII becomes activated and separates from von Willebrand factor and interacts with factor IX, another coagulation factor. This interaction sets off a chain of additional chemical reactions that form a blood clot. Activation of a sequence of blood clotting factors generates thrombin which converts fibrinogen to fibrin. Fibrin mesh is then produced around the hemostatic plug in turn strengthening the clot.
von Willebrand disease is the most common type of bleeding disorder and is usually less severe in comparison to other bleeding disorders. It occurs due to decrease in or malfunctioning von Willebrand factor activity which ultimately affects the hemostasis process and slows the formation of blood clots resulting in prolonged bleeding episodes. It is estimated that around 1% of the world’s population is affected by von Willebrand disease.
Hemophilia is a bleeding disorder where the blood is unable to clot properly. It can lead to spontaneous bleeding as well as bleeding after injury or surgery. Those who suffer from hemophilia can bleed longer than usual, although not faster. There are two main types of hemophilia which are hemophilia A and hemophilia B with the former being the most common of the two. Although it is the most common type of hemophilia, it is a rare condition and it affects about one in every 10,000 males whilst hemophilia B affects one in every 50,000 males. The condition arises when a mutation or change occurs in one of the genes that provide instructions for making the clotting factor proteins needed to form a blood clot thus resulting in reduced production or deficiency of the respective clotting factor. The F8 gene and F9 gene, both situated on the X-chromosome, provides the instructions for producing coagulation factors VIII and IX respectively. A mutation in the F8 gene causes hemophilia A whilst a mutation in the F9 gene results in hemophilia B. Suffers therefore have low levels of either clotting factor VIII or IX and the severity is determined by the level of the factor in the blood.
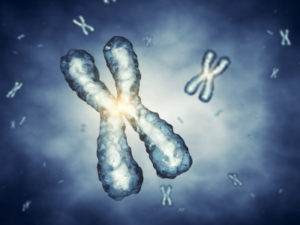
Due to the sex-linkage of the disorder, the prominence amongst male is greater than in females. Although the disorder mainly affects males, females can be carriers of the affected gene and experience symptoms. Hemophilia is a hereditary bleeding disorder. However, it has been found that in about a third of new diagnoses there is no previous family history. This could be due to new or spontaneous genetic mutations. It is estimated that worldwide, around 400,000 people are living with hemophilia with 20,000 of these cases present in the United States and around 6,000 in the United Kingdom. Main symptoms can include a prolonged bleeding from cuts, a tendency to bruise easily especially in early childhood, and bleeding into joints and muscles causing pain, swelling, and stiffness which can result in joint deformity and limitation of movement if left untreated. Women can experience prolonged or heavy menstrual bleeding (menorrhagia) and the excessive blood loss can lead to anemia resulting in weakness and fatigue. In general, during the process of ovulation, women can develop simple/ functional ovarian cysts which are small and not usually problematic. However, it has been found that carriers of hemophilia are more likely to experience significant bleeding during ovulation and have a greater risk of bleeding into these simple cysts which then become hemorrhagic ovarian cysts that can cause considerable pain and may require urgent medical intervention. Women with hemophilia are also more likely to have postpartum bleeding following childbirth.
It has been reported that of the 400,000 people living with hemophilia worldwide, only around 25% receive adequate treatment. The recommended treatment plan for hemophilia depends on the severity of the condition. The main treatment for hemophilia is replacement therapy whereby the missing clotting factor is slowly dripped or injected into a vein. A CDC- sponsored randomised clinical trial found that regular treatment to prevent bleeding (prophylaxis with recombinant factor VIII) was effective in preventing joint damage and decreased the frequency of joint and other hemorrhages in young boys with severe hemophilia. The children who were treated on a regular basis also had less evidence of joint damage by 6 years of age than did those who were treated after a bleed had commenced.
However, factor replacement therapy has its limitations as it has been found that approximately 25–30% of people with severe hemophilia A and 1–5% of people with severe hemophilia B develop an antibody (inhibitor) to the treatment which causes major complications.
There are a number of new therapies under development which include gene therapy where researchers are investigating means by which the faulty genes that cause bleeding disorders such as hemophilia can be corrected. Research is also being conducted to design and implement interventions that will help combat complications. Although there is no cure for hemophilia, with the right treatment, care, and lifestyle changes, those who suffer from hemophilia can lead fulfilled lives.
If you are interested in reading more on this topic, please visit the BMC Hematology website. The journal welcomes submissions on non-malignant and malignant hematological diseases, hemostasis and thrombosis, hematopoiesis, stem cells and transplantation. Related papers which detail basic, experimental and clinical research can be submitted to the journal here.
The following are a few of the interesting picks and recent publications in the journal covering the area of hemophilia:
Generic and disease-specific quality of life among youth and young men with Hemophilia in Canada
Prophylaxis in older Canadian adults with hemophilia A: lessons and more questions
Comments